 From the desk of Gus Mueller
From the desk of Gus Mueller
What? You say you don't believe in prescriptive methods for programming hearing aids? Really? Then let me ask you this: Your Monday morning patient has a relatively flat 60 dB loss of cochlear origin. Would you program his hearing aids with 60 dB gain? Of course not. How about 10 dB gain? Not good either, right? Guess what—the moment you reached these conclusions, you're already using a prescriptive fitting approach.
As Denis Byrne so appropriately stated 30 years ago:
"The only choices are whether we admit to using a theoretical procedure, or even realize that we are doing so, and whether we are prepared to say what procedure we are using . . . The only problem with confessing to using a theoretical procedure is that it inevitably exposes our inadequacies."
 So once you "admit" to using a fitting procedure, the question then becomes what procedure to use? For you seasoned veterans out there, you might remember the days when we had ten or more prescriptive methods to choose from: Lybarger, MSU, CID, Berger, Libby, POGO (and let's not forget POGO II), VIOLA, FIG6, the earlier versions of NAL and DSL, and many more. It's important to point out, however, that with the technology available at the time, and often armed with only a single adjustment potentiometer and a screw-driver (or an electronic screw-driver), we seldom matched the targets in the real ear for any of the methods for the frequencies above 2000 Hz, which tended to minimize the differences among the procedures. That is, if you could only obtain 1/3 gain at 4000 Hz in the real ear, it really didn't matter if the prescriptive method called for 1/3, 1/2 or 2/3!
So once you "admit" to using a fitting procedure, the question then becomes what procedure to use? For you seasoned veterans out there, you might remember the days when we had ten or more prescriptive methods to choose from: Lybarger, MSU, CID, Berger, Libby, POGO (and let's not forget POGO II), VIOLA, FIG6, the earlier versions of NAL and DSL, and many more. It's important to point out, however, that with the technology available at the time, and often armed with only a single adjustment potentiometer and a screw-driver (or an electronic screw-driver), we seldom matched the targets in the real ear for any of the methods for the frequencies above 2000 Hz, which tended to minimize the differences among the procedures. That is, if you could only obtain 1/3 gain at 4000 Hz in the real ear, it really didn't matter if the prescriptive method called for 1/3, 1/2 or 2/3!
Today, with improved microphone and receiver technology, and sophisticated automatic feedback reduction algorithms, we really can fit to prescriptive target for most patients. This makes choosing the "right" method even more important than it was in years past. And there is more good news. Our list is shorter. We now really only have two methods to choose from: the latest versions of the NAL and the DSL. So you might ask, are these two methods pretty much the same, or are there significant differences between them? Good question, and we brought in a guest to 20Q this month who is prepared to answer this.
Earl Johnson, AuD, PhD is an advanced practice audiologist for the U.S.A. Department of Veterans Affairs Medical Center (VAMC) in Mountain Home, Tennessee. He also participates in the Doctorate of Audiology curriculum instruction at East Tennessee State University as an Assistant Professor. Much of Dr. Johnson's research and training has been focused on the efficacy and effectiveness of hearing aid product features and signal processing as well as hearing aid dispensing and practicing trends. While he is only a few years removed from his Ph.D. training at Vanderbilt, his publications already include numerous journal articles and book chapters, and he is a frequent workshop speaker.
Dr. Johnson is a currently funded research investigator through the VA Rehabilitation Research and Development Program on a Career Development Award. I suspect that Earl's interest in prescriptive fitting approaches was somewhat influenced by his visit to Australia a couple years ago, where he spent several months at the Australian National Acoustic Laboratories working with Harvey Dillon. Understanding and comparing these two new prescriptive fitting methods is no easy task, and we're fortunate that Earl has done all the hard work for us.
And of course, when you are thinking about the NAL and the DSL fitting procedures, what would be better than to have comments from the gurus themselves? Check out this month's Bonus 20Q, where Harvey Dillon and Susan Scollie comment on Earl's article, and provide a few extra pearls for you about their procedures.
April 20Q Bonus: Harvey Dillon and Susan Scollie Discuss their Latest Fitting Formulas
Gus Mueller, Ph.D.
Contributing Editor
April 2012
To browse the complete collection of 20Q with Gus Mueller articles, please visit www.audiologyonline.com/20Q
1. Before we get to the specific methods, are you sure it's even possible to "prescribe" hearing aid gain and output? Sure, provided a few qualifiers. Prescriptions have most always been either: 1) group-based, threshold-based approaches to amplify conversational speech, or 2) estimates of loudness recruitment to restore normal loudness perception. The accuracy of the first depends on the accuracy of threshold measurement and the extent to which the hearing aid wearer is a typical, average individual. The second depends on the accuracy of loudness scaling within the individual and for group-based approaches the consistency of loudness scaling across patients.
Sure, provided a few qualifiers. Prescriptions have most always been either: 1) group-based, threshold-based approaches to amplify conversational speech, or 2) estimates of loudness recruitment to restore normal loudness perception. The accuracy of the first depends on the accuracy of threshold measurement and the extent to which the hearing aid wearer is a typical, average individual. The second depends on the accuracy of loudness scaling within the individual and for group-based approaches the consistency of loudness scaling across patients.
My favorite article on the topic was written by Dennis Byrne almost 20 years ago (Byrne, 1996). In it he discusses hearing aid selection based on prescriptive formulas and underlying philosophies. He was very much concerned about the possibility that the hearing aid fitter would lose control of the fitting process and that nonvalidated prescription formulae would proliferate. His concerns are as relevant today as when he wrote them.
2. You didn't answer my question. Is it possible?
Over the years, many clinicians and researchers have noted the intersubject variability that poses a challenge to prescribing gain-frequency responses that are preferred by nearly all subjects. Byrne and Cotton (1988) indicated that as many as 20% of individuals may prefer an alternate preference to NAL-R.
The fact that hearing aid prescriptions were too loud was a major criticism of the previous NAL-NL1 and DSL v4.1 versions. For example, Keidser and Dillon (2006) indicated that 46% of subjects found NAL-NL1 "too loud", as their preferred listening level was more than 3 dB below prescribed levels.
As an evidence review of the time, Mueller (2005) indicated a moderate level of evidence existed for using prescriptive methods to approximate the real-world outcome of the use gain preferred by a group of patients. So yes, I believe it is possible to prescribe amplification. Following which, through typical clinical interactions with the patient, that prescription may be modified to accommodate individual patient differences.
As a result of new knowledge in the past decade, the NAL-NL1 and DSL v4.1 prescriptions have undergone revisions. The latest of these revisions are from two prominent prescriptive groups that you no doubt know well: the NAL-NL2 and the DSL m[i/o], aka DSL v5.0.
3. I'm interested in the new methods, but you still haven't convinced me—doesn't the volume control eliminate the need for "prescribed" gain?
First, many people are fitted with hearing aids that don't have volume controls, but let's forget that for the moment. The volume control changes gain but only within a finite and usually limited range. Also, volume control adjustments generally extend across a wide range of frequencies. Provided the frequency-specific nature of hearing loss, the amount of applied gain needs to be in discrete frequency locations. Additionally, let's consider these two other factors.
- From an audiologic standpoint, the quick history on the need for prescriptions goes as follows. The birth of the prescriptive concept was credited to West in about 1937 but Watson and Knudsen (1940) are often remembered for their mirroring the most comfortable level (MCL) curves using a tonal stimuli approach, and of course, Lybarger (1944) was known for the half-gain rule. The half-gain rules specified that frequency-specific gain should equal half the air conduction threshold. One setback of the time was that analog hearing aids lacked sophistication of more than gross frequency response control. To this end, and because the use of loudness and threshold measurements in the clinic were regarded as impractical by some individuals, there were indications that frequency response could not be prescribed for any individual.
As such, flat amplification or rising 6 dB per octave became common frequency responses recommended for hearing aids, e.g. The Harvard Report, Davis et al. (1946) and MedResCo Report, Radley et al. (1947). In the late 1970s and early '80s, Pascoe, Skinner, and colleagues at Central Institute for the Deaf showed that a frequency response could be selected for an individual that would produce the best speech recognition score based on audiologic measurements (Pascoe, 1975; Skinner, 1980; Skinner, Pascoe, Miller, & Popelka, 1982). From that time until current day, many prescriptions for selecting responses for an individual have been proposed, but only a few would be considered scientifically validated.
- From a quantitative standpoint, let's consider the number of possibilities for programming the frequency response of a typical power BTE, for instance a 16 channel device with up to 70 dB gain in 1 dB increments. Using permutation mathematics allowing repetition, such a calculation indicates there are a lot of gain-frequency response possibilities (71^16 = 4.16E+29).* Yes, the number is so large that scientific notion is used instead of individual integers.
To say that number out loud, you would read: Four hundred sixteen octillion, nine hundred ninety-seven septillion, six hundred twenty-three sextillion, one hundred sixteen quintillion, and three hundred seventy quadrillion.
Assuredly, there must be lot fewer reasonable frequency responses that are appropriate for treating any one individual's hearing loss. Wouldn't you like to have your choices narrowed?
* Footnote 1 - There are 71 incremental divisions in the 70 dB range to include the possibility of 0 dB of prescribed insertion gain which is common when hearing thresholds are near or within the normal sensitivity range.
4. Of course. But, I could narrow it just using my clinical experience. Why doesn't that work?
Let's consider a formula that calculates the odds of success by calculating the product of a restrictive series of fractional values from the number of estimated possibilities known to the field of physics as Drake's Equation.
You might have seen the equation recently popularized in the TBS comedy, Big Bang Theory or in one of Bill Bryson's books entitled, The Short History of Nearly Everything.
As applied here to hearing aid frequency responses, we can rule out a large number of possible frequency responses because we are certain that "best" frequency-specific amplification will fall in some limited range of each channel's available 70 dB of gain. I'm working with your comment of "clinical experience." As a result, let's assume that an optimal frequency response falls within a 20 dB range in each of the 16 channels - the range of a typical hearing aid volume control (±10 dB ) - provided that the amount of desired gain in any one channel is dependent upon an individual patient's hearing loss in the channel's covered frequency range.
Still there is need for a somewhat "smooth" response across the side-by-side channels of adjacent frequencies. That is, not only are there technological challenges, but really there is not a typical need with respect to hearing loss configuration, for 0 dB of gain in one frequency channel, followed by 20 dB of gain in the adjacent channel, and 0 dB of gain in the next channel and so on. Remember that the inclusion of a 0 dB gain possibility allows for 21 dB increments. Thus, so somewhat smooth frequency responses are obtained, let's eliminate an additional 99.9999% of the available 16 channel, 20 dB range frequency response choices.
Then applying further fractional values that only a few frequency responses can simultaneously provide the best speech intelligibility (1 out of 10,000), an adequate, but acceptable loudness (1 out of 10,000), and actually be preferred for sound quality by the patient (1 out of 10,000) eliminates a lot more possible frequency responses*.
After all of which, 1430 possible frequency responses still remain from which to choose for any particular patient!!!
4.16998E+29*(21/71)^16*0.000001*(0.0001)^3 = 1430
This number does not even consider the prescription of frequency response as a function of input level - common in wide dynamic range compression hearing aids. We have only considered a single input level of say, average level speech at 65 dB SPL.
I hope this demonstrates why we need prescriptions; they focus our efforts on a frequency response or range of responses that are in all likelihood "optimal" based on underlying rationale(s) of the prescription and are, as a result, inherently selective.
* Footnote 2 - If more conservative (less extreme) assumptions are made, the number of possible frequency responses to consider only increases.
5. Can you elaborate on what you mean by "selective?"
It simply means to not apply gain in either a random manner or common manner for any and all hearing losses encountered, but rather to be selective in the choice with a basis on audiologic measures and subsequent rationale(s).
6. What rationales do hearing aid prescriptions use?
There are several main rationales hearing aid prescriptions may follow. Aside from categorizing prescriptions based on whether they are based on threshold or suprathreshold audiologic measures, for linear or non-linear hearing aids, or from proprietary or non-proprietary sources, the most common rationales to consider are that of loudness normalization and loudness equalization.
7. I've heard of those last two rationales, but they sort of sound the same to me. What exactly is the difference?
In brief, loudness normalization intends to restore, usually for certain frequency bands, the loudness perception of the listener with hearing impairment to the same loudness perceived by a listener with normal hearing. Loudness normalization can also mean that soft, medium, and loud speech as heard by a normal hearer are appropriately amplified to the categorical rating descriptor of "soft" "average" and "loud" by an individual with hearing impairment. When obtaining loudness growth curves across frequencies, Cox and colleagues (1997) validated use of the Contour Test with loudness categories numbered 1 to 7, "Very soft", "Soft", "Comfortable, but Slightly Soft", "Comfortable", "Comfortable, but Slightly Loud", "Loud, but OK", and "Uncomfortably Loud."
In contrast, loudness equalization aims to equalize the perception of loudness over a range of frequencies instead of having lower frequencies dominate loudness as is the case for listeners with normal hearing. For example, the frequency range of 500-4000 Hz can be amplified such that the loudness perception of 500 Hz and 4000 Hz as well as the various narrow bands in between are equivalent in the unit of sones. This process was explicit in the earlier years of linear NAL prescriptions.
8. Do the NAL and the DSL prescriptions use the same rationale?
Kind of, sort of. NAL prescriptions are definitely loudness equalizers. Equalizing loudness across frequency was in fact the intent of linear NAL procedures (i.e., NAL, NAL-R and NAL-RP). NAL-NL1 was not designed to equalize loudness per se, however, the authors noted that the speech intelligibility index optimization with a constrained overall loudness budget secondarily equalized loudness in the mid-frequencies between 500 and 2000 Hz. (Byrne, Dillon, Ching, Katsch, & Keidser, 2001). This finding was positively regarded as further substantiation of the earlier loudness equalization rationale. NAL-NL2 also equalizes loudness across the mid-frequencies (Johnson & Dillon, 2011).
The underlying rationale for the DSL procedure has been to normalize loudness at each frequency (Cornelisse, Seewald & Jamieson, 1995; Scollie et al., 2005). Although, Seewald et al. (1996) described the DSL as a procedure that can be modified to provide equalized loudness. In the 1990s there were prescriptions that used loudness normalization as a primary rationale: the Visual Input-Output Locator Algorithm (VIOLA) of the Independent Hearing Aid Fitting Forum (IHAFF) protocol (Cox, 1995; Valente & Van Vliet, 1997) and FIG6 (Killion, 1994; 1995). These two loudness normalization prescriptions have fallen out of vogue as evidenced by the lack of commonplace use.
9. How do the latest NAL and DSL methods compare and contrast?
Well, that depends on what you want to compare and contrast as well as for what particular patient population. For example, we could compare insertion gain or aided response (output) targets, speech intelligibility, loudness, frequency bandwidth, or a smorgasbord of patient outcomes.
We could also specify new or experienced hearing aid users, adults or children, females or males, sensorineural or conductive hearing loss components, unilateral or bilateral, listening in noise or in quiet, etc.
10. Gosh, I thought it would be more straightforward?
Actually, it is rather straightforward. Let's start by specifying what population you are most interested in.
11. I mostly fit adults, so can we start there?
Johnson and Dillon (2011) showed that for a selection of sensorineural hearing losses for adults, the average prescribed loudness of both NAL-NL2 and DSL m[i/o] agreed well with past laboratory and field trials of preferred hearing aid loudness (Smeds, 2006a,b). This loudness was about 8 sones for each prescription and was a little less than half the loudness that was prescribed by the previous NAL-NL1 method. That halving is definitely a noticeable difference to most of individuals with hearing impairment!
Poloneko et al. (2010) has additionally demonstrated that DSL m[i/o] targets approximated, on average, the preferred listening levels of participants within 2.6 dB.
In quiet listening environments, speech recognition for sentence material often approximates 100% with prescriptive restoration of the selected hearing losses. In noisy environments, speech recognition was, of course, poorer. It was worse not because of a lack of prescribed audibility but rather masking properties of the noise itself. Averaged across the five sensorineural hearing losses in Johnson and Dillon (2011), NAL-NL2 and DSL m[i/o] were the same. Both methods provided an estimated 96% predicted intelligibility at +10 dB signal-to-noise ratio (SNR), 77% at 0 dB SNR, and 7% at a -10 dB SNR for sentence level material of the Connected Speech Test (Cox, Alexander & Gilmore, 1987) with a transfer function from Humes (2002).
12. So I assume the similarities between NAL-NL2 and DSL m[i/o] means they both prescribe similar frequency responses?
That is a fair assumption, but there are still some noteworthy differences. Sometimes the differences are small (within ±5 dB) but other times, depending on the configuration and severity of hearing loss, they can be much larger.
One generality is that for more severe-to-profound hearing loss thresholds DSL m[i/o] will prescribe more insertion gain than NAL-NL2 at average input levels. Note in Figures 1 and 2 that for audiogram A-2, DSL [m[i/o] prescribes much more gain than NAL-NL2 in the low frequencies and for audiograms A-4 and A-5, DSL m[i/o]provides more gain in the high frequencies. One explanation for the use of less gain by NAL-NL2 for poorer hearing thresholds is its use of a revised desensitization factor. The factor predicts less utility for extracting speech information as hearing thresholds worsen.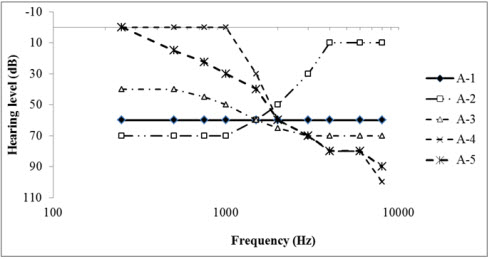
Figure 1. Audiograms 1-5 (A-1 through A-5). Used with permission from Johnson and Dillon (2011). J Am Acad Audiol 22:441-459.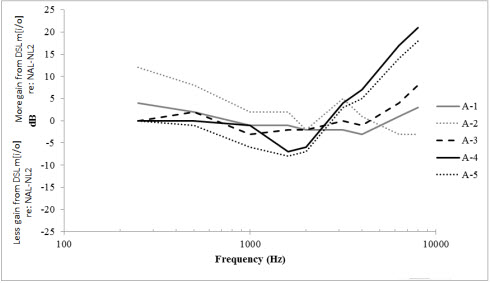
Figure 2. Frequency-specific differences in insertion gains prescribed by DSL m[i/o] and NAL-NL2 for each of the five sensorineural hearing losses. The data is reported as DSL m[i/o] minus NAL-NL2. Negative numbers indicate less gain from DSL m[i/o] and positive numbers indicate more gain from DSL m[i/o] for a 65 dB SPL input re: NAL-NL2. When targets were unavailable from the standalone prescriptions, gain through 8 kHz was extrapolated based on the recommended gain of the highest available frequency using a 6 dB/octave slope. Used with permission from Johnson and Dillon (2011). J Am Acad Audiol 22:441-459. Click Here to View Larger View of Figure 2 (PDF)
13. What are the differences in the prescriptions for children?
We could spend another 20 questions devoted to prescriptive methods for children, so I'd like to keep our discussion focused on adults. But, since you asked, let me briefly say that as compared to adults, the DSL m[i/o] increases gain by 7 dB for medium level inputs, provides less gain for high level inputs, and provides more gain for low level inputs for children (Scollie et al., 2005). In a similar vein, the NAL-NL2 prescribes 5 dB more gain for medium input levels, less for high input levels, and more for low input levels for children than for adults (Keidser, Dillon, Flax, Ching, & Brewer, 2011). Both methods also allow for a higher compression ratio for children relative to adults. Figure 3, used with permission from Keidser et al. (2011), is a nice representation of the difference in the NAL-NL2 prescription for both children and adults with reference to the NAL-NL1 prescription.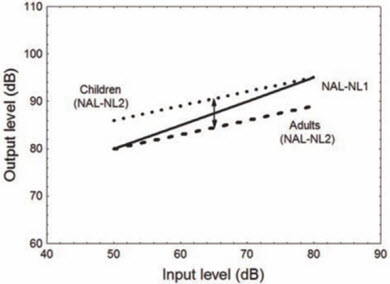
Figure 3. A schematic overview of the changes to the overall output level prescribed by NAL-NL2 relative to NAL-NL1 across different input levels for children (dotted line) and adults (broken line). Used with permission from Keidser et al (2011).
14. So what about specific patient factors—how do they compare between the two methods?
Let's consider the following specific patient factors: hearing aid experience, gender, bilateral versus unilateral, and the use of loudness discomfort measures.
Experience: It is now fairly well documented that new hearing aid users desire less amplification that experienced users - a convention that has been highly controversial in the recent past (Convery, Keidser & Dillon, 2005). At this time, DSL m[i/o] does not incorporate a correction for gain based on new or experienced hearing aid user status (Scollie et al., 2005; Scollie, personal communication, 2012). NAL-NL2 incorporates adjustments that not only differ as a function of hearing loss but include an increase for experienced users and a decrease for new users (Figure 4).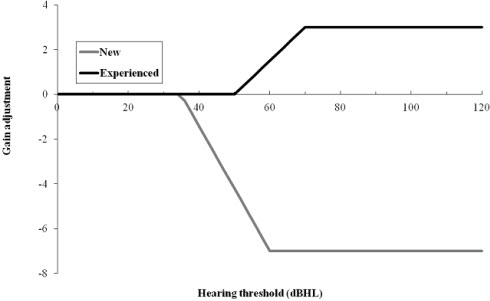
Figure 4. Adjustments to default NAL-NL2 prescribed gain derivations based on the hearing aid experience and pure tone average hearing threshold level of the patient.
Gender: DSL m[i/o] does not include an adjustment for gender whereas NAL-NL2 includes a 1 dB increase in gain for male wearers and a 1 dB decrease in gain for female wearers. The NAL-NL2 adjustment was based on an analysis, irrespective of degree of hearing loss and experience with amplification, that females preferred 2 dB, on average, less gain than males (Keidser & Dillon, 2006; Keidser et al., 2011).
Bilateral fittings: DSL m[i/o] prescribed targets for speech are reduced by 3 dB across input levels for bilateral fittings re: unilateral fittings (Scollie et al., 2005). NAL-NL2 has a bilateral gain correction that increases with input level. The correction for binaural summation is 2 dB at low input levels and up to 6 dB at high input levels for symmetric losses, and less for asymmetric losses.
Loudness discomfort measures: NAL-NL2 does not alter its prescription of gain and output at any input level based on loudness discomfort levels (LDLs) or uncomfortable listening levels (ULLs). In fact, an entry for patient-specific loudness discomfort measures is not an option. Whereas DSL m[i/o] will accept patient-specific loudness discomfort measures; subsequently, it will alter its prescription of gain and output for not only high input levels that approximate the loudness discomfort measure but also the gain and output for soft input levels as well.
A few other differences are that NAL-NL2 includes a slight adjustment for less gain with an increasing number of channels (a channel summation effect). NAL-NL2 also includes alternate recommendations for tonal and non-tonal languages as the frequency importance function for the types of languages differ and as such affected the speech intelligibility optimization procedures upon which NAL-NL2 was based.
15. Those corrections sound pretty small. Do they really matter?
They can. Here is an example using NAL-NL2. We'll take two different patients that you might have on any given Monday morning: a woman obtaining her first set of hearing aids, and an experienced male user, obtaining a new set of hearing aids. To make it easy, let's say that they have the same hearing loss; 20-30 dB HL in the low frequencies sloping down to 70 dB HL at 2 kHz and above. While their hearing loss is the same, the prescribed insertion gain at 2 kHz for the female for a 65 dB SPL speech input would be 16 dB, whereas for the male it would be 21 dB. At 4 kHz, the respective insertion gains are 23 and 29 dB. I think that's a big enough difference to matter, and perhaps could even impact the success of the fitting.
16. So let's get practical. Most hearing aids now have a "trainable" option. Does that mean I no longer need a NAL-NL2 or DSL m[i/o] prescription?
The training capability still relies on the initial prescribing of hearing aid amplification characteristics for individual listeners. This is based upon research that indicates when listeners are allowed to train the frequency- and input-dependent gain of the hearing aids, the end result is affected by the starting response (baseline) (Dreschler, Keidser, Convery, & Dillon, 2008; Keidser, Dillon & Convery, 2008; Mueller, Hornsby & Weber, 2008).
For example, Mueller et al. (2008) used an analysis of effect size, partial eta squared η2, to determine that 92% of the variability in preferred gain deviations was attributable to the starting point. Keidser et al. (2008) further indicated that some trained settings are not overwhelmingly "preferred" settings compared to untrained settings, and Dreschler et al. (2008) indicated the end trained response is affected by the training interface device itself. The point is—if you want a good trained setting, it's best to start with gain and output that is at least close to optimum for the average person.
17. So you're saying it's okay for my patients to train their hearing aids?
That is a loaded question. But the practicing consensus would appear to be a resounding, yes - at least for those patients who can adequately manipulate their hearing aid or remote control accurately and reliably. This goes back to my earlier comments that the prescription represent what research has shown to be best for "average."
18. Where do I find DSL m[i/o] and NAL-NL2 prescriptive recommendations?
You will find them in almost every hearing aid manufacturer's programming software. Although, you will have to check out the "preferences" or "options" section to ensure that the prescriptive method you desire is selected. Most manufacturers choose as the default their own proprietary prescriptions which by definition include many unknowns and should not be assumed equivalent or similar enough to DSL m[i/o] or NAL-NL2.
Also, you may contact either the University of Western Ontario Audiology research group or the National Acoustic Laboratories Audiology research group if your specific purposes would require a stand-alone software app.
19. But I thought that just choosing the prescription in the programming software wasn't enough. The prescriptive targets need to be verified by either coupler or real-ear measures, correct?
You are correct. That step is the vital part to evidence-based practice use of prescriptive methods for hearing aid fittings. Currently, you will have some difficulty finding the newest prescriptive methods in some hearing aid test systems. To circumvent this reality you may have to modify the system's targets (i.e., insertion gain, aided gain, or aided response), if possible, with those made available by the manufacturer in the programming software or from a stand-alone software app. See the system's user manual for how and if this can be accomplished with your system.
As an alternative, we are currently evaluating the potential for fitting to new prescriptive targets with novel, live-real ear applications built into the manufacturer program software until new prescriptive targets are made available on hearing aid test systems. Of course, we hope for the availability of the newest prescriptions on separate hearing aid test systems soon. Be sure to check with your local distributor of hearing aid verification equipment on the availability of NAL-NL2 and DSL m[i/o] if upgrading to new equipment for use in the clinic or research.
20. Okay, you've pretty much convinced me to use prescriptive methods, but I have to ask—do I pick the NAL or the DSL?
I am so glad you asked that question. As dispensers of hearing aids, we sometimes think that such choices are ours to make because, after all, it is unlikely that our patients will have familiarity with the prescriptive alternatives for hearing aids. I sometimes have to explain to patients and research subjects that prescriptions are about how the hearing aid sounds not how the device looks.
True patients can get darn good results with both NAL or DSL prescriptions and using either is much better no prescriptive rationale at all!
But, I'd like for us to consider the feasibility of allowing patients to choose between prescriptive alternatives at the time of their initial fitting and/or throughout the period of acclimatization to amplification. It seems probable that when considerable variation in prescribed frequency response exists between prescriptions (e.g., 5+ dB differences shown in Figure 2) , a patient might have a preference for one response over another, consistent with Keidser and colleagues (1995), perhaps even when overall loudness and speech intelligibility have been shown comparable (Johnson & Dillon, 2011). That is, given the capability to rapidly verify prescriptive recommendations with real-ear probe microphone equipment and quickly alternate those recommendations in a programming software, the patient may very well be able to pick for themselves. The dispenser, of course, should facilitate this process with the patient, however its operating parameters and steps may be defined.
This article was supported by a Career Development Award-1 by the U.S.A. Department of Veterans Affairs Rehabilitation Research and Development Office.
Disclaimer: The opinions expressed in this article are those of the author and do not necessarily represent the official position of the U.S. Department of Veterans Affairs or the United States government.
References
April 20Q Bonus: Harvey Dillon and Susan Scollie Discuss their Latest Fitting Formulas In this month's 20Q, our Question Man travelled to eastern Tennessee to talk to our guest author Earl Johnson . Their conversation resulted in a very informative comparison of the two hearing aid prescriptive fitting methods that we use today: the NAL-NL2 from the National Acoustic Laboratories and the Desired Sensation Level (DSL) from the University of Western Ontario. There is quite a history surrounding both of these methods.
In this month's 20Q, our Question Man travelled to eastern Tennessee to talk to our guest author Earl Johnson . Their conversation resulted in a very informative comparison of the two hearing aid prescriptive fitting methods that we use today: the NAL-NL2 from the National Acoustic Laboratories and the Desired Sensation Level (DSL) from the University of Western Ontario. There is quite a history surrounding both of these methods.
The modern era of hearing aid prescriptive fitting was launched by an article by Denis Byrne and Will Tonnison in 1976. While not officially called the "NAL method," it soon became known as that, as this was the origin of the research (Denis was the "Audiologist-In-Charge" of research at the NAL). Not too many years later, we started seeing this fellow "Harvey Dillon's" name appear on publications with Denis, and in 1986 Byrne and Dillon published the "revised" NAL prescriptive method (NAL-R). As it became necessary to have a prescriptive method for non-linear hearing aids, the research of Denis and Harvey led to NAL-NL1, and over the past 10 years, Dr. Dillon has developed yet another new and improved NAL version, the NL2.
The same year that the Byrne and Tonnison paper was published, Richard Seewald enrolled in the Ph.D. program at the University of Conneticut, where he worked with Mark Ross and began the development of the original DSL method. The results of their work were published in 1985. The math for calculating his DSL prescriptive output was a little challenging for the average clinician (the process was kindly titled "DSL-By-Hand"), and Richard immediately went to work using his Sinclair ZX81 computer to make the process more automatic. As a result, the DSL was distributed as a software system in 1991, making DSL v3.0 the first computerized fitting method for children. A few years later, when WDRC fittings were becoming standard, we saw the DSL[i/o] (DSLv4.1a) revision. It was also about this time that we started to see Susan Scollie's name associated with publications from "DSL-Land." Through the work of Dr. Scollie and colleagues, DSLv5.0 was introduced in 2005.
It's a special day when both Harvey Dillon and Susan Scollie join us here at 20Q. I know that you'll enjoy reading their comments and unique insights about their prescriptive fitting methods
Gus Mueller, Ph.D.
Contributing Editor
April 2012 From Harvey Dillon
From Harvey Dillon
I enjoyed reading Earl's 20Q article, and I don't have too much to add, especially on the calculation of how many gazillions of ways a modern hearing aid can be adjusted.
As Earl says (reply to Question 8), procedures based on loudness normalization, especially those based on scaling the loudness of individual patients, have not passed the test of time. A complication he does not mention is that normalizing loudness one frequency at a time does not ensure that the loudness of broadband sounds like speech is also normalized. Regarding the tendency of the NAL-NL2 prescription to equalize loudness across frequency as a means of maximizing intelligibility, exceptions to this do occur. If hearing loss is much worse in one frequency region than in others, then NAL-NL2 will not attempt to give that frequency region the same loudness as other regions, as the potential contribution to intelligibility from that region will be less, so equal loudness represents wasted loudness.
The impact of the number of channels on the prescription often concerns people (Question 14). There is no reason why speech at the ear canal should be any different if on its way through the hearing aid it has been broken up into 1, 10, or 100 channels, (as long as the different channels have all been put back together again). However, if the gain of a hearing aid is measured with pure tones, all the power of the signal is concentrated in one narrow frequency channel, so multi-channel hearing aids act as though the pure tone is part of a much more intense broadband sound, and reduce the gain accordingly. Consequently, the gain for pure-tone test signals, but not for broadband test signals, should decrease as the number of channels increase. This characteristic occurs in the NAL-NL1 and NL2 prescription formulae.
Finally, while I recognize that Earl's article was focused on the adult population, I would like to comment that we are following 470 children from the time they get their first hearing aid. They are now from 4 to 9 years of age. Half of these children were randomly assigned to receive the DSL prescription and half the NAL prescription. Although their language scores are significantly affected by a range of predictive factors, the hearing aid prescription used is not amongst these. Given that there are still some differences between the NAL and DSL prescriptions, this result means that quite a number of the adjustment possibilities of the hearing aid that Earl calculated actually are equally effective for the hearing aid wearer, even if they don't sound exactly the same as each other. What seems to be a reasonable conclusion is that using an evidence-based prescription formula is important; whether it is NAL-NL2 or DSLv5.0 seems to be much less important. From Susan Scollie
From Susan Scollie
My hat is off to Earl Johnson for this great overview of prescriptive methods. I really loved Question 4, because it brought me back to the days of developing DSL5. Even though we had a lot of people on the team, it still felt like a very big job - I guess we didn't know we had 1430 choices for each target!
Our group certainly agrees with Earl that fitting and verification to any well-developed, well-validated prescriptive method is more likely to result in positive patient outcomes than not doing so. This consideration is of great importance for those hearing aid users who cannot advocate for their own preferences, including infants and young children.
It's been interesting to see the prescriptions move closer and closer to one another over the years. Yet, as shown here, the differences for some hearing aid users can be considerable: a high-frequency difference of 5 to 20 dB in prescribed high frequency gain can really change the audible bandwidth available from the hearing aid, especially for soft speech. One recent study by Todd Rickets and colleagues tells us that 2/3 of adults prefer a wide aided bandwidth, but 1/3 don't.
So what should we do? Perhaps we should consider the individual. Individual variation in speech recognition performance with audibility is significant: some listeners with severe sloping losses do very well with audible speech while others don't, even in the studies that underlie the original NAL-NL1 desensitization corrections. Our conclusions about which prescription is best may change if we look at the "average patient", versus if we realize that individual patients differ. Some adults do better with a broad audible bandwidth.
Children tend to benefit from (and prefer) more audibility and a broader bandwidth. Hearing aid prescriptions vary in the bandwidth they deliver. SII-based analyses of whether bandwidth matters may miss the true benefits that a broad bandwidth has to offer: a blunt tool perhaps? (Samantha Gustafson and Andrea Pittman published a wonderful study of this problem in IJA last year).
For these reasons, the DSL5 target starts with the assumption that audibility may be helpful, and we scale the listening level a little lower for adults to better approximate their preferences. Maybe a back-to-basics approach includes revisiting how we use one or more prescriptions across patients to better meet each of their needs.
back to article
References
Byrne, D. (1996). Hearing aid selection for the 1990s: where to? Journal of the American Academy of Audiology, 7, 377-395.
Byrne, D., & Cotton, S. (1988). Evaluation of the National Acoustic Laboratories' new hearing aid selection procedure. Journal of Speech and Hearing Research 31(2), 178-186.
Byrne, D., Dillon, H., Ching, T., Katsch, R., Keidser, G. (2001). NAL-NL1 procedure for fitting nonlinear hearing aids: Characteristics and comparisons with other procedures. Journal of the American Academy of Audiology, 12, 37-51.
Convery, E., Keidser, G., & Dillon, H. (2005). A review and analysis: Does amplification experience have an effect on preferred gain over time? The Australian and New Zealand Journal of Audiology, 27(1), 18 - 32.
Cornelisse, L., Seewald, R.C., & Jamieson, D.G. (1995). The input/output formula: a theoretical approach to the fitting of personal amplification. Journal of the Acoustical Society of America, 97, 1854-1864.
Cox, R.M. (1995). Using loudness data for hearing aid selection: the IHAFF approach . Hearing Journal, 48, 10-44.
Cox, R., Alexander, G., & Gilmore, C. (1987). Development of the connected speech test (CST). Ear and Hearing, 8,119s.
Cox, R.M., Alexander, G.C., Taylor, I.M., & Gray, G.A. (1997). The contour test of loudness perception. Ear and Hearing, 18, 388-400.
Davis, H., Hudgins, C. V., Marquis, R. J., Nichols, R. H., Peterson, G. E., Ross, D. A., et al. (1946). The selection of hearing aids. Laryngoscope, 56, 85-115, 135-163.
Dreschler, W., Keidser, G., Convery, E., & Dillon, H. (2008). Client-based adjustments of hearing aid gain: The effect of different control configurations. Ear and Hearing, 29, 214-227.
Humes, L. (2002). Factors underlying the speech-recognition performance of elderly hearing-aid wearers. Journal of the Acoustical Society of America, 112, 1112-1132.
Lybarger S. (1944). U.S. Patent application SN 543, 278. July 3.
Johnson, E., & Dillon, H. (2011). A comparison of gain for adults from generic hearing aid prescriptive methods: Impacts on predicted loudness, frequency bandwidth, and speech intelligibility. Journal of the American Academy of Audiology, 22, 441-459.
Keidser, G., & Dillon, H. (2006). What's new in prescriptive fittings Down Under. In C. Palmer & R. Seewald (Eds.), Hearing care for adults (pp. 133-142). Stafa, Switzerland: Phonak AG.
Keidser, G., Dillon, H. & Byrne, D. (1995). Candidates for multiple frequency response characteristics. Ear and Hearing, 16,562-574.
Keidser, G., Dillon, H., & Convery, E. (2008). The effect of the base line response on self-adjustments of hearing aid gain. Journal of the Acoustical Society of America 124,1668-1681.
Keidser, G., Dillon, H., Flax, M., Ching, T., & Brewer, S. (2011). The NAL-NL2 prescription procedure. Audiology Research, 1, 88-90.
Killion, M. (1994). Fig6.exe software: Hearing aid fitting targets for 40, 65 & 95 dB SPL inputs. (Version 1.01D) Copyright, Mead Killion, Etymotic Research.
Killion, M. (1995). Loudness-data basis for "FIG6" hearing aid fitting targets. Journal of the Acoustical Society of America, 98, 2927-2927.
Lybarger S. (1944). U.S. Patent application SN 543, 278. July 3.
Mueller, H.G. (2005). Fitting hearing aids to adults using prescriptive methods: an evidence-based review of effectiveness. Journal of the American Academy of Audiology, 16, 448 - 460.
Mueller, H.G., Hornsby, B.W.Y., & Weber, J.E. (2008). Using trainable hearing aids to examine real-world preferred gain. Journal of the American Academy of Audiology, 19,758-773.
Pascoe, D. (1975). Frequency responses of hearing aid their effects of the speech perception of hearing impaired subjects. Annals of Otology, Rhinology and Larnygology, 84 (suppl 23), 1-40.
Polonenko, M.J., Scollie, S., Moodie, S., Seewald, R., Laurnagaray, D., Shantz, J., et al. (2010). Fit to targets, preferred listening levels, and self-reported outcomes for the DSL v5.0a hearing aid prescription for adults. International Journal of Audiology, 48, 550-560.
Radley, W. G., Bragg, W. L., Dadson, R. S., Hallpike, C. S., McMillan, D., Pocock, L. C., et al. (1947). Hearing aids and audiometers: Report of the committee on electroacoustics. London: His Majesty's Stationery Office.
Scollie, S., Seewald, R., Cornelisse, L., Moodie, S., Bagatto, M., Laurnagaray, D., et al. (2005). The desired sensation level multistage input/output algorithm. Trends in Amplification, 9,159-197.
Seewald, R.C., Cornelisse, L.E., Ramji, K.V., Sincliar, S.T., Moodie, K.S., Jamieson, D.G. (1996). DSL v4.0 for Windows Manual. London, ON: University of Western Ontario.
Skinner, M. (1980). Speech intelligibility in noise-induced hearing loss: Effects of high frequency compensation. Journal of the Acoustical Society of American, 67, 306-317.
Skinner, M., Pascoe, D., Miller, J.,& Popelka, G. (1982). Measurements to determine the optimal placement of speech energy within the listener's auditory area: a basis for selecting amplification characteristics. In G. Studebaker & F. Bess (Eds.), The Vanderbilt-hearing aid report (pp. 161 - 169). Upper Darby, PA: Monographs in Contemporary Audiology.
Smeds, K., Keidser, G., Zakis, J., Dillon, H., Leijon, A., Grant, F., et al. (2006a). Preferred overall loudness. I. Sound field presentation in the laboratory. International Journal of Audiology, 45, 2-11.
Smeds, K., Keidser, G., Zakis, J., Dillon, H., Leijon, A., Grant, F., et al. (2006b). Preferred overall loudness. II. Listening through hearing aids in field and laboratory tests. International Journal of Audiology, 45, 12 - 25.
Valente, M., & Van Vliet, D. (1997). The independent hearing aid fitting forum (IHAFF) protocol. Trends in Amplification, 2, 6-35.
Watson, L.A. & Knudsen, V.O. (1940). Selective amplification in hearing aids. Journal of the Acoustical Society of America, 11, 406 - 419.


