How Hearing Care Contributes to Holistic Health
AudiologyOnline: What do you mean when you say “holistic health”?

Sigurd Brandt: We tend to put things in boxes when we talk about health, for example “heart health”, but in reality no area of health is isolated. At GN Group, we develop solutions to manage hearing loss, but our customers might also be affected by other health issues when they are seeking hearing care. Hearing loss is well-known to be associated with other health-related issues and it is becoming clearer that we need to consider hearing loss beyond audibility; hearing loss can be thought of as being like the tip of an iceberg above the surface while there are many more related issues beneath with little visibility. So “holistic” refers to considering how these different issues interact and affect peoples’ overall functioning and well-being and consider these in the context of how the devices we make can help manage them. We believe that one of the most important areas to focus on is the link between cognitive health and hearing loss.
AudiologyOnline: Why is it especially important to consider cognition or even dementia in the context of hearing care?
Sigurd Brandt: Over more than a decade, studies have consistently shown a correlation between hearing loss and cognitive decline. The evidence built to the point where the Lancet commission in 2020 positioned hearing loss as the biggest potentially modifiable risk factor for dementia, which really catapulted the topic into the spotlight. The next logical question is that if a hearing loss might be contributing to your risk of dementia, could aiding your hearing alleviate the associated risk? Some studies have suggested that this could indeed be the case, but they have not met the methodological criteria that would allow us to make a definitive conclusion.
AudiologyOnline: The existing studies you mention point in the same direction and support treating hearing loss with amplification to slow cognitive decline. Why are they not enough?
Sigurd Brandt: Many of the studies were done on existing data sets, meaning that the researchers looked at data which was collected in a different context, but where there also was data on, for example, cognition, hearing loss and hearing aid use. Doing your study this way lets you see if different factors are correlated. But it limits the power to extrapolate the results to real world outcomes. We need to make sure not to overlook variables that also could have an effect.
AudiologyOnline: It sounds interesting to consider that a hearing aid can modify your risk of dementia. Can you expand on what you mean by overlooking variables?
Sigurd Brandt: Dementia is a multifactorial condition meaning many factors contribute to your risk, including hearing loss. On top of that, dementia is an umbrella covering various sub-types, Alzheimer’s being one of them. It’s a complex space. When I talk about overlooking variables it’s about trying to find groups that are as similar as possible and then you try to only change one of the known factors that can contribute to dementia. That way you can best understand what effect, if any, a factor such as treatment with hearing aids can have on your risk with high confidence that the effect is not caused by something else which you didn’t look for.
AudiologyOnline: If there are so many factors that contribute to dementia risk, is hearing loss then just a drop in the ocean, so to speak?
Sigurd Brandt: Hearing loss is considered to be the biggest potentially modifiable risk factor. A person’s risk of dementia is an individual risk profile with an individual threshold. Apart from hearing loss, the other 11 potentially modifiable risk factors identified by the Lancet commission include things like length of education, hypertension, diabetes, alcohol consumption, smoking, and physical activity level. Our behavior and habits or genetic predispositions create different starting points for our own risk. Thus, the sum of your total factors constitutes your risk of dementia and how close you are to the threshold. If you are not close to the threshold, lowering a risk factor may not have a noticeable effect. If you have a high risk, altering one or more of the risk factors can have a much bigger impact.
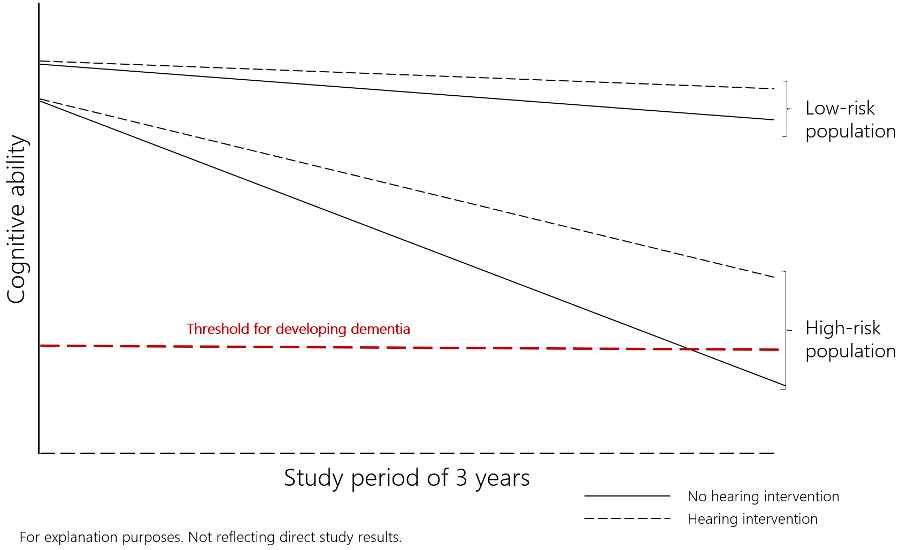
Figure 1. An example of how the trajectory of cognitive abilities might change over time depending on the individual’s level of risk factors. If an individual is at high-risk, using a hearing aid could make a big difference on how quickly cognitive decline might happen. If an individual is at low-risk, the hearing aids might still provide a reduced risk, but it might not be noticeable due to fewer risks overall.
AudiologyOnline: Are we sure there’s any real benefit to be found?
Sigurd Brandt: This was seen quite clearly in the ACHIEVE trial (Lin et al, 2023). This study followed two groups of people with hearing loss for three years: a high-risk group and a healthy control group. The investigators assessed changes to the study participants’ cognitive abilities when randomized to either using hearing aids or not using hearing aids. Across all participants no significant difference was seen between the ones who used hearing aids and the ones who didn’t. However, among the population of high-risk individuals they saw a significant 48% reduction in how fast the cognitive score declined over the three-year period in the group who used hearing aids compared to the ones who did not.
AudiologyOnline: What do you mean by a high-risk group in this study?
Sigurd Brandt: Firstly, high-risk means that the individuals had more chronic diseases such as heart disease and diabetes. Next, they were also older, had lower income levels, and shorter education which broadly speaking also predisposes the population to habits such as increased alcohol intake, smoking, etc. To my previous point, the sum of risk was greater than the general sum of risk in the healthy population. The power of the hearing aid intervention indicates that reducing one of the risk factors and thus the total sum of risk can have a big impact on your trajectory towards dementia. In this case it was by 48% for the high-risk group.
AudiologyOnline: Can you explain how you are looking at this topic in more practical terms?
Sigurd Brandt: First and foremost, we think raising awareness is key. Many within the audiological community are aware of the link, but at different levels. Furthermore, in a busy work life, you don’t always have time to stay up to date on all the research that comes out. As a result, finding ways to incorporate this knowledge into the daily workstream can be difficult. One of our objectives is to convey this information in a tangible, applicable and ethical way. At its core, we see this as a positive message. The more actions you can take to affect your future quality of life, the more you are empowered to live the life you want.
AudiologyOnline: You also mention devices earlier on. How do you see these changing in the light of the more holistic approach?
Sigurd Brandt: The way we create hearing solutions is centered around the natural ways we hear and use our hearing. Taking advantage of the synergies in what technology can do and what the brain can do ultimately have beneficial impact on the brain. This approach is in line with the leading hypotheses around why hearing loss could be associated with dementia. By creating devices that decrease our listening effort through incredibly advanced beam forming technologies and improved speech in noise performance, we can support the natural way the brain processes sound with the least amount of effort. That is Organic Hearing. We will continue down this path and long-term we believe the technology will play a greater role in general health through targeted health monitoring capabilities. Hearing aid users will get insights that they can act on to maintain good health and communicate with health care providers.
AudiologyOnline: A greater role in health monitoring capabilities. Can you be a little more concrete?
Sigurd Brandt: Health monitoring in hearing aids means to be able to use sensors to collect objective data about your health. Sensors can be microphones, accelerometers, heartbeat monitors or anything that picks up data. The data collected by sensors can help you to understand when you should talk to your health care provider and what you should say. And it means being able to help the health care provider make more informed individualized decisions on your treatment, because they can use the data to understand exactly what you might need. These prospects are unprecedented and make for an exciting future in healthcare.
References
Lin, F. R., Pike, J. R., Albert, M. S., Arnold, M., Burgard, S., Chisolm, T., ... & Coresh, J. (2023). Hearing intervention versus health education control to reduce cognitive decline in older adults with hearing loss in the USA (ACHIEVE): a multicentre, randomised controlled trial. The Lancet, 402(10404), 786-797.


