Introduction
Hearing aids are generally fit based on the type and degree of hearing loss, not etiology. However, in medically complex cases, hearing loss is only one manifestation of an underlying and ongoing disease process impacting the anatomic and physiologic status of the auditory system.
Essentially all non-linear hearing aid fitting rationales are based on a model of outer and inner hair cell loss, resulting in changes in loudness perception, "corrected" via the chosen hearing aid fitting rationale (i.e., hearing aid prescription). For reasonably stable and/or slowly progressing etiologies such as presbyacusic or noise-induced hearing loss, this model is sufficient. Gain and compression calculations based on hair cell loss attempt to restore or equalize loudness while maximizing audible speech information. These prescriptions are based on the assumption that "measurable hearing is usable hearing," and that if "speech is made audible (above threshold and above the background noise), it is made useful" for the patient. Although the above assumption is valid for the majority of patents fit with hearing aids (those with sensory presbyacusic and/or noise-induced hearing loss), it may not be as valid for patients with medically complex hearing loss etiologies.
The term "medically complex" as used here, refers to patients with etiologies such as Meniere's disease and related inner ear abnormalities (endolymphatic hydrops, cochlear Meniere's disease, sudden sensorineural hearing loss, cochlear hydrops, etc.). However, other "non-otologic" etiologies such as systemic disease, can negatively impact the auditory system, and these, too, are considered medically complex hearing losses. For example, patients with autoimmune disease, multiple sclerosis, cytomegalovirus, a multitude of oncologic diseases and importantly, those on pharmacologic regimens requiring ototoxic medications, are considered medically complex.
The most common medically complex hearing loss the audiologist manages is usually from Meniere's Disease. Meniere's Disease serves as an excellent example of the potential range of signs and symptoms the patient may present with: fluctuating hearing loss, rising audiometric configurations, unilateral or asymmetric sensorineural hearing loss, reduced word recognition scores and reduced dynamic ranges, vertigo, aural fullness and/or aural pressure and unilateral tinnitus (Johnson & House, 1979; Valente et al., 2006). These patients are challenging and often require additional insight, resources and aural management techniques to achieve successful hearing aid fittings. Therefore, we believe traditional hearing aid fitting rationales may be less applicable to "medically complex" patients.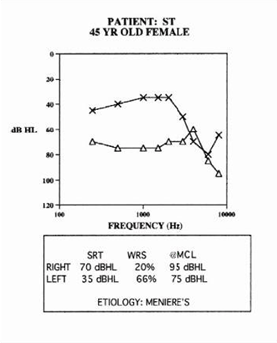
Figure 1. An example of a patient with a medically complex etiology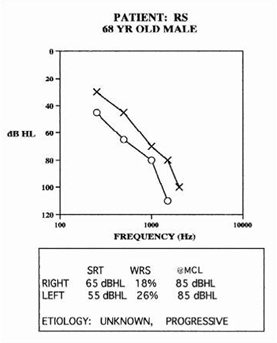
Figure 2. A second example of a patient with a medically complex etiology.
Figures 1 & 2 provide example profiles of two medically complex patients. In this article, we will review management strategies to help guide the hearing aid fitting process for patients with medically complex hearing loss.
An Alternative Fitting Strategy
Schum & Beck (2006) introduced the concept of Residual Capabilities. Residual Capabilities can be thought of as a hearing aid fitting philosophy which maximizes the relationship between the daily acoustic environments the patient experiences and the remaining hearing abilities (i.e., residual capabilities) of the patient. In the Residual Capabilities model, the hearing aid serves as the facilitator to enhance the relationship between the patient and their world of sound. Each patient is recognized as having their own unique auditory needs. Therefore, the hearing aid serves as a conduit to best match the patient's needs to the sounds of greatest interest, typically human speech.
When medically complex etiologies cause disruptions and abnormalities within the auditory system beyond inner and outer hair cell loss, it is important to understand that the ideal hearing aid fitting rationale may not include loudness and audibility restoration. Rather, the Residual Capabilities philosophy focuses on how to make the most of the remaining hearing for each unique patient.
In recent years, attention has been paid to the possibility of "dead zones" within the inner ear (Moore, 2003). In cases in which dead zones are identified or suspected, it has been recommended to avoid amplification within those regions (Flynn & Schmidtke, 2002). The re-evaluation and recognition of dead zones (Moore, 2003) is a good example of how our profession critically reviews and has updated hearing aid fitting protocols away from simply fitting amplification to all obtainable thresholds, to carefully exploring and critically evaluating what works best and why.
Characteristics of Medically Complex Disorders
As noted above, we define medically complex hearing disorders based on dynamic physiologic and anatomic changes which impact the auditory system. Nonetheless, there are some commonalities across medically complex hearing loss presentations.
One of the most common audiologic characteristics of medically complex presentations is reduced word recognition performance. In general, patients with sensorineural hearing (SNHL) loss, from mild to moderate (or even severe) have good to excellent word recognition performance in quiet, when words are presented at comfortable supra-threshold levels. In addition, the performance-intensity function (the relationship between percent correct as a function of presentation level) is normally monotonic. In the case of Meniere's Disease, for example, the maximum word recognition score may be reduced and the performance-intensity function may show roll-over or other abnormalities (Clemis & Johnson, 1967; Hood, 1984).
Another common audiologic characteristic of the medically complex patient, especially those with Meniere's Disease, is abnormal loudness growth functions (Johnson & House, 1979). Nearly all patients with stable SNHL demonstrate reduced dynamic ranges. For example, patients with mild to moderate hearing loss typically have dynamic ranges on the order of 50 to 70 dB. Patients with moderate-to-severe hearing losses often have at least 40 dB dynamic ranges. However, Meniere's and other medically complex patients may demonstrate extremely steep loudness growth functions with dynamic ranges of only 10 to 30 dB.
The third observed audiologic characteristic of some patients with medically complex disorders is an excessive spread of masking. Most patients with typical SNHL experience an upward spread of masking, especially at higher presentation levels. However, patients with medically complex disorders may show masking patterns in which a low frequency stimulus may affect thresholds 2 octaves above the stimulus (Schum, 1995).
Patients with medically complex hearing disorders demonstrate instability within their peripheral auditory system. An insult to the auditory system can disrupt the intricate, delicate and dynamic functions of the inner ear and associated neural pathways. Distortion and other auditory degradation can occur. In some cases, the status of the auditory system may be in flux for many years. However, even in patients with stabilized Meniere's, the auditory system does not process complex signals, such as speech, accurately or effectively.
Candidacy
Unfortunately, some audiologic and otologic training materials have discouraged fitting amplification on medically complex patients. However, little clinical or scientific evidence has been presented to support those notions. Nonetheless, case examples exist which specifically demonstrate that medically complex patients can be appropriately and satisfactorily fit, often using a hearing aid fitting philosophy such as, or similar to, Residual Capabilities.
Feldman and Oviatt (1993) presented the case of an 84 year old patient with a sloping mild-to-severe SNHL with good word recognition in the left ear, and a flat, severe SNHL with no word recognition in the right ear. The patient had a long history of hearing aid use on the left ear, but never used amplification on the right ear. The audiologists fit the right ear and gave the patient several weeks to adapt to amplification in the previously unaided ear. Upon follow-up, soundfield word recognition testing was performed in quiet and at +10 dB S/N. The patient scored 76% and 56% in quiet and noise (respectively) with the hearing aid only on the left ear. However, with the binaural fitting, word recognition scores improved to 92% and 88%. The additional hearing aid on the ear with no measurable speech understanding (under headphones) allowed a significant improvement in both quiet and noise.
This case demonstrates the potential dis-service to the patient, which could have occurred, based on arbitrary exclusionary amplification rules. Our understanding of auditory processing in medically complex ears is so rudimentary, that the only true test is often a trial hearing aid fitting. Hearing aid fittings are fully reversible with no lasting negative side effects. Therefore, we believe it is difficult to justify not engaging a hearing aid trial in this, and other medically complex, cases.
It is equally important for the audiologist to ensure that the patient approaches the hearing aid fitting process with realistic expectations (Valente et al. 2006). The dramatic improvement demonstrated by the patient presented by Feldman and Oviatt (1993) is probably the exception, not the rule. With dramatic changes to the auditory system, it is important for both the professional and patient to recognize that amplification cannot restore many of the complex signal processing abilities of the normally functioning system.
Role of Nonlinear Processing
Many patients who present with medically complex hearing losses have hearing thresholds in the severe range. Given this degree of hearing loss, often the first inclination is to fit them with powerful linear hearing aids. However, for many of these patients, the better solution is to use advanced technology multi-channel, nonlinear fittings. Medically complex patients with severe hearing loss often use significantly less gain than would be expected based on their hearing thresholds and often will only tolerate highly compressed sounds at a low audibility level.
Schum (1995) studied a group of 15 patients with a variety of medically complex disorders, including Meniere's Disease, progressive idiopathic losses and retro-cochlear disorders. Patients were fit with nine different hearing aid processing strategies. Five were linear strategies with multiple bandwidths and four were nonlinear strategies. Each of the 15 patients evaluated all nine options in a comprehensive round-robin format. Performance was evaluated using a panel of 18 different objective and subjective measures.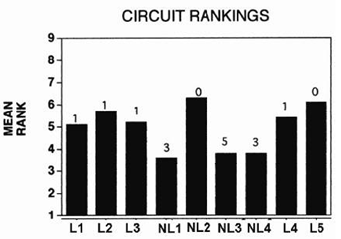
Figure 3. 15 subjects mean rankings (lower score is better) across 9 signal processing approaches and their preferred signal processing strategy.
Figure 3 presents the average rankings across the 18 measures by the 15 patients. Three of the options (NL1, NL3 & NL4) grouped together with significantly lower (i.e., better) average rankings. Patients were allowed to pick which signal processing strategy they wanted for their "permanent" hearing aid. The numbers above each bar indicated the number of subjects who chose each of the processing strategies. Eleven of the 15 subjects chose one of the three highly ranked non-linear strategies. NL1 was a Treble Increase at Low Levels (TILL) (Killion, Staab & Preeves, 1990) circuit, NL3 was a two channel WDRC device and NL4 was a three channel WDRC device.
A retrospective evaluation of the gain levels used by those 11 patients indicated they typically used between 5 and 15 dB less gain for soft inputs in the mid-to-high frequencies than NAL-NL1 prescribed.
The Fitting Process
Since the nature of the medically complex hearing loss is different from the more typical SNHL fit with amplification, the medically complex process will be different, too.
Measuring Improvement: Given the severity of the abnormalities and disruptions in the medically complex auditory system, the patient may not meet traditional performance standards when aided. Although the patient presented by Feldman and Oviatt (1993) demonstrated aided benefit on a traditional performance measure (soundfield word recognition), this may not always be the case. Often and appropriately, the patient will be the final arbiter regarding the benefit provided by amplification and their final analysis or judgment criteria may not be predictable. Perhaps it will relate to comfortable loudness, sound quality, recognition of words, environmental sounds or even sound awareness. Although their final analysis and judgment criteria may not be predictable, it is always significant and tangible to the patient.
Verifying benefit: As discussed previously, traditional prescribed targets may not be relevant in many medically complex fittings. Therefore, matching real ear targets may not be of paramount importance. Nonetheless, real ear verification is recommended, so an objective determination and recording of successful and unsuccessful processing strategies is obtained for analysis and is available for comparison at a later date.
Importantly, speech understanding may not necessarily be improved by a "successful" hearing aid fitting. From the perspective of the medically complex patient, sometimes improved localization or a qualitative improvement allowing improved differentiation of speech from other sounds is of significant importance. Nonetheless, objective measures to verify hearing aid fittings should be considered. Sometimes, tests originally developed for cochlear implant patients such as discrimination of noise-voice, sentence understanding or audio-visual perception are useful in evaluating aided versus unaided performance in these patients.
Binaural vs. Monaural Strategies
Although consensus appears to be that audiologists generally fit bilateral hearing loss with binaural amplification to offer the full range of binaural advantages (Noble, 2006), there are times when the hearing aid fitting process may be better served by fitting only one ear (Jerger & Silman, 1993) or, by fitting one ear maximally, and then re-evaluating.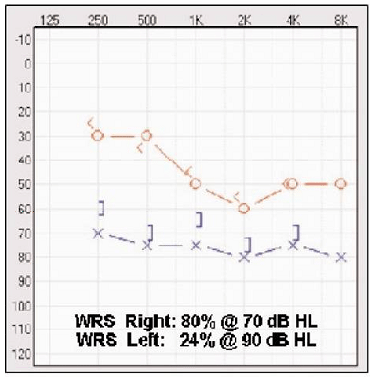
Figure 4. Audiogram of patient fitted with amplification on right ear first, with left hearing aid added two months later.
Figure 4 presents the audiogram from a patient with stable hearing loss from Meniere's Disease. One strategy is to treat this case as two monaural fittings. Given the asymmetry, one assumes if the hearing continues to remain stable, the patient will primarily rely on her right ear. Assuming that's true, the right ear fitting must be as effective as possible. Once a maximal right ear fitting has been achieved, the audiologist may fit the left ear to see if it adds to the overall auditory performance or experience of the patient. Although fitting the left ear may prove useful, it is unlikely to become as useful for the patient as is the right ear. Rather, the goal here may be to achieve a solution in which the right ear is fit optimally, while the left ear successfully provides additional assistance without competing with, or distracting from, the right. As noted above, the traditional prescription for the left ear may not be relevant as full restoration (based on the threshold hearing loss in the left ear) may compete with or reduce the word recognition of the right ear.
In the above case, the audiologist started with a multi-channel, non-linear power BTE in the right ear. Although the device was not required based on current hearing thresholds (see audiogram), extra gain and output may be needed if the hearing thresholds decrease. After two months of adjustments and adaptation, the audiologist added a matched hearing aid on the left ear based on the left ear's hearing thresholds. However, it was assumed that that much power would not be needed given the etiology and the philosophical approach to the left ear as the "secondary" ear. The patient went through three follow-up sessions to fine-tune the left hearing aid and currently uses between 5 and 10 dB less than prescribed gain. The patient reports a clear but non-specific advantage when using both hearing aids, as compared to using just the right. She uses both devices while at work, although at home, she occasionally uses just the right device.
Significant asymmetrical SNHL may best be seen as two different fittings, with a dominant ear and a "secondary" ear. Achieving the best possible fitting on the dominant ear should occur first, with intentional and cautious addition of the secondary ear, in a step-wise and evaluative manner, consistent with the Residual Capabilities philosophy.
Final Thoughts
The traditional approach to fitting hearing aids is based on a predictive model. Audiologists establish hearing thresholds and perhaps other measures such as MCL and UCL and loudness growth characteristics. The acquired data is entered into a fitting rationale algorithm and a hearing aid fitting target is derived. Variations and corrections away from these targets are made if the patient provides negative subjective reactions or requests additional fine-tuning.
When fitting patients with medically complex disorders, the audiologist and patient benefit from a more adaptive model. It can be assumed from the outset that for medically complex fittings, initial prescriptive targets based on threshold and loudness data may not be close to the ideal or optimized setting and that indeed, final settings may change over time as the hearing disorder evolves. Programmability and multiple memories are important considerations for these patients.
It is clear that managing medically complex hearing loss is more challenging than managing typical noise induced or presbyacusic hearing loss. Patients with medically complex hearing loss are extremely handicapped and tend to be very appreciative of any assistance the audiologist can provide. Although the process of finding optimized settings may be frustrating to the patient and audiologist, finding the right solution can be an extremely satisfying professional experience.
Please Note: This article was provided by Oticon to audiology graduate students as a special supplement to the Hearing Journal, July, 2006.
References
Clemis, J. & Carver, W. (1967). Discrimination scores for speech in Meniere's Disease, Archives of Otolaryngology, 86, 614-618.
Feldman, A. & Oviatt, D. (1993). BiCros or binaural: A case study. Seminars in Hearing, 14(3), 229-233.
Flynn, MC, & Schmidtke, TE (2002). Four fitting issues for severe and profound hearing impairment. The Hearing Review, 9(11), 28-33.
Hood, J. (1984). Speech discrimination in bilateral and unilateral hearingloss due to Meniere's Disease. British Journal of Audiology, 18, 173-177.
Jerger J, Silman S, Lew HL, Chmiel R. (1993). Case studies in binaural interference: converging evidence from behavioral and electrophysiologic measures. Journal of the American Academy of Audiology, 4, 122-31.
Johnson, E. & House, J. (1979). Meniere's Disease: Clinical course, auditory findings and hearing aid fittings. Journal of the American Auditory Society, 5, 76-83.
Killion, M., Staab, W. & Preeves, D. (1990). Classifying automatic signal processors. Hearing Instruments, 41(8), 24-26.
Moore, B. (2003). An Introduction to the Psychology of Hearing. 5th Ed. San Diego: Academic Press.
Noble, W. (2006): Benefits of Fitting One Versus Two Hearing Aids. ASHA Leader, March 21, pp. 6-32.
Schum, D. (1995). Amplification options for severe distortional hearing loss. Final report to the U.S. Department of Education.
Schum, D. & Beck, D. (2006). March 2006. Alternative Fitting Approaches for Special Populations. News From Oticon.
Valente, M, Mispagel, K, Valente, L.M. and Hullar, T. (2006) : Problems and Solutions for Fitting Amplification to Patients with Meniere's Disease. Journal of the American Academy of Audiology, 17, 6-15.
Amplification and Medically Complex Hearing Loss
October 9, 2006
This article is sponsored by Oticon.
Related Courses
1
https://www.audiologyonline.com/audiology-ceus/course/oticon-government-services-may-2023-38919
Oticon Government Services May 2023 Contract Update
Oticon understands that sudden, disruptive sounds affect a large majority of hearing aid users, making it difficult to stay sharp and focused – especially when engaged in conversation. Oticon Real™ is designed to help with this challenge and keep patients engaged. In this course we introduce new options on the VA hearing aid contact.
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Oticon Government Services May 2023 Contract Update
Oticon understands that sudden, disruptive sounds affect a large majority of hearing aid users, making it difficult to stay sharp and focused – especially when engaged in conversation. Oticon Real™ is designed to help with this challenge and keep patients engaged. In this course we introduce new options on the VA hearing aid contact.
38919
Online
PT60M
Oticon Government Services May 2023 Contract Update
Presented by Kirstie Taylor, AuD
Course: #38919Level: Intermediate1 Hour
AAA/0.1 Intermediate; ACAud inc HAASA/1.0; ASHA/0.1 Intermediate, Professional; BAA/1.0; CAA/1.0; IACET/0.1; IHS/1.0; Kansas, LTS-S0035/1.0; NZAS/1.0; SAC/1.0
Oticon understands that sudden, disruptive sounds affect a large majority of hearing aid users, making it difficult to stay sharp and focused – especially when engaged in conversation. Oticon Real™ is designed to help with this challenge and keep patients engaged. In this course we introduce new options on the VA hearing aid contact.
2
https://www.audiologyonline.com/audiology-ceus/course/why-evidence-matters-38163
Why Evidence Matters
Oticon has a long history of focusing on innovative research into how the brain processes sound and how technology can support the brain’s natural ability to process sound. In this course we will review evidence supporting Oticon’s technology developments and how hearing care professionals can use this information to discuss benefits and explain why they are recommending Oticon solutions.
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Why Evidence Matters
Oticon has a long history of focusing on innovative research into how the brain processes sound and how technology can support the brain’s natural ability to process sound. In this course we will review evidence supporting Oticon’s technology developments and how hearing care professionals can use this information to discuss benefits and explain why they are recommending Oticon solutions.
38163
Online
PT60M
Why Evidence Matters
Presented by Lana Ward, AuD
Course: #38163Level: Intermediate1 Hour
AAA/0.1 Intermediate; ACAud inc HAASA/1.0; AHIP/1.0; ASHA/0.1 Intermediate, Professional; BAA/1.0; CAA/1.0; IACET/0.1; IHS/1.0; Kansas, LTS-S0035/1.0; NZAS/1.0; SAC/1.0
Oticon has a long history of focusing on innovative research into how the brain processes sound and how technology can support the brain’s natural ability to process sound. In this course we will review evidence supporting Oticon’s technology developments and how hearing care professionals can use this information to discuss benefits and explain why they are recommending Oticon solutions.
3
https://www.audiologyonline.com/audiology-ceus/course/oticon-government-services-introducing-more-36630
Oticon Government Services: Introducing Oticon More
Sound scenes are dynamic, complex and unpredictable. It is the role of the brain to handle this complexity to hear and make sense of it all. Oticon is committed to developing life changing technologies that support the way the brain naturally processes sound. Get ready to discover the new perspective in hearing care with a fundamentally new approach to signal processing. *This is a recording of the VA Oticon More Introduction Event from May 3, 2021*
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Oticon Government Services: Introducing Oticon More
Sound scenes are dynamic, complex and unpredictable. It is the role of the brain to handle this complexity to hear and make sense of it all. Oticon is committed to developing life changing technologies that support the way the brain naturally processes sound. Get ready to discover the new perspective in hearing care with a fundamentally new approach to signal processing. *This is a recording of the VA Oticon More Introduction Event from May 3, 2021*
36630
Online
PT60M
Oticon Government Services: Introducing Oticon More
Presented by Candace Depp, AuD, Thomas Behrens, MS, Danielle Tryanski, AuD, Sarah Draplin, AuD
Course: #36630Level: Intermediate1 Hour
AAA/0.1 Intermediate; ACAud inc HAASA/1.0; AHIP/1.0; BAA/1.0; CAA/1.0; IACET/0.1; IHS/1.0; Kansas, LTS-S0035/1.0; NZAS/1.0; SAC/1.0
Sound scenes are dynamic, complex and unpredictable. It is the role of the brain to handle this complexity to hear and make sense of it all. Oticon is committed to developing life changing technologies that support the way the brain naturally processes sound. Get ready to discover the new perspective in hearing care with a fundamentally new approach to signal processing. *This is a recording of the VA Oticon More Introduction Event from May 3, 2021*
4
https://www.audiologyonline.com/audiology-ceus/course/genie-2-fitting-focus-series-36119
Genie 2 Fitting Focus Series: Oticon More First Fit
In this course we will cover the initial fitting steps for a successful Oticon More initial fitting using Oticon’s Genie 2 fitting software.
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Genie 2 Fitting Focus Series: Oticon More First Fit
In this course we will cover the initial fitting steps for a successful Oticon More initial fitting using Oticon’s Genie 2 fitting software.
36119
Online
PT30M
Genie 2 Fitting Focus Series: Oticon More First Fit
Presented by Amanda Szarythe, AuD, CCC-A
Course: #36119Level: Intermediate0.5 Hours
AAA/0.05 Intermediate; ACAud inc HAASA/0.5; AHIP/0.5; BAA/0.5; CAA/0.5; IACET/0.1; IHS/0.5; NZAS/1.0; SAC/0.5
In this course we will cover the initial fitting steps for a successful Oticon More initial fitting using Oticon’s Genie 2 fitting software.
5
https://www.audiologyonline.com/audiology-ceus/course/counseling-techniques-supporting-standard-care-38697
Counseling Techniques Supporting Standard of Care
Effective counseling practices make a tremendous difference in hearing healthcare. Being able to communicate the benefits of advanced technology in simple language patients can understand is the key element in this process. This course will provide suggestions for consumer-friendly language based on clear benefits when making a strong recommendation for premium technology as the standard of care.
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Counseling Techniques Supporting Standard of Care
Effective counseling practices make a tremendous difference in hearing healthcare. Being able to communicate the benefits of advanced technology in simple language patients can understand is the key element in this process. This course will provide suggestions for consumer-friendly language based on clear benefits when making a strong recommendation for premium technology as the standard of care.
38697
Online
PT60M
Counseling Techniques Supporting Standard of Care
Presented by Amanda Greenwell, AuD
Course: #38697Level: Intermediate1 Hour
AAA/0.1 Intermediate; ACAud inc HAASA/1.0; AHIP/1.0; ASHA/0.1 Intermediate, Professional; BAA/1.0; CAA/1.0; IACET/0.1; IHS/1.0; Kansas, LTS-S0035/1.0; NZAS/1.0; SAC/1.0
Effective counseling practices make a tremendous difference in hearing healthcare. Being able to communicate the benefits of advanced technology in simple language patients can understand is the key element in this process. This course will provide suggestions for consumer-friendly language based on clear benefits when making a strong recommendation for premium technology as the standard of care.



