Interview with Dr. J. Thomas Roland, Jr., Director of Otology and Neurotology, Co-director of the New York University Cochlear Implant Center
Paul Dybala: This is Dr. Paul Dybala with Audiology Online. Today I have Dr. J. Thomas Roland from the Cochlear Implant Center at New York University. Dr. Roland, thank you for talking with me today. Could you start by telling us a little bit about yourself and your professional background?
J. Thomas Roland: I am currently the Director of Otology and Neurotology and the Co-Director of the Cochlear Implant Center at New York University. I wear several hats. First, I am responsible for the otologic education of our residents, and I run a fellowship in Neurotology. We take a fellow every other year, and because it is an ACGME approved fellowship, the fellow is eligible to sit for the Certificate of Added Qualification with the Neurotology Boards.
I also practice clinically. I have a very busy and active practice, with a very busy cochlear implant practice. I have personally implanted over 1000 cochlear implants, and we complete somewhere between 140 and 170 cochlear implants a year at NYU. I am also very involved in skull base surgery and acoustic neuroma surgery, and I have performed approximately 40 auditory brainstem implants, which I think makes us the second busiest center in this country for ABIs.
NYU Cochlear Implant Center
I spend a lot of my research time working with and understanding cochlear implant related issues and cochlear implant electrode design in particular. I have worked with engineers from different companies over the last 15 years on various aspects of the surgical feasibility and the function of cochlear implants and cochlear implant electrodes.
Dybala: You definitely stay busy. As we are talking about cochlear implantation and electrode insertion, can you tell us the typical issues associated with standard straight or lateral wall electrode insertions?
Roland: Yes. Historically, during a cochlear implant operation we make a hole in the basal turn of the cochlea, or what we call a cochleostomy. I think we used to make it in the wrong place, but we are getting better and better at putting it in the right place. This is in part due to our understanding of what is necessary to preserve residual hearing during cochlear implantation. The idea is to get the electrode to go into the lower scala, the scala tympani and be as atraumatic as possible.
A straight electrode is basically an outer wall electrode. When you push something straight into a circle it wants to re-obtain its straight configuration, and therefore, it occupies the outer wall of the cochlea. Usually, these electrodes sit up under the spiral ligament, where the basilar membrane attaches, and have often been documented to disrupt, break, or injure the basilar membrane. The geometric nature of the scala tympani is such that the outer wall has an upward slope;therefore, any force that you push against that wall will result in reactive forces pushing the electrode upwards superiorly through the upper scala structures.
Depending on some of the physical characteristics of the electrode (i.e., how flexible it is, how soft it is, how delicate it is), the degree of trauma will change;however, in general, straight electrodes occupy the outer wall of the cochlea and cause trauma to the outer wall.
There are some issues related to the stimulation characteristics as well, because when stimulating from the outer wall, larger fields of stimulation are created and specificity of neuronal subpopulation stimulations may be reduced. If the stimulus is generated near the spiral ganglion cells, lower thresholds are required and perhaps more specific neuronal subpopulation stimulus occurs. That is all somewhat dependent on the stimulation mode and the electrical characteristics of the electrode.
Dybala: Very good. Now, you have been involved with various research projects that focus on the Contour Advance electrode and the Advance Off-Stylet (AOS) technique. Can you tell us how this is different from standard techniques?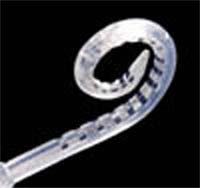
Contour Advance Electrode
Roland: The standard technique is where you basically push a straight electrode into the cochlea through the cochleostomy. With the Contour electrode, which is the predecessor to the Contour Advance, you push the electrode in and then pull a stylet, and then it would coil once it is already fully inserted. The idea with the Contour Advance was to create a technique and electrode that would reduce intracochlear outer wall contact and trauma even more. In essence, it is a curl-as-you-go type of electrode. It coils as it is advanced off a stylet.
The concept is to insert the electrode until the white marker on the electrode which is about 11 contacts from the tip, is at the cochleostomy. At this point the electrode tip is just contacting the posterior wall of the cochlea (the back wall of the pars ascendens). Then, holding the stylet steady the electrode is advanced sliding it off the stylet. It curls to a perimodiolar position as it goes in the cochlea. This significantly reduces the amount of contact, the amount of friction, and the amount of force on that posterior outer wall. This was well documented in several studies.
If intracochlear trauma occurs, it is almost always at the point of contact with the posterior outer wall. This is where too much force can result in electrodes going up through the basilar membrane and into the other scala. The Contour Advance basically avoids that contact, pressure, and force in that area to hopefully prevent those types of injuries to the cochlea.
Dybala: There was a study published in Laryngoscope in 2005 where you used the AOS technique on cadavers to evaluate this technique. Can you tell us what this study showed?
Roland: In that study, we looked at a number of things to help the electrode design engineers and those people interested in electrodes evaluate their electrode performance. We watched the procedures on real-time fluoroscopy to evaluate performance. We cut the bones and looked histologically for any evidence of intracochlear trauma or injury and we also measured forces, mechanical and hydraulic.
We were able to use a device, an Instron machine, that would insert the electrode at a constant rate. We then measured, with a force measuring device, the amount of pressure applied to the back wall of the cochlea. I have done this technique with other electrodes, but on this particular study we looked at the difference between the Contour and the Contour Advance.
In the study, the Contour was inserted as an outer wall electrode, then the stylet was pulled, and the electrode moved to the medial wall;however, there still was a fair amount of outer wall contact. We compared the forces generated with that technique to those that were generated with the Advance Off-Stylet technique, and we found very significant and striking results. Using the Advance Off-Stylet technique with a Contour Advance electrode resulted in minimal- to no- forces applied to the back wall of the cochlea. Therefore, the implication would be that there would be less trauma, less force, and less damage to the basilar membrane and the upper scalar structures with the Advance Off-Stylet technique.
We also showed that there were no significant hydraulic forces generated. We could measure those forces from a catheter in the superior semicircular canal ampulla. We also showed fluoroscopically and histologically that this reduced force did indeed result in a nice perimodiolar positioning, and in the five bones that we studied carefully, there was no significant intracochlear trauma.
As a corollary to that, we also looked at x-rays on patients that have been implanted with both of these electrodes. With the standard Contour electrode and that insertion technique, about one third of the x-rays showed that we probably penetrated the basilar membrane and it had at least partial scala vestibuli insertions.
When we looked at another cohort of patients using the Contour Advance electrode with the Advance Off-Stylet technique, we found only about 4% of cases where we might have traversed the scala and had scala vestibuli positioning in at least some of the electrodes. This put our studies into the clinical realm, and it showed a nicer, more reliable, more consistent insertion with less risk of trauma.
Dybala: Sure, and if there is less trauma to the cochlea then some of the residual hearing can be preserved. Could you tell us about studies to this effect?
Roland: I know of a large European study as well as some anecdotal reports and studies in America using the standard Contour Advance electrode with the AOS technique and saving a significant amount of hearing. By making the cochleostomy properly and in the right position and using a careful Advance Off-Stylet technique, clinicians were able to preserve hearing in a significant number of patients.
There are also some more recent studies that suggest a correlation between the electrode placement and the resultant performance with these electrodes. In a study in Germany and also in a study out of St. Louis, CAT scans were performed posteratively, and those patients that had pure scala tympani insertions (with fewer electrodes in scala vestibuli) seemed to have better speech perception scores. There was a direct correlation between the number of electrodes in the scala vestibuli and a lower speech perception score.
Dybala: Great. For my final question, could you discuss the findings of the study conducted at the University of North Carolina that was published in Laryngoscope in 2007?
Roland: Of course. This study was the result of a questionnaire that was distributed out by the House Cochlear Implant Study Group, which meets once a year at the Academy meetings. This is a group of cochlear implant surgeons and professionals. They unite to cover pertinent cochlear implant issues, and the group has grown quite significantly over the years.
The questionnaire was handed out to about 73 members of this group, and I think 55 or so responded. It asked a number of questions, such as, "Where would you place your cochleostomy?" It had a grid showing various cochleostomy placement points and the respondent had to pick a number on that grid.
It also asked, "Do you routinely identify the facial nerve during the facial recess? Do you routinely identify the chorda tympani nerve? Do you drill off part of the round window? What is your final cochleostomy size? Do you sometimes do round window insertions?" The questionnaire also asked a little bit about professional experience;for example, "How many cochlear implants do you do a year? What kind of a drill do you use for the cochleostomy? What size burr do you use?"
What they discovered was that there is still a large variability in the techniques used, and there is a lack of uniformity, even among experienced surgeons, of where they place the cochleostomy and the technique used.
My personal feeling, having studied electrodes for 15 years and looking at and cutting temporal bones (for example, we just cut seven bones this weekend) is that a very low inferior cochleostomy is the way to go. If you want to stay away from the basilar membrane, reduce intra-cochlear trauma, and get the correct trajectory to initiate your cochlear implant insertion, the cochleostomy should be directly inferior to the round window. The surgeon should approach the cochlea from inferiorly. We leave the endosteum intact until the very last minute and then open the endosteum delicately and insert the electrode with the right trajectory down the basal turn of the cochlea.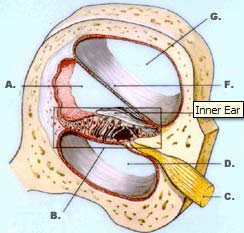

Anatomy of the Inner Ear
The basic take-home message from this study is that there is still a large amount of variation in the field. I think that is very interesting and pertinent, because I think we stopped focusing on cochleostomy position and techniques. More recently, this concept is of prime interest among surgeons, especially because studies are showing electrode placement may have implications for performance.
In addition, consistent perimodiolar positioning may have implications for being able to use some of the new programming and processing capabilities of these devices;therefore, it would be very nice to know that every single implant is in a great perimodiolar position with appropriate electrode placement.
There are a number of potential implications to having precise electrode placement. If one were programming bilateral implants, it would be nice to know that electrode three on one side correlates with electrode three on the other side to help with aspects such as pitch matching.
Dybala: Great point. I think that concludes the questions I have today. For more information on the work that Dr. Roland and his team do at NYU Cochlear Implant Center, visit www.med.nyu.edu/cochlear/, and for access to a variety of interviews, news articles, and live e-seminars on cochlear implants, search cochlear implants on Audiology Online at www.audiologyonline.com. Dr. Roland, thank you very much for providing this insight today.
Roland: You are welcome.
More information on NYU Cochlear Implant Center
The NYU Cochlear Implant Center originated in 1984, and since that time, they have provided sound to thousands of children and adults of all ages through cochlear and auditory brainstem implantation. The Cochlear Implant Center at NYU has served as a pioneer in the field of implantation, being the first to implant several new prostheses and being a part of several clinical studies. In addition to clinical services, the NYU Cochlear Implant Center is also heavily involved in research to further the development of implantation in the future.

