Ear Prosthesis Overview:
Craniofacial defects may result from congenital conditions, ablative tumor surgery, or trauma. The ear, orbit, or nasal/midface may be affected. These defects create esthetic, functional, and psychosocial problems for the patient. Surgical reconstruction using autologous tissue is the most natural method of replacement. This requires multiple surgeries over a period of time. In some cases, surgical reconstruction is not possible.
The uniqueness of the area involved may prove too difficult to reconstruct with autologous tissue. In the case of a missing eye, there is not an autologous replacement and reconstruction of the orbit is difficult. Nasal reconstruction is possible but as with other facial procedures, symmetry and fine detail of the reconstructed area is difficult to achieve.
Reconstruction of a congenitally missing ear or one lost to trauma using rib cartilage grafts is difficult given the complexity of the reshaping of the cartilage in order to mimic the three dimensional shape of the opposite ear. There is no description in the literature of reconstruction of an ear missing due to tumor surgery.
In cases of cancer, surgical reconstruction is often deferred due to concerns for recurrence or never attempted. If loss of the ear is due to trauma, the defect may lack adequate soft tissue to perform surgery. In the case of a congenitally missing ear, surgical reconstruction is most common but the result may not be acceptable to the patient. In other situations, the patient's health may preclude the multiple surgical procedures required for autologous ear reconstruction or the patient may simply opt not to have additional surgery. Prosthetic rehabilitation is a viable alternative to surgical reconstruction.
Accounts of prostheses to replace the ear date back several centuries.1 Today, aural prosthesis are made of medical grade silicone rubber and the shape and color are customized for each patient. These prostheses contribute to the restoration of functional, cosmetic and psychological normalcy.
In the past, these prostheses have been retained with skin adhesives. While adhesives provided a reliable means of retention, they have several problems. The application of the adhesive may be messy and time-consuming. The edges of the prosthesis must often be thickened or reinforced with fabric to resist tearing that may occur as the adhesive is cleaned from the prosthesis on a daily basis. This may detract from the appearance of the prosthesis. The adhesive may cause skin irritation, particularly in those patients who have undergone radiation therapy. Retention by the skin adhesive may be unreliable, especially if the prosthesis is large, the weather humid, or if the patient has oily skin. Proper positioning of the prosthesis is difficult in the absence of key anatomical landmarks; especially if the patient has compromised manual dexterity or visual acuity.
Branemark (1985) a Swedish orthopedic surgeon defined "osseointegration" as a direct structural and functional connection between ordered living bone and the surface of a load-carrying implant.2 This phenomenon was based on his bone healing research begun in the 1950s. In 1965, the principles of osseointegration were applied to dental implants and this procedure has been widely recognized as safe and effective.3
In 1983, Tjellstrom published results regarding osseointegrated implants to retain auricular prostheses and also, bone-conducting hearing aids.4 In 1995, osseointegrated implants were determined to be safe and effective for this application by the United States Food and Drug Administration (FDA). This decision was based on the results of the study, "Bone Anchored Craniofacial Prosthesis Study"5 of which The Craniofacial Center at the University of Illinois Medical Center was a participant.
Implant retention offers several advantages over skin adhesives. For example; there is less wear and tear on the prosthesis, and daily cleaning is faster and easier. Both of these factors contribute to extended life of the prosthesis. Additionally, adhesive related skin irritation is eliminated and implants provide more reliable retention of the prosthesis.6 Precise placement of the prosthesis is assured as the retentive elements automatically guide the prosthesis to its correct position. Implant-retained auricular prostheses have been used successfully in cases where the pinna is missing.
The Baha System:
Osseointegrated implants offer another benefit. These protocols may be used to retain a bone conducting hearing aid. The Baha, manufactured and distributed by Cochlear Corporation is an alternative hearing device for patients unable to use conventional hearing instruments. Patients include those with medically untreatable conductive hearing losses (e.g., bilateral atresia, chronic middle ear problems, etc.). In addition, the FDA has recently approved the Baha for patients with unilateral sensorineural hearing loss, as an alternative to using CROS hearing aids.
Traditionally, bone conduction hearing aids have been recommended for selected patients with specific etiologies, such as those mentioned above. It is not unusual for patients to report that traditional bone conduction systems are cumbersome and uncomfortable as they historically included a body-worn device coupled to a bone oscillator held in place by a headband. The headband requires significant pressure for the transmission of sound from the bone oscillator through the skin, to the skull and inner ears. Even when properly fitted the sound is naturally attenuated in the high frequencies as it passes through the skin. Since the Baha is a surgically-implanted device, with a removable external sound processor, these concerns are eliminated.
For patients with unilateral sensorineural hearing loss, the Baha is placed on the side with the hearing loss. The sound is routed from the microphone on the side of the "bad" ear to the "good" ear via bone conduction. A previous approach to this type of hearing loss has been the "transcranial CROS." The transcranial CROS uses a power hearing aid worn deep in the canal on the "bad" side, and the amplified sound travels to the "good" ear via bone conduction. Interestingly, with the surgically implanted Baha, interaural attenuation is not a factor. Interaural attenuation is only an issue when the sound is delivered by air conduction, which is not the case with a surgically implanted bone conduction device.
The Baha has several advantages over the traditional bone conduction hearing aid set-up. First and foremost, this device has been shown to provide better hearing. Tjellstrom and Jakansson compared the Baha to conventional bone conduction hearing aids and reported better word discrimination in quiet and in noise with the Baha.7 Second, it is more comfortable, as there is no need for a headband or additional body worn components. The contact point (a small abutment) is placed in bone in the mastoid area, just above the hairline, so the device is entirely hidden by medium to long hair and is more discrete than traditional head band based bone conduction and/or CROS systems.
Patient Selection and Audiometric Issues:
The patient is evaluated for an implant-retained prosthesis by a rehabilitative team that includes a surgeon, prosthodontist, anaplastologist and an audiologist.
Preoperative audiologic testing is performed to confirm the patient is a candidate for such treatment. An audiogram is necessary to determine whether the patient has sufficient bone-conducted hearing and word recognition to use the device successfully. A bone-conducted four-frequency (500, 1k, 2k, 3k) PTA of less than 45 dB HL and word recognition score of greater than or equal to 60% for PB words is preferred. The patient may also have an in-office trial with the device by using a special test rod that is held between the teeth. This is the best approximation of the effect of having direct bone conduction hearing. The procedure for surgery and application of the hearing aid are explained to the patient. In selected instances a patient may be a candidate for both an implant-retained auricular prosthesis and a Baha.
Surgical placement of the Baha is based on a standard measurement and direction from the external meatus; 50-55mm from the ear canal at the 10 o'clock position on the right side or the 2 o'clock position on the left. This position may have some variability; especially in congenital cases where the position of the meatus and/or hairline may be altered. Surgical positioners may be used intraoperativley as guides for implant locations for both the Baha and ear prosthesis.8 In any event, the Baha must be positioned so that it does not touch the pinna of the ear. The surgical procedures are performed on an outpatient basis. See photo ONE.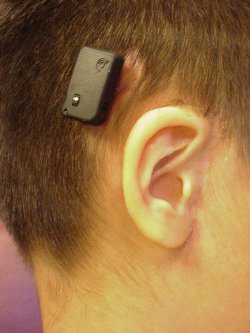
Figure 1. BAHA and ear prosthesis in place. NB. With long hair, BAHA is less noticeable. (Prosthesis by Susan Habakuk)
For the Baha, the skin must also be thinned to accommodate the single 5.5mm height of the abutment that connects the implant through the skin. This too is for hygiene considerations and for comfort while wearing the hearing aid. A special dermatome has been designed by Entific Medical Systems for this use. Following abutment placement, ear prosthesis fabrication or placement of the Baha may occur. The Baha requires a single implant while an ear prosthesis requires 2-3 implants.
Fitting and instruction regarding use of the Baha external device, and post-fitting testing and audiologic follow-up is performed by the audiologist. The patient is instructed on day to day use of the instrument, proper cleaning, use of the volume control, batteries and replacement. In addition, adjustments can be made to the frequency response of the device via a trimpot. Soundfield audiometry with volume set to the patient's most comfortable level (MCL) is recommended. Measurement of word recognition in noise performed at 70 dB SPL with a +10 signal to noise ratio is also a recommended measure of the efficacy of the device. These post-fitting checks and any subsequent adjustments in frequency response/volume control setting should be performed at 3 and 6 months post-fitting to allow for adequate patient adjustment to the device.
For the ear prosthesis, the patient is likewise instructed on its placement, removal, and care. Daily hygiene instructions for the prosthesis and the skin are also given.9 The prosthesis and skin are checked on a 6-month basis.
A soft headband is available for infants to use the processor before they are eligible to have the implant and abutment placed. There are also plans to introduce a sound processor with directional microphones to improve hearing in noise.
Summary and Conclusion:
Missing an external ear may have functional and quality of life implications. Replacement of an ear may be by surgical means but is not always possible or satisfactory to the patient. Therefore, an ear prosthesis is an option. The use of osseointegrated implants improves the result that may be achieved in these cases.
In cases of specific conductive hearing losses, a bone conducting hearing aid retained by an osseointegrated implant may offer improved hearing over conventional aids.
This article described the application of osseointegrated implants for use with an ear prosthesis and a bone conducting hearing aid to improve the quality of life for these patients.
REFERENCES:
Figure 1. BAHA and ear prosthesis in place. NB. With long hair, BAHA is less noticeable. (Prosthesis by Susan Habakuk)
For more information about the BAHA system, click here.
