Learning Outcomes
As a result of this course, participants will be able to:
- Describe three factors that support adding new solutions such as HyperSound to a hearing care practice’s portfolio.
- Explain shared decision making and how it applies to hearing healthcare.
- Provide an overview of HyperSound technology, and explain how it can be integrated into an existing clinical protocol.
Introduction and Overview
Today’s course will review the new HyperSound Clear 500P technology and how it can grow your practice. My goal is to explain why HyperSound should be included in your current product portfolio and how it can be positioned as a viable recommendation in your clinic. In order to satisfy the needs of new and existing patients, HyperSound should be a routine offering, along with hearing aids, assistive devices and aural rehabilitation.
In order to successfully integrate HyperSound into your clinical protocol, there are some considerations that must be taken into account, particularly your existing patient selection process. In addition, as this webinar will highlight, a critical part of the successful implementation of HyperSound is conducting a demonstration for your patients. This state-of-the-art technology is truly the first of its kind. Because it is so new, it is important to demonstrate it to as many patients as possible in order for them to fully experience its potential benefits.
Opportunities
There are three factors at play in the hearing care industry that support including HyperSound as part of your routine treatment offerings.
The first factor is what I refer to as the Silver Tsunami. In the United States, approximately 10,000 people per day turn 65. Over the next 10 to 15 years, the number of people with hearing loss over the age of 65 will approximately double. This wave of older adults provides us with ample opportunities to help meet their hearing aid needs, in addition to offering other products to assist them.
Baby Boomers are a substantial part of this Silver Tsunami. Baby Boomers approach any market a bit differently than previous generations. As I am sure you have heard before, Baby Boomers are more likely to want to be actively involved in their healthcare. They are usually more proactive and knowledgeable about the healthcare options.
A second factor is that the American healthcare system is changing dramatically. The way that medicine is being practiced around the country is also evolving. The manner in which physicians and other healthcare providers work with their patients is moving toward a shared decision making approach. Physicians around the country are being reimbursed differently now than they were a few years ago, and, according to experts, this change is going to occur at a faster pace over the next three to five years. Physicians are now reimbursed to keep patients healthy; this is known as population-based healthcare. In order for a patient to successfully communicate with their physician, their nurse practitioner, or whomever they might see as a medical gate keeper – it's important for them to be able to hear and communicate effectively. In order to achieve that, they must have normal or near-normal hearing, which may involve some type of amplification or instrumentation. The phrase I use to characterize these changes in healthcare is patient engagement. Patient engagement, which is a cornerstone of population-based healthcare, is the key to understanding how changes in the healthcare system might affect us as hearing care professionals.
Finally, important legislation and regulatory changes may occur over the next six to twelve months. Recently, the National Academies of Sciences, Engineering, and Medicine (the National Academies) released the consensus study report, Hearing Health Care for Adults: Priorities for Improving Access and Affordability. Among the recommendations in this report were to create a new category of over-the-counter hearing devices. This can be viewed as an opportunity, because it might bring a new segment of the market into our practices. That new segment, which might be very interested in HyperSound, is likely to have a milder hearing loss and not view their condition as a problem that requires the use of hearing aids.
The Unmet Need of the Hearing Impaired
Let’s take a closer look at various segments of our market in the context of the unmet need of the hearing impaired population (Figure 1). This pyramid represents the segment of the hearing impaired market who may not be using amplification. The top of the pyramid shows that 5% of Americans with hearing loss have a profound loss. Of that small group with profound hearing loss, 70% wear hearing aids or have a cochlear implant; the other 30% choose to be part of the Deaf culture and may rely exclusively on sign language.
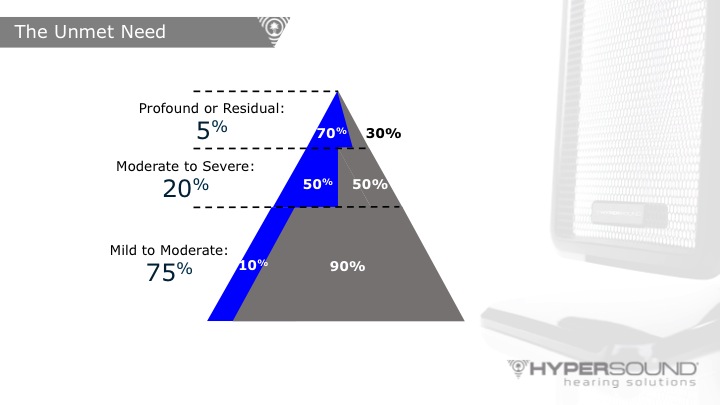
Figure 1. The unmet need of the hearing impaired.
Looking at the middle of the pyramid, we know that about 20% of Americans with hearing loss have a moderate to severe loss. Of that group, 50% use hearing aids and the other half do not. There is some opportunity to grow this market from a hearing aid standpoint to reach that 50% that do not use amplification.
Finally, the vast majority of patients with hearing loss reside at the bottom three-quarters of this pyramid. As you can see, 75% of Americans with hearing loss have a mild to high frequency moderate type of loss. Only 10% of them possess hearing aids. This uncovers some of the real opportunities within the industry, especially with respect to the bottom 75%. If three-quarters of Americans with hearing loss have a mild to moderate loss, and only 10% of them possess hearing aids, there might be some alternative products that would better meet the needs of this segment of the marketplace. HyperSound could be one of those alternative devices that can address the needs of that 90%, or even the 50% in the moderate to severe segment who do not use hearing devices.
Interestingly, recent research has shown that a fairly high number of Americans with normal audiograms have self-reported communication difficulties. When I practiced a few years ago, these were always perplexing cases. These patients expressed a lot of issues and challenges with hearing loss or communication. In taking the case history and completing the needs assessment, it may seem that such a person might have a substantial hearing loss. However, after conducting the audiogram and other tests, the patient’s results are within the normal range.
A 2015 study in Ear and Hearing showed that 12% of adults between the ages of 21 and 84 had a normal audiogram and some self-reported communication difficulties (Tremblay et al., 2015). Many of those self-reported communication difficulties are quite possibly with at-home television viewing. We are finding that watching TV at home is a very important situation where people want improved hearing. Again, HyperSound would be an ideal choice for patients that have self-reported difficulties with the television, and have hearing loss or perhaps even normal hearing.
Stages of Change
Let’s shift gears a little bit and discuss some of the psycho-social aspects of hearing loss of adult onset. It’s important to have some perspective on the entire process of hearing loss of gradual onset and how this common, chronic condition affects the attitude and behavior of the aging adult. There are several models that describe these attitudes and behaviors of adults with hearing loss. One of the more popular models is referred to as the Stages of Change model. The Stages of Change model seems to do a good job of describing how a person with age-related hearing loss adapts to the difficulties hearing loss causes over time. The six stages of change are: pre-contemplation, contemplation, determination, action, maintenance and termination. Over the last few years, research has shown that when people come into the office seeking help from the hearing care professional, very few of them are in the action stage. The Stages of Change model is relatively new to audiology, but it's a concept that is familiar to other health care professions who work with individuals with chronic conditions.
Depending on which study you read, age-related hearing loss is either the second or the third most common chronic condition among Americans over the age of 60. It's important that we study the mindset and the behavior of patients who are dealing with these chronic conditions. After all, a person can often live a long time with a non-life threatening condition that may wreak havoc with their daily existence. What this model demonstrates is that patients typically go through several stages of change before they take action. Why is this important to understand? It’s important because many of the patients that you see in your clinic are not ready to take action with regard to using hearing aids. Perhaps HyperSound could be a gateway product for these individuals.
Let’s take a closer look at the Stages of Change model. The first stage of change is the pre-contemplation stage. Pre-contemplation means the patient lacks any awareness that a problem with their hearing exists. Their spouse might complain, but the patient is in denial or completely lacks awareness of a hearing problem. They have no intent to change, because they don't even know a problem exists. During the case history, a pre-contemplator might say the problem rests with the other person (“my wife has a soft voice”) or the environment (“my TV has poor sound quality”). Recent research suggests pre-contemplators are unlikely to purchase hearing aids. However, it is possible they may be open to trying an alternative solution, especially one that doesn’t look like a hearing aid.
The next stage of change is the contemplation stage. The person is aware that they might have a problem, but they are indifferent or ambivalent. They might want to know a little bit about the pros and the cons of why they should take action. They know the problem is there, but for the most part, they are not ready to do anything about it.
Next is the preparation stage. In this stage, a person will investigate their options; they are looking for information and advice. Often, this is when patients finally search the Internet for products that might be available. Essentially, when you are in the preparation stage, you are more open to information and input from others. You are planning to take action in the near future. It is during the contemplation or preparation stage of change that the patient is open to discussing hearing aids and other treatment options.
Next is the action stage. The person is ready to take action and accept your recommendation to improve their hearing. They are prepared to change their behavior, which essentially means using a product or wearing a hearing aid. Further down the line is the maintenance stage, which holds the possibility that the person might relapse. In the hearing care profession, that might mean they stop wearing their hearing aids, or they stop following the directives of the hearing care professional. The final stage is termination, where the person is a consistent user of the treatment options. Arguably, adults with gradual hearing loss don’t fall into this category. The Stages of Change model is helpful in audiology care as we can identify the stage the patient is in and then tailor the dialogue of the appointment accordingly. In other words, meet the patient at their Stage of Change, rather than trying to force them into the preparation or action stage. The beauty of alternative solutions, like HyperSound or aural rehabilitation courses, is that because they are not hearing aids, which carry a lot of stigma, they might be viable options (or gateway solutions) for pre-contemplators or contemplators.
Earlier, I mentioned that Baby Boomers want to take a more active role in their health care. They are typically more willing to talk to a professional, or to visit websites and get more information about hearing loss. As Baby Boomers age, my prediction is we are going to see more and more patients that are in the pre-contemplation and the contemplation stages. I would argue that those are the prime patients for whom we want to discuss a range of treatment options. Knowing more about the Stages of Change model can help you to understand your patients’ needs and mindset, and, ultimately how HyperSound can benefit them.
Shared Decision Making
Four years ago, a study on shared decision making was published by audiology researchers in Europe, Australia and the United States (Laplante-Levesque, Hickson & Worrall, 2012). The shared decision-making model holds that patients want to know what their options are, and as hearing care professionals, we assist and guide them in making a decision. It helps to compare and contrast the shared decision making model with another model that many audiologists and other healthcare professional’s use, which is the paternalistic model. With the paternalistic model, during the appointment with the patient, the healthcare professional gathers information and then tells the patient what they should do. Historically that has worked well. Baby Boomers, however, usually want to be more directly involved in the decision making process, so the paternalistic approach is probably not the best approach with them. A shared decision making approach is needed.
The shared decision making approach is predicated on having alternative options or choices. Throughout my 25 years in the industry, the only choice we often provide patients is hearing aids, usually 3 or 4 levels of technology. We offer them good, better, and best hearing aid options. The exciting thing about the world today, is that other technologies exist that might be complementary or an alternative to the traditional hearing aid. Indeed, hearing aids will be the main option for many of our patients, but there are opportunities to offer other products or services. Offering several possible treatment options seems to be an important component to the shared decision making approach.
Interestingly, in the 2012 study, when patients were given a choice other than hearing aids, about half chose these other interventions. There were 289 potential participants. Of this group, 153 had a mild loss or greater and were considered eligible for intervention. They were given three options in this shared decision making paradigm. The three options were: trying hearing aids; participating in a communication program or aural rehabilitation; and, the option of doing nothing. They were asked to give it some thought. After some consideration, 43% chose hearing aids, 18% chose communication programs and 39% chose no intervention.
A noteworthy point is that regardless of the intervention option they chose (either the communication program or the hearing aids), the outcome was highly favorable. There was a 93% adherence to the intervention, with very positive results on several outcomes measures. We can surmise that when someone has more “skin in the game,” and they are able to make a decision about what they want to do, that is reflected in better outcomes. A 93% adherence number is a significantly better outcome than many other studies where the only intervention choice was hearing aids alone.
It's important to acknowledge the difference between decisions and actual uptake. Decisions are what patients are thinking about doing. Uptake is an action. According to this study, clinicians should periodically re-assess the needs of the patient every six months or so to determine if they are ready to take action on an alternative or complementary solution that might enhance their ability to hear. Also, we know that when patients are given multiple intervention options, more than half of those patients that are seeking help obtain something other than a hearing aid. In other words, many find these complementary or alternative options more appealing. Down the road, they might choose hearing aids. Patients need to know that there are several treatment options for them and it's our job to guide them through the process. HyperSound Clear can be an integral part of the shared decision making process when it is one of many possible options the patient can chose to learn more about.
HyperSound Clear Technology
Let's take a closer look at HyperSound and the television watching experience. To review, according to the US Census Department, the average American watches five or more hours of television every day. Additionally, people over the age of 65 watch seven hours of television. Thus, we know that watching television is an important leisure activity for a lot of individuals, especially those over the age of 65. According to one study (Laplante-Levesque et al., 2012), 61% of adults between the ages of 54 and 66 reported difficulty following conversations in noise (radio, television, restaurants). The HyperSound Clear 500P can help address this situation.
In Figure 2, we can see an aerial view of how the HyperSound emitters work in a typical family room with a couple seated in the room. The emitters are on either side of the flat screen TV. The person in the light gray chair has the emitters pointed at each ear. His companion is seated on the black sofa. She's able to watch the television at normal volume and he's able to listen to the television with HyperSound. Both people can listen to the same show, and there are no obstructions from other devices. They can enjoy the TV show together and have conversation during the commercial breaks, for example. Or, they could be streaming a movie, pause the movie and discuss a key scene without have to take off an amplified head set.

Figure 2. How HyperSound Clear 500P works.
The HyperSound Clear 500P could be a great way to attract new, younger patients. Think about the data in Figure 1. Seventy-five percent of Americans with hearing loss have a mild to high frequency moderate loss. It is likely that a large percentage of that group are patients under the age of 65. Most of those patients don't even acknowledge that they have a hearing loss or that they are a hearing aid candidate. Now we can offer them a product for an activity they are likely to value: watching television. They might find a HyperSound solution more appealing, because it is not a hearing aid and it addresses a very specific problem.
We also know there's a group of patients that wear hearing aids, but want to enhance their television viewing experience. Maybe their hearing aids aren't quite right for the TV or for a particular show. Other products that they might choose are complex or difficult to use. HyperSound is a great complementary product for those happy hearing aid users who want a little boost for their favorite television shows.
Finally, another group of patients who could be considered prime candidates would be “the advanced elderly” - patients who are typically over the age of 80 or 85. They are more likely to have cognitive issues, such as Alzheimer's or dementia. According to epidemiologic studies, 80% to 90% of them have some degree of hearing loss. A substantial percentage of this patient group has tried hearing aids, but they forget them, or they can't get them in their ears, and it becomes a nuisance for them to be consistently wearing hearing aids. A lot of these patients still enjoy television with their family. Sometimes they are a bit more house-bound than average. HyperSound is a prime solution for that group of patients as well.
Evidence/Studies
We conducted a patient preference study with HyperSound (Taylor, Hartenstein, & Gruttadauria, 2015). Results were extremely favorable. The research was conducted in two separate independent practices. In the study, we allowed a group of 30 to 40 patients to listen to audio through HyperSound for several minutes at a comfortable listening level. Overall, just under 70% of the participants rated the audio experience with HyperSound as very good to excellent, which is an 8 or a 9 on a 1 to 10 scale; 79% reported that speech intelligibility was markedly or tremendously improved. These patient preference studies are an incredibly positive early indication of the effectiveness of HyperSound for patients with hearing loss.
Integrating HyperSound Clear into Your Clinical Protocol
Because HyperSound is a new product category, the clinician needs to give some thought to how it is integrated into their existing patient workflow. Through experience, we have found that you simply cannot conduct a demonstration and expect people to buy it. Rather, clinicians need to present HyperSound as one of many possible solutions. Further, there are five main patient “touch points” where HyperSound Clear can be added to your existing clinical protocol:
- Appointment Booking
- Identifying the Need
- Validating the Need
- Demonstrating HyperSound Clear™
- Gaining Agreement to Purchase
Let’s take a look at each in more detail.
Appointment Booking
Once you have made the decision to become a HyperSound provider, it is beneficial to conduct some marketing activities in order to generate interest in the product. The HyperSound sales team provides several creative marketing options. After you send out the marketing mailers and people start calling you back with interest, it is important to coach your staff on how to successfully book those appointments. For example, your front office person might ask, "Are your finding that watching television is a challenge?" Be sure to schedule patients for a 30-minute demonstration. In some of our early work, we found that if we didn’t schedule at least 30 minutes, the patient was not able to fully be immersed in the technology and the sound provided by the HyperSound unit.
One of the common questions that you might get from a patient would be, "I received the mailer. How much does HyperSound Clear cost?" It’s important that you provide a range of possible costs, just as you would with hearing aids. You can modify the price range somewhat, depending on the products that are available in your practice. Also, it's important for your front office professional who fields phone calls to mention that HyperSound is state-of-the-art technology used to improve the home audio or TV viewing experience.
Identifying the Patient Need
Let’s take a look at what happens once a patient comes in to the clinic to see a provider. Identifying the patient need is critical for determining who is a prime candidate for traditional hearing aids and who might be a candidate for HyperSound. A more clinical term that I use is triaging (sorting out patients and deciding what type of intervention they might need and what their priorities are). We've come up with some tools and visuals to help you walk people through the process.
We recommend using your existing intake form, such as the COSI. These are forms where the patients can, often with your help, nominate up to five different listening situations to target for improvement. In conjunction with the intake form, some type of questionnaire is also useful to gain information. The Hearing Handicap Inventory for the Elderly (HHIE; Ventry & Weinstein, 1982) is a common survey that has been around for about 35 years. One that we recommend is called the Patient Assessment of Communication Abilities (Clutterbuck, 2015). While the patient is in the waiting area, they can fill out this very brief questionnaire. They assess a number of common listening situations and rate them on a five-point scale (1 = No Difficulty to 5 = Very Much Difficulty). Some examples of listening environments include one-on-one conversations, restaurants and watching television. At the bottom of the questionnaire, there is a place where the patient can rank order their three most challenging or important listening situations. This is a great way to obtain information from the patient in their own words using a scale. With the information from the intake forms and questionnaires, the provider can start a conversation about some of the patient’s priorities. Simply ask the patient, "Of these situations in which you are having difficulty, which one do you want to focus on first?"
Validating the Need
Once you've identified and prioritized the need, then it's important to provide some validation, or reassurance, for moving on to the next step. Most of us who have worked in this business might think of the sales process as a series of next steps. The next step means gaining agreement from the patient that you want to validate their need. That's a good time to ask some probing questions about the challenges they might face with the television, and if other family members are complaining that the volume is too loud. We want to sort out the patients for whom television is a priority, as they might be good candidates for a HyperSound demonstration. Other patients might be better off starting with traditional hearing aids. The exciting thing is now we have some options. Not everyone turns in to a hearing aid candidate. We have some complementary or alternative products that you can offer.
Here is one clinical tip: During your case history, identify who might be a pre-contemplator. Typically, these are patients who assign blame for their communication difficulties on others or on the environment. Pre-contemplators display little to no concern about getting help from hearing aids, but oftentimes still express some difficulties with communication in common places, such as at-home TV viewing. In my opinion, these are good patients to have a discussion with about the benefits of HyperSound.
In keeping with the spirit of shared decision making, we have developed another tool to help walk a patient through the spectrum of available hearing solutions. On this schematic (Figure 3), we have non-custom solutions and custom solutions.
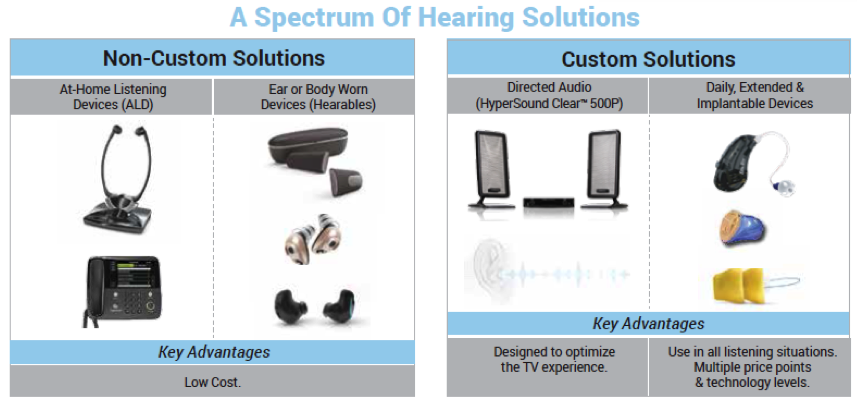
Figure 3. Non-custom vs. custom devices.
Think back to that shared decision making model. The intent is to educate the patient on all of their options. Some of these options you may not even have in your practice. That's okay, because Baby Boomers and healthy agers are likely already familiar with this technology. It's important that we acknowledge that and allow them the opportunity to guide the agenda of their appointment.
Here is how the education tool in Figure 3 works: Show the patient that there are a range of non-custom and custom solutions. Inform them of the pros and cons of each. Ask which ones they have tried or which ones they know about. Allow the patient and companion to set the agenda – where do they want to begin and what solution do they want to know more about? Rather than telling the patient what to do, the patient sets the agenda and we follow their lead. The vision aid in Figure 3 is simply an educational tool in this shared decision making process.
Talking Points: Customizable vs. Non-customizable
This is a sample script of a conversation you might have with a patient:
There are two categories of hearing solutions. The first is non-customizable solutions. Some of these solutions are designed to assist you in hearing the TV or telephone better. While they are quite affordable, the sound quality is inconsistent and uneven. Plus, non-customized solutions cannot be adjusted by a professional if your hearing or listening demands change. The second category offers customized solutions that can be programmed to your hearing needs. These tend to be more popular with patients because they provide optimal sound quality in many everyday listening situations and they often deliver much higher quality sound.
If you are sensing that a patient is not ready to use hearing aids, this is the time of the appointment where you want to start positioning HyperSound as a great alternative, and set up a demonstration.
Demonstrating HyperSound Clear
Once you've identified patients who are candidates for HyperSound based on their priorities and their needs, the next step is to conduct a demonstration. We have a detailed checklist of steps you need to take to set up the demo (Figure 4).

Figure 4. Basic setup of HyperSound Clear demonstration.
We think it's important that you enter the patient's audiogram into the HyperFit software prior to conducting the demonstration. Use the proper audio clips to demonstrate the sound quality. Compare the HyperSound audio to conventional audio, so a patient hears the difference. If you have access to YouTube with a Wi-Fi connection in your practice, we recommend using the favorite television show of your patient during the demonstration. Playing dialogue from programs with English accents, or dialogue where there are sound effects in the background, is a great way to demonstrate the speech clarity feature. Following the steps carefully will ensure proper setup, and the demonstration will elicit a “wow” effect from your patient.
The HyperSound Pivot
In many cases, patients will be prime candidates for traditional hearing aids. Unlike HyperSound, traditional hearing aids, by virtue of being worn on the ears, can be beneficial in all listening situations. However, some patients who are prime hearing aid candidates are simply not ready to pursue them. Once you recognize a patient who is a hearing aid candidate but is not yet ready, pivot the conversation. That is, rather than risk the patient leaving the appointment and doing nothing, move to a conversation about getting help for television listening. If a patient who is not ready for hearing aids reports that TV is a problem listening situation, you can ask the patient if he or she is interested in learning more about and receiving a demonstration of HyperSound. By seamlessly moving or pivoting the conversation to HyperSound you minimize the risk that a patient who is on the cusp of taking action to get help will delay receiving help of any kind for several months or years.
HyperSound as a Gateway Product
Hearing aids have a relatively low uptake rate. Reasons for this include cost, stigma, and negative word-of-mouth. Additionally, people with milder hearing loss may have only situational difficulties that preclude the use of hearing aids. Regardless of the specific reason, HyperSound may be a gateway to eventual hearing aid use. For individuals with mild losses and/or situational listening difficulties, HyperSound may be effective for TV viewing (if it’s a problem) until the hearing loss worsens. For individuals with more substantial hearing loss who are simply not ready to wear hearing aids for whatever reason, HyperSound may also be a gateway to eventual hearing aid acceptance. By addressing a specific need sooner with HyperSound, it is presumed individuals may transition to hearing aid user sooner. We need evidence to support this point, but the theory is that HyperSound improves the TV viewing experience so much, that other places where the patient struggles with hearing become magnified. That is, the contrast between hearing the TV well with HyperSound and other listening places becomes greater and hastens the use of hearing aids.
Gaining Agreement to Purchase
Once you have demonstrated the product, and the patient is ready to proceed with acquisition of it, it's important to transition into gaining agreement to purchase the product. Here are some effective ways to gain agreement from the patient:
Option 1: I have a HyperSound Clear™ available. Would you like to bring it home today?
Option 2: I realize this is a big purchase for you, so if you like, you can try HyperSound Clear™ for free at home for two weeks. If it’s not working out for you after two weeks, you can simply return it. Would you like to give it a try?
Offering a free trial alleviates the pressure to purchase. It is a nice way to reduce the risk involved with trying this state-of-the-art product. Those who try it for free are likely to want to keep it based on our early experiences.
Becoming a HyperSound Provider
I’m going to go through, at a very high level, how we onboard new clinics that sign up to be a HyperSound provider. As I've already mentioned, it's important to have a demonstration day. Prior to the demonstration day, make sure that everyone in your clinic has been trained, and that the demonstration has been set up. Double-check that your front office staff has been coached on how to answer questions and how to book patients for the 30-minute appointment.
When we onboard new clinics using HyperSound for the first time, we help ensure the office workflow is not disrupted, that the professionals in the office are up to speed on the basics of the product, and that they have determined where and how the demo will be conducted. We have effective processes in place for the training day, as well as for the demo day.
We have created some marketing collateral that you can use. These tools are located on our website: https://HyperSoundhearing.com/. Click the “Professionals” tab to find the tools. We have created a very effective and sophisticated process for integrating HyperSound into your practice with education, marketing and a demo day.
After the demo day is over, we ensure that you continue to be successful in your practice. We have a 12-week onboarding plan summary that outlines the different stakeholders as well as the follow up and maintenance duties that need to be implemented. At the end of 12 weeks, there is a review that consists of a 30-minute meeting with the practice owners to make sure that things are working well. We recognize that every practice is unique in the way that they work with patients. We have enough flexibility within our protocol to accommodate these differences in order to help all practices be successful.
Summary
The shared decision making process is a key element in helping to introduce HyperSound, especially to your Baby Boomer patients. We can expand our breadth of service by offering validated complementary and alternative devices, such as HyperSound.
As the market changes, it is important to have solutions like HyperSound as an integral part of your product portfolio. It's a great way to open doors and complement your existing business. You have the ability help more patients, and to also grow your own revenues and profits.
However, just like any product, HyperSound doesn’t sell itself. It requires everyone’s diligence and hard work to make sure HyperSound is successfully integrated into your office protocol. Please know that we are here to support you every step of the way.
Questions and Answers
What if more than one person in the family needs the device?
You could buy two devices and they could each have one of their own, but that's probably not very realistic. HyperSound is programmable, like a hearing aid. It has multiple memories like a hearing aid. With the remote control on your HyperSound device, for Person One, you could set it (tune it) for his hearing loss, and for Person Two, you could set it for her hearing loss. The disadvantage of that is they would have to be watching TV individually, and that may not be so good. If they want to watch television together, you could program one emitter for one person and one emitter for the other. You narrow the beam and that might be one workaround. I think with the programmability of the product and the fact that there are two emitters, you can handle a lot of those unique situations. The bottom line is that to optimize the performance of HyperSound, one HyperSound unit per listener is needed.
What would the first step be?
I think the first step for a patient would be booking an appointment for a demo. I would encourage you to meet with your HyperSound rep to develop a protocol around that first step. It is important when booking an appointment to give patients a range of prices, and to strongly encourage them to come in and have a 30-minute demonstration of this state-of-the-art technology.
References
Clutterbuck, S. (2015). Another tool for assessment of communication needs? Try the TRACA: Their Reported Assessment of Communication Abilities. Audiology Practice, 7(1),16-19.
Laplante-Levesque, A., Hickson, L., & Worrall, L. (2012). What makes adults with hearing impairment take up hearing aids or communication programs and achieve successful outcomes? Ear and Hearing, 33(1), 79-93. doi: 10.1097/AUD.0b013e31822c26dc
Taylor, B., Hartenstein, R., & Gruttadauria, S. (2015). Patient preferences for a directed audio solution. Hearing Review, 22(10), 28.
Tremblay, K.L., Pinto, A., Fischer, M.E., Klein, B.E., Klein, R., Levy, S., et al. (2015). Self-reported hearing difficulties among adults with normal audiograms: The Beaver Dam Offspring Study. Ear and Hearing, 36(6), e290-299. doi: 10.1097/AUD.0000000000000195
Ventry, I. & Weinstein, B. (1982). The Hearing Handicap Inventory for the Elderly: A new tool. Ear and Hearing, 3,128-134.
Citation
Taylor, B. (2016, July). Growing your business with HyperSound. AudiologyOnline, Article 17612. Retrieved from www.audiologyonline.com


