Learning Outcomes
After completing this text course, participants will be able to:
- Describe various studies that discuss the impact of hearing aids on tinnitus perception and listening effort.
- Discuss various evaluation methods commonly used to assess listening effort.
- Explain how the following variables affect tinnitus outcomes: hearing aid user experience, objectively verified hearing aids, hearing aid wear time, tinnitus maskers and counseling.
Introduction
Hearing aids are primarily designed to improve audibility for those with hearing loss as a way to facilitate communication and increase awareness of environmental sounds. However, research increasingly shows that hearing aids offer further secondary benefits beyond these primary effects. For example, there is substantial discussion regarding the effects of hearing aids on cognition and whether amplification affects cognitive decline. Retrospective correlational and prospective randomized controlled trials appear to indicate that, at least for some individuals at higher risk for dementia, hearing aids may reduce cognitive decline, or that risk of decline is higher for people who do not wear hearing aids (e.g., Lin et al., 2023; Cantuaria et al., 2024).
Two additional secondary benefits of hearing aid use that have been discussed in the literature are (1) tinnitus relief and (2) reduced listening effort. The purpose of this review is to assess the evidence concerning hearing aid effects on tinnitus and listening effort. These outcomes highlight the multifaceted role of hearing aids not only as devices to improve auditory perception, but also as a therapeutic intervention that can enhance overall well-being and ease communication difficulties across a variety of listening environments. Investigating these broader effects offers a more comprehensive understanding of the clinical value of hearing aids, moving beyond the traditional focus on audiometric thresholds to encompass functional and psychosocial outcomes. Additionally, recent efforts argue for extending hearing aid candidacy to a broader clinical population, including individuals with minimal hearing loss or no audiometric loss but with other auditory complaints (Roup et al., 2018; Mealings et al., 2024). This expanded perspective of what should constitute a good hearing aid candidate underscores the importance of clarifying secondary benefits of hearing aids such as the effects on tinnitus and listening effort.
Tinnitus
Tinnitus affects a significant proportion of the population and is often associated with distress and reduced quality of life, making it a key focus of ongoing research. In 2022, it was estimated that tinnitus affected 740 million adults globally (Jarach et al., 2022). In the U.S., estimates show 1 in 10 adults report tinnitus (Bhatt et al., 2016). A growing body of evidence indicates that hearing aids can effectively reduce tinnitus-related distress and improve quality of life. Two main methodologies have been used in the literature for assessing tinnitus. One includes behavioral assessments such as tinnitus pitch matching or loudness matching (National Guideline Center, 2020), and the second involves subjective self-reported measures such as the Tinnitus Functional Index (TFI; Meikle et al., 2012), or the Tinnitus Handicap Inventory (THI; Newman et al., 1996), which are the two most widely used self-report measures (Fernandez et al., 2022). Numerous other validated and reliable questionnaires also are available for assessing tinnitus outcomes, each characterized by certain advantages and limitations. Employing multiple questionnaires may therefore provide the most comprehensive understanding of the adverse impact of tinnitus on an individual (Theodoroff, 2020). The TFI addresses the following areas: intrusiveness, sense of control, cognition, sleep, auditory, relaxation, quality of life, and emotional distress, and can be interpreted on a scale from not a problem (0-17) to a very big problem (73-100), while the THI categories include functional (e.g. problems with day-to-day difficulties like concentration, sleep, etc.), emotional, and catastrophic areas (e.g. loss of control, fear of disease, etc.) and can be interpreted on a scale from slight or no handicap (score of 0-16) to catastrophic handicap (score of 78-100). A visual analogue scale has been used with some success as a tinnitus screener that assesses the perceived loudness of tinnitus, its annoyance, the distress it is causing, and how well the patient is coping (Raj-Koziak et al., 2018). Depending on what outcome measure is administered, and perhaps depending on the perspective of the researchers, various terms have been used to characterize tinnitus severity, such as tinnitus-related quality of life, bothersomeness, distress, annoyance, etc.
There is evidence in the literature that supports the positive effects of using hearing aids for tinnitus management (e.g. for scoping review, see Shekhawat et al., 2013). In addition to this evidence base, formal clinical practice guidelines have also been developed (Department of Veterans Affairs & Department of Defense, 2024). These guidelines were created by a multidisciplinary workgroup of experts that created five levels of recommendations: recommends, suggests, neither for or against, suggest against, or recommend against. Guidelines published in 2024 “suggest” hearing aids for tinnitus management in adults with hearing loss. It is important to consider study limitations such as sample size, potential introduced bias, and whether a study is a randomized control trial; however, review papers have also argued that systematic reviews that are too strict in their inclusion criteria may skew conclusions to state inconclusive results of the effectiveness of hearing aids or maskers when clinical effectiveness has been shown (Henry et al., 2022). For example, Kaniewska and Refaie (2024) found that among 20 patients with moderate hearing loss, most patients showed varying degrees of improvements in tinnitus-related quality of life from using hearing aids as evaluated by the THI, while a few showed no improvement or worsening THI score. The most clinically significant gains were observed in patients with slight to mild tinnitus handicap, while those reporting persistent sleep difficulties experienced less benefit, suggesting that comorbid factors may influence treatment efficacy. Their findings also highlight that hearing aids prescribed primarily for routine hearing loss can positively affect tinnitus perception and overall well-being.
A study using the Japanese version of the TFI found some subscales showed improvements for 10 out of 21 participants, while other areas of tinnitus’ impact on participants showed no improvement (Noguchi et al., 2021). These researchers found significant reduction in tinnitus scores 12 months post-hearing aid fitting in the scales of intrusiveness, sense of control, sleep and emotional subscales, however, no difference was noted for cognitive, auditory, relaxation, and quality of life subscales. Others have shown that hearing aids can meaningfully reduce tinnitus in patients with normal hearing as well (Waechter et al., 2023).
Studies have also examined whether traditionally fit hearing aids versus hearing aids used in combination with tinnitus maskers have differing results. Waechter et al. (2025), in a randomized controlled multicenter study, found significant reduction in tinnitus distress, as measured by a reduction of 13 or more points on the TFI, three months after the hearing aid fitting with a sample of 108 individuals. The researchers tested various types of tinnitus therapy in these hearing aid users including increased gain at the tinnitus pitch and notch therapy, where the gain at the tinnitus pitch was eliminated, and they found no significant difference compared to objectively fit hearing aids. In fact, those fit with conventional hearing aid amplification had better speech intelligibility outcomes compared to those fit with increased gain or notch therapy at the tinnitus pitch.
When following participants with hearing aids with and without tinnitus maskers, Henry et al. (2015) found that 26 out of 30 participants experienced a meaningful reduction in tinnitus both when fitted with hearing aids incorporating broadband noise as a tinnitus masker and when using hearing aids alone; however, users with maskers in their devices scored 6.4 points better on their TFI than the control group (hearing aids only). In a similar outcome, a randomized clinical trial found a clinically significant reduction in tinnitus (> 13-point reduction on the TFI) in 67% of hearing aid-only users, and 79% of users with hearing aids with a sound generator (Henry et al., 2017). Other factors such as a multi-disciplinary team to address tinnitus, follow-up visits, and patient education and counseling regarding tinnitus may also influence levels of tinnitus reduction whether patients have hearing aids, ear-level masker devices, or no devices at all (Folmer & Carroll, 2006). When it comes to using tinnitus maskers with hearing aids, others found mixed results in patient tinnitus outcomes of improved symptoms, worsened symptoms, or no change in symptoms (Villatte et al., 2025).
Hearing aid wear time appears to play a crucial role in outcomes. In patients with chronic hearing loss and tinnitus, hearing aid use successfully suppressed tinnitus symptoms after at least six months of consistent use at an average of 7.2 hours (± 3) in the first month and up to 9.1 hours (± 3) per day by the sixth month (Simonetti et al., 2022). This aligns with Boecking et al. (2022), who demonstrated that hearing aid use time partially mediated treatment-related improvement in tinnitus related distress, with an optimal hearing use time of 9.5-10.5 hours per day. Others found that daily hearing aid use time in patients with high-frequency hearing loss positively correlated with a reduction in TFI results in users with gain extending into the high frequencies (Joergensen et al., 2022). The consistent finding that benefits emerge after months of sustained device use further highlights the importance of early intervention and long-term management strategies (e.g. Simonetti et al., 2022).
There is some consideration of hearing aid programming effect on tinnitus. In a meta-analysis, Waechter and Jönsson (2022) compared the differences in questionnaires such as the THI, TFI, and tinnitus severity index (TSI) scores in patients fit with objective hearing aid verification (e.g. real-ear) and those fit with unverified hearing aids. They found a greater reduction in TFI scores in hearing aid users fit with objectively verified devices after 12 months. Joergensen et al., (2022) found that broadband amplification (125 Hz-10 kHz) resulted in a reduced THI and TFI scores as compared to band-limited amplification (125Hz to 3-4kHz). This study also noted a significant reduction in tinnitus annoyance and loudness using a visual analogue scale of 0-100, where baseline scores were 50.65 ± 5.32 and 54.5 ± 4.2 points respectively at baseline, which reduced to 31.4 ± 3.5 and 45.1 ± 3.0 points after 12 weeks with broadband amplification.
Another consideration is whether hearing aid experience affects tinnitus relief. It appears that after a 12-week trial with hearing aids, both new and experienced hearing aid users showed a reduction in TFI scores. This helps to conclude that properly fit hearing aids are a helpful approach to tinnitus relief regardless of hearing aid experience level (Sanders et al., 2023). Finally, there are an array of other individual patient factors that may influence tinnitus outcomes, including age, tinnitus duration, hearing ability, and perceived location of tinnitus within the head or ears amongst other factors. These factors should be considered in continued research guiding tinnitus management decisions (Theodoroff et al., 2014).
In addition to amplification alone, evidence supports the combined use of counseling with hearing aids. Lee et al. (2022) conducted a retrospective study of 116 patients, half of whom received both counseling and hearing aids, while the other half received counseling alone. Using the THI and the Satisfaction with Amplification in Daily Life (SADL) questionnaire, they observed significant reductions in THI scores six months after intervention in the group fitted with hearing aids, whereas only some non-significant improvement was seen in patients who received counseling alone. They found that visual analogue scale scores showed a significant reduction in tinnitus loudness for both groups. This could suggest that amplification not only improves audibility but may increase the efficacy of counseling-based tinnitus management strategies. Even those with only mild hearing loss experienced meaningful tinnitus relief when hearing aid use was combined with individualized tinnitus counseling (Lee et al., 2022).
In general, the literature supports an average reduction in tinnitus-related complaints with hearing aid use. However, it is clear that not all individuals experience these secondary benefits. The heterogeneity of outcome measures used across studies creates a challenge in interpreting data on a larger scale. Higher levels of evidence will help to clarify the extent of hearing aid effects on tinnitus measures across individuals and comorbidities, and determine the important components of additional intervention beyond hearing aids (e.g., maskers, counseling, etc.).
Listening Effort
The human brain has a remarkable ability to separate out a competing noise from the intended signal. However, hearing impairment reduces both the audibility and quality of sound perception and causes difficulty for listeners (Moore, 1996). The amount of difficulty for a listener is challenging to measure. However, recent interest in this subject has led to research on a concept frequently referred to as listening effort, often defined as “the deliberate allocation of mental resources to overcome obstacles in goal pursuit when carrying out a [listening] task” (Pichora-Fuller et al., 2016). Importantly, it has been shown that hearing impairment increases effort exerted by the listener in both adults (Ohlenforst et al., 2017; Zekveld et al., 2011) and children (Hicks & Tharpe, 2002; McGarrigle et al., 2019). However, results vary across studies, perhaps due to varying methods.
Three main types of methods have been employed to measure listening effort: (1) self-report, (2) behavior, and (3) physiology. Self-report measures consist of closed set questionnaires and judgements of effort by the participant during experimental listening tasks (e.g. visual analog scales). Behavioral measures typically involve a dual-task paradigm in which the primary task is a type of speech recognition task. Accuracy or reaction time on a secondary task is then used to measure listening effort. Secondary tasks often involve memory, visual recognition, or tactile recognition tasks (McGarrigle et al., 2014). This method follows the presumption that cognitive resources are finite and distributed between tasks (Wingfield, 2016). If more “effort” is given to the primary task, either accuracy will decrease or reaction time will increase on the secondary task. Using this framework, performance on the secondary task is taken as a measure of how much listening effort was used in the primary task (McGarrigle et al., 2014; Pichora-Fuller et al., 2016). Finally, physiological measures record changes in the activity of the nervous system as a task is being performed. As the task increases in difficulty, any systematic physiological change is ascribed to listening effort. Common physiological measures include functional magnetic resonance imaging (fMRI), electroencephalography (EEG), event-related potentials (ERPs), skin conductance, and pupillometry (McGarrigle et al., 2014).
Although their main purpose is to improve speech audibility, hearing aids may provide important benefits in reducing listening effort. Ohlenforst et al. (2017) reviewed numerous studies that demonstrated that hearing aids have been shown to reduce listening effort, using all three methodologies mentioned above. More recently, Holman et al. (2021) compared self-report outcomes in two groups of 53 adults with similar hearing losses. Subjective listening effort before and after fitting the treatment group with hearing aids was measured with the Listening Effort Assessment Questionnaire (EAS; Alhanbali et al., 2017). The treatment group reported significantly decreased listening effort compared to the control group post-fitting. In a non-peer reviewed preprint by Gianakas et al. (2024), school-age children with hearing loss performed a dual-task paradigm in the unaided and aided condition. The primary task assessed sentence recognition at the child’s measured SNR70, meaning the signal-to-noise ratio where the child could accurately repeat the sentence 70% of the time. The secondary task was a visual recognition task in which the child would identify a target color as quickly as possible. The researchers found that reaction times were significantly shorter when in the aided condition. Vaisberg et al. sought to measure neural correlates of listening effort with functional near-infrared spectroscopy (fNIRS). They examined the difference in oxygenation of the pre-frontal cortex of 30 adult hearing aid users with and without hearing aids. The listening task involved repeating the final word in low context sentences from the revised speech perception in noise test (R-SPIN; Bilger et al., 1984). Wearing hearing aids resulted in less oxygenation of the pre-frontal cortex, implying less effort. They also observed that when the listening situation became more challenging with poorer SNR, participants reported greater subjective listening effort. Conversely, other recent studies have shown contrasting results using one or more methods of measuring listening effort, finding no significant differences between aided and unaided conditions (e.g., Blümer et al., 2024; Hussein et al., 2022; Nguyen et al., 2024). Some studies have specifically examined the possible benefits of certain hearing aid features on listening effort. Enabling noise reduction algorithms and directional processing in hearing aids has been demonstrated to reduce listening effort compared to when these features were disabled (Dong et al., 2024; Fiedler et al., 2021; Picou et al., 2017; Sarampalis et al., 2009; Valderrama et al., 2025).
Listening effort is an area of concern, because it can lead to listening fatigue, or fatigue resulting from the continued application of effort during difficult listening tasks (Pichora-Fuller et al., 2016). Listening fatigue can either be measured as a subjective feeling or as a performance decrement (Hornsby et al., 2016). The concept of listening fatigue is supported by Nachtegaal et al. (2009), who found that poorer hearing thresholds were associated with a greater need for recovery after work and that poorer hearing was associated with lower self-rated productivity at work (Nachtegaal et al., 2012). Listening fatigue can greatly affect a person’s quality of life, including work performance, family life, and social relationships (Blümer et al., 2024; Hornsby et al., 2016).
Overall, strong evidence exists to support the concept of listening effort and the role of hearing aids in alleviating it. However, additional research in this area is needed to establish greater standardization and consistency. Due to the various methodologies used, comparison across studies can be challenging. Within-study comparisons do not always produce consistent results; for instance, subjective and physiological measures of listening effort may reveal little or no correspondence between the two. These discrepancies do not dismiss these measures but may indicate that different assessment methods tap into distinct dimensions of listening effort, or alternatively, into related cognitive processes (Ohlenforst et al., 2017).
Summary and Conclusion
The primary purpose of hearing aids is to improve audibility for those with hearing loss. For decades, improving performance in background noise and other complex listening environments has become another critical focus of hearing aid manufacturers. There seems to be an increased research interest in recent years, however, regarding the secondary effects of hearing aids, such as effects on tinnitus ratings and listening effort, which we have addressed in this review. Table 1 provides key resources that may be helpful for the inquiring audiologist.
Although continued tinnitus research is necessary, amplification with hearing aids represents a promising and evidence-based treatment strategy. As the literature shows, hearing aids can play an integral role in tinnitus treatment, extending beyond their primary function of restoring audibility. Hearing aids may alleviate tinnitus perception, reduce tinnitus-related distress, and improve quality of life for patients with a wide range of hearing abilities, including those with only mild impairment or normal hearing. Future research should continue to explore individual differences in treatment response and examine the interactions between amplification, tinnitus therapy, psychological factors, and counseling approaches. Such studies will help refine clinical best practices and improve outcomes for individuals living with tinnitus.
The concept of listening effort has also become an important consideration when treating hearing loss. At the present time, however, empirical evidence describing and measuring the concept is lacking. Taken together, the existing evidence appears to support the general reduction of effort for hearing aid users. In order for knowledge of listening effort to advance, clear definitions and conceptual frameworks for listening effort and related subjects are imperative. Standardization of outcome measures is also needed to introduce inter-study comparisons and replication of results. This will lead to application of results to clinical processes and promote better patient outcomes.
Table 1 includes select key articles on tinnitus and listening effort for more information. 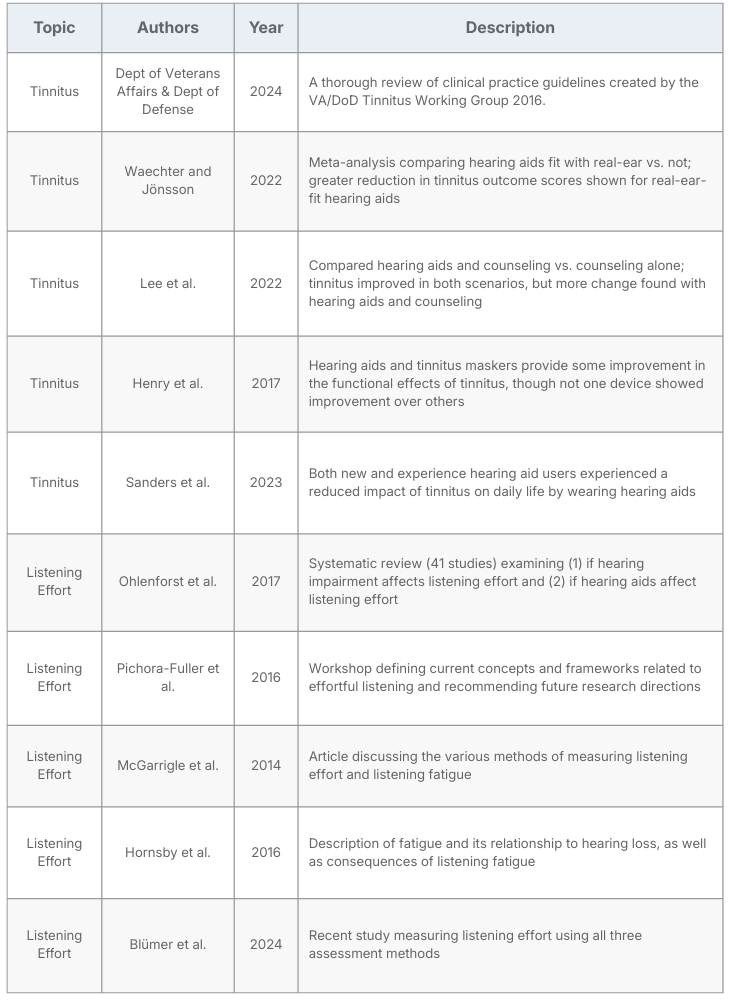
Table 1. Select articles on tinnitus and listening effort. Click here for a PDF version.
References
Alhanbali, S., Dawes, P., Lloyd, S., & Munro, K. J. (2017). Self-reported listening-related effort and fatigue in hearing-impaired adults. Ear and Hearing, 38(1), e39–e48. https://doi.org/10.1097/AUD.0000000000000361
Bhatt, J. M., Lin, H. W., & Bhattacharyya, N. (2016). Prevalence, severity, exposures, and treatment patterns of tinnitus in the United States. JAMA Otolaryngology–Head & Neck Surgery, 142(10), 959–965. https://doi.org/10.1001/jamaoto.2016.1700
Bilger, R. C., Nuetzel, J. M., Rabinowitz, W. M., & Rzeczkowski, C. (1984). Standardization of a test of speech perception in noise. Journal of Speech, Language, and Hearing Research, 27(1), 32–48. https://doi.org/10.1044/jshr.2701.32
Blümer, M., Heeren, J., Mirkovic, B., Latzel, M., Gordon, C., Crowhen, D., Meis, M., Wagener, K., & Schulte, M. (2024). The impact of hearing aids on listening effort and listening-related fatigue—Investigations in a virtual realistic listening environment. Trends in Hearing, 28. https://doi.org/10.1177/23312165241265199
Boecking, B., Psatha, S., Nyamaa, A., Dettling-Papargyris, J., Funk, C., Oppel, K., Brueggemann, P., Rose, M., & Mazurek, B. (2022). Hearing aid use time is causally influenced by psychological parameters in mildly distressed patients with chronic tinnitus and mild-to-moderate hearing loss. Journal of Clinical Medicine, 11(19), 5869. https://doi.org/10.3390/jcm11195869
Cantuaria, M. L., Pedersen, E. R., Waldorff, F. B., Wermuth, L., Pedersen, K. M., Poulsen, A. H., Raaschou-Nielsen, O., Sørensen, M., & Schmidt, J. H. (2024). Hearing loss, hearing aid use, and risk of dementia in older adults. JAMA Otolaryngology–Head & Neck Surgery, 150(2), 157–164. https://doi.org/10.1001/jamaoto.2023.3509
Department of Veterans Affairs & Department of Defense. (2024). VA/DOD clinical practice guidelines: Tinnitus. VA/DoD Health Quality. https://www.healthquality.va.gov/guidelines/CD/tinnitus/
Dong, R., Liu, P., Tian, X., Wang, Y., Chen, Y., Zhang, J., Yang, L., Zhao, S., Guan, J., & Wang, S. (2024). Influences of noise reduction on speech intelligibility, listening effort, and sound quality among adults with severe to profound hearing loss. Frontiers in Neuroscience, 18. https://doi.org/10.3389/fnins.2024.1407775
Fernández, M., Cuesta, M., Sanz, R., & Cobo, P. (2022). Comparison of Tinnitus Handicap Inventory and Tinnitus Functional Index as treatment outcomes. Audiology Research, 13(1), 23–31. https://doi.org/10.3390/audiolres13010003
Fiedler, L., Seifi Ala, T., Graversen, C., Alickovic, E., Lunner, T., & Wendt, D. (2021). Hearing aid noise reduction lowers the sustained listening effort during continuous speech in noise—A combined pupillometry and EEG study. Ear and Hearing, 42(6), 1590–1601. https://doi.org/10.1097/AUD.0000000000001050
Folmer, R. L., & Carroll, J. R. (2006). Long-term effectiveness of ear-level devices for tinnitus. Otolaryngology–Head and Neck Surgery, 134(1), 132–137. https://doi.org/10.1016/j.otohns.2005.09.030
Gianakas, S. P., Wiseman, K. B., & Walker, E. (2024). Hearing aids reduce listening effort in school-age children who are hard of hearing. OSF Preprints. https://doi.org/10.31219/osf.io/f5mku
Henry, J. A., Carlson, K. F., Theodoroff, S., & Folmer, R. L. (2022). Reevaluating the use of sound therapy for tinnitus management: Perspectives on relevant systematic reviews. Journal of Speech, Language, and Hearing Research, 65(6), 2327–2342. https://doi.org/10.1044/2022_JSLHR-21-00668
Henry, J. A., Frederick, M., Sell, S., Griest, S., & Abrams, H. (2015). Validation of a novel combination hearing aid and tinnitus therapy device. Ear and Hearing, 36(1), 42–52. https://doi.org/10.1097/AUD.0000000000000093
Henry, J. A., McMillan, G., Dann, S., Bennett, K., Griest, S., Theodoroff, S., Silverman, S. P., Whichard, S., & Saunders, G. (2017). Tinnitus management: Randomized controlled trial comparing extended-wear hearing aids, conventional hearing aids, and combination instruments. Journal of the American Academy of Audiology, 28(6), 546–561. https://doi.org/10.3766/jaaa.16067
Hicks, C. B., & Tharpe, A. M. (2002). Listening effort and fatigue in school-age children with and without hearing loss. Journal of Speech, Language, and Hearing Research, 45(3), 573–584. https://doi.org/10.1044/10924388(2002/046
Holman, J. A., Drummond, A., & Naylor, G. (2021). Hearing aids reduce daily-life fatigue and increase social activity: A longitudinal study. Trends in Hearing, 25. https://doi.org/10.1177/23312165211052786
Hornsby, B. W. Y., Naylor, G., & Bess, F. H. (2016). A taxonomy of fatigue concepts and their relation to hearing loss. Ear and Hearing, 37(Suppl 1), 136S–144S. https://doi.org/10.1097/AUD.0000000000000289
Hussein, A. B., Lasheen, R. M., Emara, A. A., & El Mahallawi, T. (2022). Listening effort in patients with sensorineural hearing loss with and without hearing aids. The Egyptian Journal of Otolaryngology, 38(1), 99. https://doi.org/10.1186/s43163-022-00288-w
Jarach, C. M., Lugo, A., Scala, M., van den Brandt, P. A., Cederroth, C. R., Odone, A., Garavello, W., Schlee, W., Langguth, B., & Gallus, S. (2022). Global prevalence and incidence of tinnitus: A systematic review and meta-analysis. JAMA Neurology, 79(9), 888–900. https://doi.org/10.1001/jamaneurol.2022.2189
Joergensen, M. L., Hyvärinen, P., Caporali, S., & Dau, T. (2022). Broadband amplification as tinnitus treatment. Brain Sciences, 12(6), 719. https://doi.org/10.3390/brainsci12060719
Kaniewska, E., & Refaie, A. E. (2024). What is an impact of hearing aids primarily fitted for presbyacusis on quality of life in patients complaining of tinnitus: A pilot study. The Egyptian Journal of Otolaryngology, 40(1), 124. https://doi.org/10.1186/s43163-024-00692-4
Lee, H. J., Kang, D. W., Yeo, S. G., & Kim, S. H. (2022). Hearing aid effects and satisfaction in patients with tinnitus. Journal of Clinical Medicine, 11(4), 1096. https://doi.org/10.3390/jcm11041096
Lin, F. R., Pike, J. R., Albert, M. S., Arnold, M., Burgard, S., Chisolm, T., Couper, D., Deal, J. A., Goman, A. M., Glynn, N. W., Gmelin, T., Gravens-Mueller, L., Hayden, K. M., Huang, A. R., Knopman, D., Mitchell, C. M., Mosley, T., Pankow, J. S., Reed, N. S., … Coresh, J. (2023). Hearing intervention versus health education control to reduce cognitive decline in older adults with hearing loss in the USA (ACHIEVE): A multicentre, randomised controlled trial. The Lancet, 402(10404), 786–797. https://doi.org/10.1016/S0140-6736(23)01406-X
McGarrigle, R., Gustafson, S. J., Hornsby, B. W. Y., & Bess, F. H. (2019). Behavioral measures of listening effort in school-age children: Examining the effects of signal-to-noise ratio, hearing loss, and amplification. Ear and Hearing, 40(2), 381–392. https://doi.org/10.1097/AUD.0000000000000623
McGarrigle, R., Munro, K. J., Dawes, P., Stewart, A. J., Moore, D. R., Barry, J. G., & Amitay, S. (2014). Listening effort and fatigue: What exactly are we measuring? A British Society of Audiology Cognition in Hearing Special Interest Group ‘white paper.’ International Journal of Audiology, 53(7), 433–445. https://doi.org/10.3109/14992027.2014.890296
Mealings, K., Valderrama, J. T., Mejia, J., Yeend, I., Beach, E. F., & Edwards, B. (2024). Hearing aids reduce self-perceived difficulties in noise for listeners with normal audiograms. Ear and Hearing, 45(1), 151–163. https://doi.org/10.1097/AUD.0000000000001412
Meikle, M. B., Henry, J. A., Griest, S. E., Stewart, B. J., Abrams, H. B., McArdle, R., Myers, P. J., Newman, C. W., Sandridge, S., Turk, D. C., Folmer, R. L., Frederick, E. J., House, J. W., Jacobson, G. P., Kinney, S. E., Martin, W. H., Nagler, S. M., Reich, G. E., Searchfield, G., … Vernon, J. A. (2012). The Tinnitus Functional Index: Development of a new clinical measure for chronic, intrusive tinnitus. Ear and Hearing, 33(2), 153–176. https://doi.org/10.1097/AUD.0b013e31822f67c0
Moore, B. C. J. (1996). Perceptual consequences of cochlear hearing loss and their implications for the design of hearing aids. Ear and Hearing, 17(2), 133–161.
Nachtegaal, J., Festen, J. M., & Kramer, S. E. (2012). Hearing ability in working life and its relationship with sick leave and self-reported work productivity. Ear and Hearing, 33(1), 94–103. https://doi.org/10.1097/AUD.0b013e318228033e
Nachtegaal, J., Kuik, D. J., Anema, J. R., Goverts, S. T., Festen, J. M., & Kramer, S. E. (2009). Hearing status, need for recovery after work, and psychosocial work characteristics: Results from an internet-based national survey on hearing. International Journal of Audiology, 48(10), 684–691. https://doi.org/10.1080/14992020902962421
National Guideline Centre (UK). (2020). Evidence review for psychoacoustic measures: Tinnitus: Assessment and management. National Institute for Health and Care Excellence (NICE).
Newman, C. W., Jacobson, G. P., & Spitzer, J. B. (1996). Development of the Tinnitus Handicap Inventory. Archives of Otolaryngology–Head & Neck Surgery, 122(2), 143–148. https://doi.org/10.1001/archotol.1996.01890140029007
Nguyen, D. L., Valentin, O., Lehmann, A., & Prévost, F. (2024). A multimodal investigation of listening effort in single-sided deafness. American Journal of Audiology, 33(4), 1341–1349. https://doi.org/10.1044/2024_AJA-24-00073
Noguchi, M., Suzuki, N., Oishi, N., & Ogawa, K. (2021). Effectiveness of hearing aid treatment in patients with chronic tinnitus: Subscale evaluations using the Tinnitus Functional Index and factor analysis. The Journal of International Advanced Otology, 17(1), 42–48. https://doi.org/10.5152/iao.2020.9161
Ohlenforst, B., Zekveld, A. A., Jansma, E. P., Wang, Y., Naylor, G., Lorens, A., Lunner, T., & Kramer, S. E. (2017). Effects of hearing impairment and hearing aid amplification on listening effort: A systematic review. Ear and Hearing, 38(3), 267–281. https://doi.org/10.1097/AUD.0000000000000396
Pichora-Fuller, M. K., Kramer, S. E., Eckert, M. A., Edwards, B., Hornsby, B. W. Y., Humes, L. E., Lemke, U., Lunner, T., Matthen, M., Mackersie, C. L., Naylor, G., Phillips, N. A., Richter, M., Rudner, M., Sommers, M. S., Tremblay, K. L., & Wingfield, A. (2016). Hearing impairment and cognitive energy: The Framework for Understanding Effortful Listening (FUEL). Ear and Hearing, 37, 5S–27S. https://doi.org/10.1097/AUD.0000000000000312
Picou, E. M., Moore, T. M., & Ricketts, T. A. (2017). The effects of directional processing on objective and subjective listening effort. Journal of Speech, Language, and Hearing Research, 60(1), 199–211. https://doi.org/10.1044/2016_JSLHR-H-15-0416
Raj-Koziak, D., Gos, E., Swierniak, W., Rajchel, J. J., Karpiesz, L., Niedzialek, I., Wlodarczyk, E., Skarzynski, H., & Skarzynski, P. H. (2018). Visual Analogue Scales as a tool for initial assessment of tinnitus severity: Psychometric evaluation in a clinical population. Audiology & Neuro-Otology, 23(4), 229–237. https://doi.org/10.1159/000494021
Roup, C. M., Post, E., & Lewis, J. (2018). Mild-gain hearing aids as a treatment for adults with self-reported hearing difficulties. Journal of the American Academy of Audiology, 29(6), 477–494. https://doi.org/10.3766/jaaa.16111
Sanders, P. J., Nielsen, R. M., Jensen, J. J., & Searchfield, G. D. (2023). Hearing aids with tinnitus sound support reduce tinnitus severity for new and experienced hearing aid users. Frontiers in Audiology and Otology, 1, 1238164. https://doi.org/10.3389/fauot.2023.1238164
Sarampalis, A., Kalluri, S., Edwards, B., & Hafter, E. (2009). Objective measures of listening effort: Effects of background noise and noise reduction. Journal of Speech, Language, and Hearing Research, 52(5), 1230–1240. https://doi.org/10.1044/1092-4388(2009/08-0111
Shekhawat, G. S., Searchfield, G. D., & Stinear, C. M. (2013). Role of hearing aids in tinnitus intervention: A scoping review. Journal of the American Academy of Audiology, 24(8), 747–762. https://doi.org/10.3766/jaaa.24.8.11
Simonetti, P., Vasconcelos, L. G., Gândara, M. R., Lezirovitz, K., de Medeiros, Í. R. T., & Oiticica, J. (2022). Hearing aid effectiveness on patients with chronic tinnitus and associated hearing loss. Brazilian Journal of Otorhinolaryngology, 88, S164–S170. https://doi.org/10.1016/j.bjorl.2022.03.002
Theodoroff, S. M. (2020). Tinnitus questionnaires for research and clinical use. The Behavioral Neuroscience of Tinnitus, 403–418. https://doi.org/10.1007/7854_2020_175
Theodoroff, S. M., Schuette, A., Griest, S., & Henry, J. A. (2014). Individual patient factors associated with effective tinnitus treatment. Journal of the American Academy of Audiology, 25(7), 631–643. https://doi.org/10.3766/jaaa.25.7.2
Vaisberg, J. M., Gilmore, S., Qian, J., & Russo, F. A. (2024). The benefit of hearing aids as measured by listening accuracy, subjective listening effort, and functional near infrared spectroscopy. Trends in Hearing, 28. https://doi.org/10.1177/23312165241273346
Valderrama, J. T., Mejia, J., Wong, A., Herbert, N. C., & Edwards, B. (2025). Reduced listening effort with adaptive binaural beamforming in realistic noisy environments. Scientific Reports, 15(1), 17998. https://doi.org/10.1038/s41598-025-95045-3
Villatte, B., Bigras, C., Fournier, P., Fitzpatrick, E., & Hébert, S. (2025). Patients with tinnitus: Their perspective on sound generators. Noise and Health, 27(126), 233–245. https://doi.org/10.4103/nah.nah_179_24
Waechter, S., & Jönsson, A. (2022). Hearing aids mitigate tinnitus, but does it matter if the patient receives amplification in accordance with their hearing impairment or not? A meta-analysis. American Journal of Audiology, 31(3), 789–818. https://doi.org/10.1044/2022_AJA-22-00004
Waechter, S., Olovsson, M., & Pettersson, P. (2023). Should tinnitus patients with subclinical hearing impairment be offered hearing aids? A comparison of tinnitus mitigation following 3 months hearing aid use in individuals with and without clinical hearing impairment. Journal of Clinical Medicine, 12(24), 7660. https://doi.org/10.3390/jcm12247660
Waechter, S., Timmer, B. H., Olovsson, M., Pettersson, P., Frawley, L., Ibertsson, T., Thorén, E. S., & Jönsson, A. (2025). Conventional hearing aid amplification, notch therapy, or increased gain at tinnitus pitch: A randomised controlled multicentre study. International Journal of Audiology, 1–24. https://doi.org/10.1080/14992027.2025.2544152
Wingfield, A. (2016). Evolution of models of working memory and cognitive resources. Ear and Hearing, 37, 35S–43S. https://doi.org/10.1097/AUD.0000000000000310
Zekveld, A. A., Kramer, S. E., & Festen, J. M. (2011). Cognitive load during speech perception in noise: The influence of age, hearing loss, and cognition on the pupil response. Ear and Hearing, 32(4), 498–510. https://doi.org/10.1097/AUD.0b013e31820512bb
Acknowledgments
The authors wish to acknowledge funding from the U.S. Department of Veterans Affairs through VA Rehabilitation Research Development & Translation (merit award: I01RX003702; National Center for Rehabilitative Auditory Research center award: I50RX002361), which support efforts to prepare this manuscript. The contents do not represent the views of the U.S. Department of Veterans Affairs or the U.S. government.
Citation
van Ginkel, C., Anderson G. A., & Billings, C. J. (2026). How are tinnitus and listening effort affected by hearing aid use? AudiologyOnline, Article 29535. www.audiologyonline.com

