Approximately 3 out of 1000 children have unilateral hearing loss (UHL). Historically, audiologists have informed parents of children with UHL of the difficulties they would likely encounter localizing and listening in noisy situations.
However, parents were assured their child would develop speech and language normally, and that with preferential seating and perhaps the use of an FM system, they would probably do fine in school.
Studies by Bess et al (1984, 1986) revealed that children with UHL encounter more serious difficulties. They found that 35% had failed at least one grade as compared to 3.5% in their normal-hearing counterparts. Thirteen percent were in need of resource room help and 20% were described by their teachers as having behavioral problems. The results of this study were then corroborated by Oyler et al (1988).
Have the recommendations of audiologists changed with the knowledge of this information? Perhaps. With greater awareness of the possible problems encountered, there are more frequent recommendations for audiologic monitoring, FM system trials and speech-language evaluations. Some authors have recommended the use of a CROS hearing aid, but few have advocated the use of a hearing aid on the impaired ear.
Updike (1994) made comparisons among FM systems, CROS aids and personal amplification (a conventional hearing aid) in unilaterally hearing impaired children. The study looked at the speech recognition abilities of six children in quiet and in noise (+6 dB S/N). Results indicated little benefit from a CROS aid or a conventional hearing aid. Furthermore, they found there to be detrimental effects using these systems in noisy listening situations. As would be expected, speech recognition abilities improved in all listening situations with FM systems.
We often rely on the information obtained in the soundbooth to determine how a child will perform in the "real world". Though the results we obtain in the booth are valuable, they are not the final word. This is perhaps one of the reasons why outcomes measures are becoming such an important tool in our profession.
METHOD:
In 2000, the Audiology Department at the Children's Hospital of Philadelphia decided to become more proactive in fitting hearing aids to children with UHL, rather than fitting/recommending FM systems alone. This decision was due in part to the previously mentioned detrimental affects of UHL reported in the literature, as well as impressive results from a few children with UHL who had been fit at our center.
In 2001, our guidelines for audiologic management of children with UHL were changed to include hearing aid fitting. These guidelines included candidacy, testing procedures, fitting recommendations and counseling. To be considered a candidate for amplification, children should have hearing between 25 and 65 dB HL in the impaired ear and usable speech recognition in that ear. Decisions regarding children who fall outside of these criteria are left up to the professional judgement of the audiologist. Additionally, a loaner hearing aid bank was established to serve this population. Our goal is to fit the child with a loaner hearing aid on the second visit and provide a trial for three months.
As of March 2002, 28 children with unilateral hearing loss had been fit with a hearing aid on their impaired ear. Although we had documented test performance in the soundbooth, it was now our goal to determine how they performed outside of the confines of the soundbooth. Since some of these children were fit prior to the implementation of our guidelines (including outcomes measures), a survey was created to determine if different aspects of their every day life had been affected by the fitting of a hearing aid (see Figure 1). The parent was asked to score how his or her child is doing in specific areas now vs. prior to receiving the hearing aid. Some of the questions were modified from questions on the CHILD (Anderson & Smaldino, 2000). Ultimately, we wanted to know: Does this hearing aid improve their quality of life?
RESULTS:
Of the 28 children fit with hearing aids, 20 retrospective surveys were completed. Children's ages ranged from 2-17 years. Hearing loss in the impaired ear ranged from mild to moderately severe.
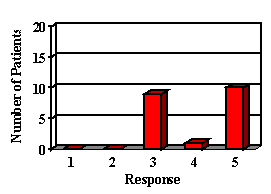
Most of the parents reported their child was either doing the same, improved or greatly improved in all areas (Figure 2). Most children showed improvements in areas in which auditory abilities were questioned. In areas in which confidence and frustration level were questioned, many remained the same, but most parents reported that confidence was not a problem prior to their hearing aid fitting. The majority of the children liked their hearing aid. Although some did not like the way it looked, they recognized that they were benefiting and chose to wear it. Although parents expressed that they were happy with their decision to get a hearing aid for their child, the majority wished they had done it sooner.
1. How has your child's attention span been affected since receiving his/her hearing aid? (RESPONSES Items 1-10 1: Greatly worsened. 2: Worsened. 3: Same. 4: Improved. 5: Greatly improved)
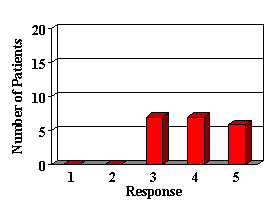
2. How is your child's ability to follow directions since receiving his/her hearing aid?
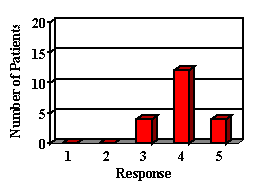
3. How is your child's general frustration level since receiving his/her hearing aid?
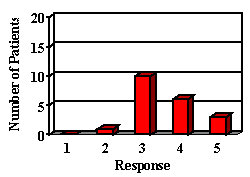
4. How is your child's ability to understand TV speech and conversations since receiving his/her hearing aid?
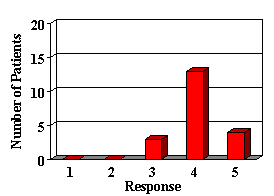
5. How is your child's response when called from another room since receiving his/her hearing aid?
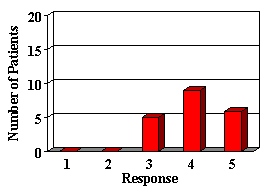
6. How is your child's ability to understand what is being said when playing or interacting in a group situation since receiving his/her hearing aid?
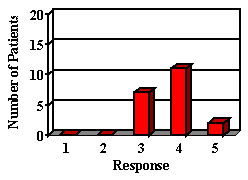
7. How is your child's ability to listen from the backseat of the car since receiving his/her hearing aid?
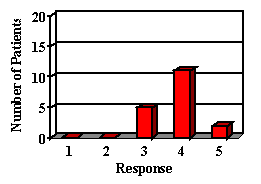
8. How is your child's ability to understand across a large room since receiving his/her hearing aid?
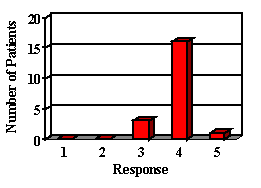
9. How is your child's confidence level since receiving his/her hearing aid?
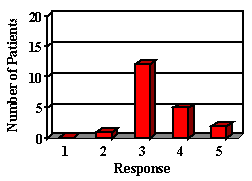
10. How is your child's general disposition since receiving his/her hearing aid?
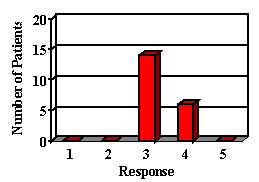
11. How does your child like his/her hearing aid? (RESPONSES 1: Hates it. 2: Does not like it. 3: Ambivalent. 4: Likes it. 5: Loves it.)
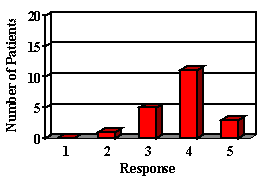
12. Based on your experience, how do you feel about your decision to get a hearing aid for your child? (RESPONSES 1: Wish you had not done it. 3: Glad you did it now 5: Wish you had done it sooner).
DISCUSSION:
All of the parents surveyed wanted to take the opportunity to make additional comments. Some comments are:
As can be seen, the parental comments support the overall findings of the survey. Parents reported that their children are hearing better, and consequently showing improvement in social and academic situations. Most noteworthy were the strong opinions expressed by parents who wished hearing aids had been recommended sooner. Many parents were passionate about this point.
Based on our findings, we believe that children with UHL (who fit candidacy requirements) should minimally receive a trial with amplification. Fitting these children has appeared to improve their quality of life. We believe that without this opportunity, the children are being denied access to their full potential.
REFERENCES:
Anderson KL, Smaldino JJ: CHILD: Children's Home Inventory for Listening Difficulties. 2000: www.edaud.org
Bess FH, Tharpe AM: Unilateral hearing impairment in children. Pediatrics 1984; 74: 206-216.
Bess FH, Tharpe AM: Case history data on unilaterally hearing- impaired children.
Ear Hear 1986; 7: 14-19.
Oyler RF, Oyler AL, Matkin ND: Unilateral hearing loss: Demographics and educational impact. Language Speech Hearing Serv Schools 1988; 19: 201-209.
Updike CD: Comparison of FM auditory trainers,CROS aids, and personal amplification in unilaterally hearing impaired children. J Am Acad Audio 1994; 5:204-209.
Appendix

Additional Comments:

