Assessment and Dialogue - Key Components in Successful Tinnitus Management
Carolyn Smaka: Welcome, Clement and Wendy. Audiology Systems and Otometrics have been recently spotlighting tinnitus management, which is a growing area of interest for audiologists. Tell me about this initiative.

Wendy Switalski: Yes, we just launched a series of activities to raise awareness about tinnitus, specifically for audiologists who are interested in adding tinnitus care to their practice. While there are methods for reducing the symptoms of tinnitus, there is in fact no cure-all for tinnitus today. This can make it difficult to know where to begin when a tinnitus patient walks in the audiologist’s clinic. We are excited to work with Otometrics to help our customers by creating awareness among hearing care professionals about the importance of assessment and dialogue in tinnitus management.

Clement Sanchez: Assessment and dialogue play a crucial role in managing tinnitus. With an assessment, the person with tinnitus can see it illustrated and quantified on an audiogram. The clinician can then use the tinnitus audiogram as a starting point for dialogue, determining the need for a hearing aid, masking sound generator, or both, and also as a base line for further assessments.
Carolyn Smaka: Let’s start at the beginning. Who are candidates for a tinnitus assessment?
Clement: Audiologists will ask about tinnitus in the case history as part of an audiological assessment. During these discussions, audiologists can determine if tinnitus is just a symptom that does not annoy the patient; or if it is creating concern and having a negative impact on the patient’s life.
For those patients in the latter group, a tinnitus assessment is in order. During the course of the, tinnitus assessment, questionnaires help to determine the severity of the impact that the tinnitus is having on the patient’s daily life. In looking at the impact, you can make a clinical decision whether dedicated tinnitus management is recommended.
Wendy: I agree with Clement. If you ask patients if they have tinnitus, many of them will say yes, as tinnitus and hearing loss often co-exist. As a quick delineator, we ask if it is bothersome tinnitus. Some people will respond by indicating, “I’m used to it and it doesn’t bother me.” It is important to note the symptom in the patient’s record, but when the tinnitus is bothersome or may be impacting quality of life, a formal assessment is indicated.
Carolyn: What are the components of a tinnitus assessment?
Clement: The tinnitus assessment consists of psychoacoustical measurements and the use of questionnaires to help quantify the impact of the tinnitus on the patient’s life.
The first part of a psychoacoustical assessment is pitch and loudness matching. We will translate the patient’s perceived pitch of the tinnitus into a frequency match, and we translate the perceived loudness of the tinnitus into a dB level. These components are very important because the results will enable you to document or map the patient’s tinnitus onto an audiogram. It is very powerful for the patient to actually see their tinnitus on an audiogram. It validates the fact that their tinnitus is a real, physical sound that they can share with their friends and family.
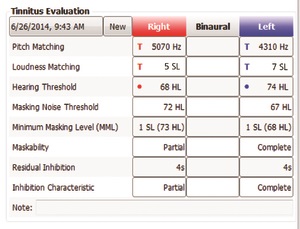
Another important component of the psychoacoustical assessment is masking the tinnitus. First, you want to determine what effect the presentation of an external sound will have on the tinnitus. Specifically, you want to find out the minimum amount of external sound that will have a positive masking effect on the tinnitus. These results will open the door to a management plan.
The next component is to measure the effect that occurs following the presentation of this external noise, what we call the rebound effect or residual inhibition. Residual inhibition refers to the temporary suppression of the tinnitus following masking. The presence of residual inhibition will provide some indication to the patient that the potential treatment will indeed provide a moment of calm or relief.
Carolyn: Practitioners have told me that documenting the pitch and loudness of the tinnitus alone helps relieve anxiety for many patients because you have validated their complaints in an objective way. Let’s move on to the questionnaires. What do they bring to the assessment?
 Wendy: As Clement mentioned, tinnitus questionnaires can help to quantify the impact of tinnitus on a patient’s daily life. The information can also be used to help make clinical decisions and to monitor a patient’s progress with treatment.
Wendy: As Clement mentioned, tinnitus questionnaires can help to quantify the impact of tinnitus on a patient’s daily life. The information can also be used to help make clinical decisions and to monitor a patient’s progress with treatment.
Commonly used questionnaires include the Tinnitus Handicap Inventory (THI) (Newman, Jacobson, & Spitzer, 1996), the Tinnitus Functional Index (TFI) (Meikle et al. 2012), and the Tinnitus and Hearing Survey (THS) (National Center for Rehabilitative Auditory Research).
The THI measures self-reported handicap and can be used to assess treatment outcomes. The TFI helps you to assess the severity of the tinnitus and define the negative impacts of the tinnitus. Both consist of 25 items and are easy to administer.
The THS helps to differentiate the challenges patients may be experiencing from tinnitus versus those they may be experiencing from hearing loss. Because hearing loss and tinnitus often co-exist, the THS provides guidance in sorting out the effects of each. These results can be helpful in the counseling process and in planning treatment. Patients often will lump their tinnitus and hearing challenges together. They may think they are not hearing well because of tinnitus, when in fact, they are not hearing well because of the hearing loss. The THS is not a validated measure so it should not be used as a primary outcome measure, but nonetheless the information it provides is beneficial and it can be a great supplement to other validated questionnaires.
Clement: I like the TFI because it’s easy to answer and scale, and it gives the professional a very fast and clear picture of how the patient is doing at a given point in treatment. It can be used to track progress over time, as it is quite robust in terms of consistency.
Carolyn: How does the MADSEN Astera2 support tinnitus assessment and management?
Clement: The MADSEN Astera2 from Otometrics is the only clinical audiometer with a dedicated tinnitus evaluation module. It has the psychoacoustical tests that we discussed, along with the tinnitus questionnaires, built in. And, the tinnitus evaluation module is very well integrated into the professional’s workflow. It guides you through the evaluation process.

The MADSEN Astera2 includes additional functionality including loudness scaling so that you can measure sound sensitivity for patients who also demonstrate that symptom. It also enables you to conduct Bekesy audiometry, which is not something new and fancy, but can be very useful for a tinnitus evaluation. For example, it is useful for patients who report that their tinnitus changes throughout the day – maybe sometimes it sounds like a low frequency buzz while other times it is a high frequency sound. With Bekesy audiometry, which is automatic, you can quickly and easily determine the pitch of their tinnitus and also get information on the patient’s sensitivity to sounds.
MADSEN Astera2 provides all these fundamental tools in an integrated and clear workflow for a complete tinnitus evaluation that is aligned with best practices.
Wendy: The clear layout of the MADSEN Astera2 tinnitus evaluation module makes the evaluation process very easy for professionals. For people that are new to tinnitus, it is a very approachable way to add tinnitus assessment to their practice. And, not only is the tinnitus module integrated into the Astera2, but the Astera works with the OTOsuite software. That means it is very easy to compare tinnitus assessment results and questionnaire results over time.
There is one other very important piece to the process - reimbursement. There is a CPT code for psychoacoustic evaluation, and the workflow in the tinnitus module ensures you have completed the necessary steps for documentation and reimbursement purposes. Lastly, it generates a tinnitus report for referral sources.
Carolyn: Clement, do you foresee Otometrics adding more tools and solutions to the tinnitus portfolio in the future?
Clement: Yes. The tinnitus assessment module in the MADSEN Astera2 has enabled us to combine the knowledge in the tinnitus literature with our technical capabilities in order to provide an excellent clinical tool for professionals. We have a lot of ideas for the future and will continue to innovate and support professionals in the tinnitus assessment and treatment process.
For more information and to access reference materials and available training, please visit www.audiologysystems.com/tinnitus or call (855) 283-7978. You are also invited to join the conversation and follow Audiology Systems on Facebook, Twitter and LinkedIn, and view the Otometrics / Audiology Systems Expo Page on AudiologyOnline.


