Introduction
Varying degrees of cerumen occlusion pose challenges in the delivery of diagnostic or rehabilitative services. Routine audiological procedures require the presence of a relatively clear external auditory canal. Although the degree to which the external auditory canal must be free of cerumen depends on the specific procedure, at some point, most audiologists will find themselves in a situation where cerumen removal is necessary for the provision of clinical services. There are several different ways to remove cerumen from the external auditory canal including mechanical removal, suction, and irrigation. The purpose of this article is to review a few fundamentals of mechanical cerumen removal.
Mechanical Removal of Cerumen
Mechanical removal of cerumen involves the use of hand-held instruments. This cerumen removal technique offers several advantages over suction and irrigation. First, mechanical removal requires the least amount of financial investment for equipment. Second, hand held instruments used for mechanical removal are portable whereas the heavier suction pumps or irrigation equipment is bulkier, posing challenges in terms of ease of portability. Finally, mechanical removal is probably the most patient-friendly in that is represents the least intimidating technique and does not require the use of suction device that may be loud or rely on introducing irrigation into the ear canal.
As with any cerumen removal technique, an appropriate light source is needed to properly illuminate the external auditory canal for inspection of the cerumen accumulation. There are a variety of light sources to choose from including something as simple as a pocket light with wire loop tips to a more expensive headlamp show in Figure 1. The deeper the impaction, the more critical of a role magnification plays. Unless cerumen resides at the opening of the external auditory canal, an appropriate light source with magnification is necessary for cerumen management procedures. For example, an operating head otoscope with or without a nasal speculum effectively provides both illumination and magnification while allowing the audiologist to readily pass instrumentation through the otoscope and into the external auditory canal. Unlike an otoscope, headlamps offer the advantage of hands-free illumination, making it easier for the audiologist to properly brace the patient's head and manipulate instrumentation. Not all headlamps provide magnification; for cerumen management purposes, a headlamp with magnification is most appropriate.
Figure 1. Welch Allyn Lumniview Headlamp with magnification.
Instrumentation
There are a variety of hand-held instruments that may be used including curettes, loops, hooks, and forceps. These hand-held instruments are typically comprised of steel, although disposable instruments are also available in plastic. Not all steel or instrument craftsmanship is of the same quality (Kemp & Bankaitis, 2005a). The highest quality steel instruments are made of German stainless steel, crafted in Germany. These instruments will cost significantly more than other stainless steel and economy-grade instruments. Economy-grade instruments represent the most inexpensive instruments; however, these non-stainless steel instruments are more susceptible to corrosion. It is not uncommon for economy-grade instruments to require replacement over a relatively short period of time (Kemp & Bankaitis, 2005a).
At first glance, it may seem that all instrumentation serves the same purpose. There happen to be a wide variety of curettes, loops, hooks and forceps. Curettes, loops, and hooks look very similar; however, each instrument has a unique tip. In contrast, forceps resemble either a small pair of scissors or a pair of tweezers. The intent of the following section is to review a few of the more commonly-used instruments.
Buck Curette:
The Buck curette (Figure 2a) is a metal rod with a tip that resembles an "O" (Figure 2b). This instrument is available in a variety of sizes as determined by the size of the tip's lumen. Sizes range from 00 to 4, with higher-size numbers corresponding to larger lumen sizes. The lumen for a size 00 Buck curette is two millimeters with each whole number curette, starting with size 1, increasing in lumen size by an additional one millimeter. In addition, the orientation of the lumen relative to the rod may be angled or straight. An angled Buck curette orients to a 45º angle, whereas a straight Buck curette orients to 0° and is not angled at all. For cerumen removal, it is recommended to integrate angled Buck curettes.
Figure 2a. Buck curette.
Note. Reprinted with permission by Auban, Inc.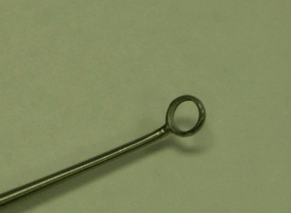
Figure 2b. Detailed view of the tip of the Buck curette.
Note. Reprinted with permission by Auban, Inc.
Billeau Ear Loop:
The Billeau ear loop (Figure 3) is a metal rod with a small wire loop at the end. The Billeau ear loop is available in small, medium, or large sizes. The small Billeau ear loop is approximately the same size as a size 0 Buck curette, whereas the large Billeau ear loop is approximately the same size as a size 4 Buck curette. This instrument is also available in a disposable form, although only in one size.
Figure 3. Detailed view of the tip of the Billeau ear loop.
Note. Reprinted with permission by Auban, Inc.
Disposable Instruments:
A wide range of disposable instruments are also available for cerumen removal. Comprised of plastic, these instruments are intended for one-time use only. Since several different manufacturers produce these instruments, a variety of sizes and types are available. Many disposable curettes are plastic versions of the Buck curette or the Billeau ear loop. Other disposable instruments resemble spoons that come in small, medium, and large sizes.
Alligator Forceps:
Alligator forceps resemble a pair of scissors (Figure 4a). Unlike the wide range in which standard scissor blades may be extended, the blades of the Alligator forceps offer a smaller range of extension, opening and closing only at the very tip of the forceps (Figure 4b).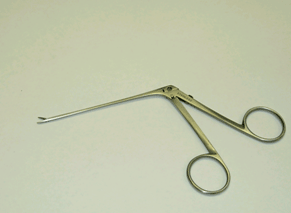
Figure 4a. Alligator forceps.
Note. Reprinted with permission by Auban, Inc.
Figure 4b. Up-close view of Alligator forceps.
Note. Reprinted with permission by Auban, Inc.
Application of Mechanical Instruments
Which mechanical instrument to use during cerumen removal procedures remains mostly a matter of preference on the part of the audiologist. As described by Bankaitis, Kelso, and Kemp (2005), there are instances where certain factors may dictate the use of one instrument type over another. In general, three main factors will influence instrument choice including
- thickness of the instrument's tip,
- degree of cerumen impaction,
- consistency of cerumen.
Thickness of instrument's tip:
When considering curettes and loops, both mechanical instruments maintain unique tip configurations comprised of varying degrees of thickness. For example, the Buck curette has a much more substantial tip as compared to the thinner wire of the Billeau loop. Due to the differences in tip thickness, the Buck curette is much more effective in scooping cerumen out of the ear canal, particularly when the cerumen is paste-like. In contrast, the flexibility of the Billeau loop's tip is ineffective in scooping copious amounts of cerumen from the external auditory canal. On the other hand, since the tip is much thinner than the Buck curette, the Billeau loop offers very little resistance to cerumen and is extremely effective in breaking through a thin section of a cerumen plug. Note that in certain circumstances it will be most effective to initiate cerumen removal with a Billeau loop and only then switch to a Buck curette.
Degree of cerumen impaction:
The degree of cerumen impaction will influence which instrument should be used during the initial stages of mechanical removal. In general, the greater the degree of cerumen impaction (ear occlusion), the smaller the surface area should be of the instrument tip. For instance, in the presence of a partial occlusion where the tympanic membrane is visible, the use of a Buck curette would most likely be effective since the impaction is incomplete and provides a wide enough gap for instrument positioning. In contrast, in the presence of a complete occlusion, initially using an instrument with a smaller surface area, such as a Billeau loop, can assist in breaking through the weakest part of the occlusion while minimizing the potential of moving the cerumen plug further back into the external auditory canal. Once a large enough hole is created within the cerumen plug, switching to a Buck curette would be appropriate.
Consistency of Cerumen:
The consistency of cerumen will, to some degree, influence instrument choice. Cerumen that is relatively moist yet pasty will be more readily removed with a Buck curette than a Billeau loop or forceps. Cerumen that is very dry or consists of a group of loose particles will be more readily removed with forceps since these instruments are designed to grab cerumen. Use of forceps in this case allows the clinician to pull dry cerumen out with less effort than it would take to sweep or scoop particles out with a Buck curette. In situations where the consistency of the cerumen is neither too moist nor too dry, depending on the degree of occlusion, it may be beneficial to initially use a Billeau loop, or Buck curette. Using forceps when cerumen is too moist will result in a labor intensive process since the moistness of the cerumen will not allow the forceps to effectively grab a significant portion.
Cerumen Removal Technique:
When using curettes or loops, the standard technique for removing cerumen involves placement of the instrument's tip at the superior aspect of the occlusion. Since cerumen typically accumulates in a bottom-up fashion, the superior aspect of a cerumen plug tends to be thinner. Thinner sections represent the weakest portion of the cerumen plug, offering the path of least resistance for mechanical instruments. Once a workable hole has been created (or already exists), the next step is to position the tip of the instrument just behind or as close to the back of the cerumen plug as possible and slowly move the instrument down and toward the opening of the ear canal, gently pulling the cerumen out. The top-down approach in removing cerumen is often the most comfortable for the patient as pressure on the anterior and posterior canal wall is avoided during removal procedures, minimizing the potential for triggering Arnold's (cough) reflex.
When using forceps, the occlusion is approached with blades (tip) closed and in a manner such that contact by the forceps will not push the cerumen plug further back in the ear canal. This technique requires positioning the forceps at the edge of the occlusion, close to where the ear canal is unoccluded. Once the impaction is approached, the forceps may be opened and then used to gently grab the occlusion and slowly move it toward the opening of the external auditory canal, making sure no portion of the cerumen is adhering to the canal wall.
Cerumen Softening Agents
Cerumen softening agents are over-the-counter solutions designed to soften cerumen. Technically, cerumen softening agents are not cerumenolytics since these agents do not chemically break down cerumen. Rather, these products soften cerumen. The active ingredient for most cerumen softening agents is 6.5% carbamide peroxide. Cerumen softening agents may be purchased from a variety of distributors and typically come packaged in one of two ways:
- ½ oz bottle of softening solution, or
- as part of an over-the-counter earwax removal system.
The earwax removal system includes the ½ oz bottle of softening solution packaged with a soft-bulb ear syringe. The earwax removal systems are designed to soften and loosen cerumen for easier removal, preferably by an audiologist, physician, or other qualified health professional.
When to Use Cerumen Softening Agents
Cerumen removal does not necessarily require the use of cerumen softening agents. The use of a cerumen softening agent is most helpful when:
- the ear canal is completely occluded with cerumen and the consistency of the cerumen is very hard or dry, or
- when the ear canal is partially occluded with cerumen and a portion of the wax is attached to the epithelial layer of the ear canal skin (Bankaitis, Kelso & Kemp, 2005)
In cases of complete occlusion with very hard or dry cerumen, the integrity of the tympanic membrane cannot be assessed. In these cases where the impacted cerumen does not make complete contact with the wall of the external auditory canal along the entire perimeter, the use of cerumenolytic agents is not recommended. Even in cases of extremely hard or dry cerumen, if there are gaps along the outer circumference of the impacted cerumen, it is possible for some of the cerumen softening agent to seep beyond the cerumen plug. Since the integrity of the tympanic membrane is unknown, it is not a good idea to proceed with this type of procedure. The best course of action is to refer the patient for cerumen removal. In cases where the impacted cerumen does make complete contact with the wall of the external auditory canal along the entire perimeter along its circumference, cerumen softening agents may be used by the patient for up to approximately four days for the purpose of the patient returning to the clinic so that the cerumen removal process may be more manageable.
Cerumen softening agents are also effective in situations when the ear canal is partially occluded with cerumen and a portion of the wax is attached to the epithelial layer of the ear canal skin. One of the advantages of a partial occlusion is that audiologists will be able to assess the integrity of the tympanic membrane most of the time. In the event the tympanic membrane is intact, softening agents should be used to weaken or soften the attachment between the cerumen and the epithelial layer of the canal wall skin. Although this may slightly delay cerumen removal for 20 to 30 minutes, the application will minimize the potential of tearing the canal skin, causing bleeding and trauma. Even subtle trauma to the sensitive canal skin wall can significantly increase the risk of skin redness, irritation, and/or infection.
It is not recommended to use cerumen softening agents in situations where the cerumen is mainly of a soft or moist consistency. Using softening products when cerumen is already moist will change its consistency to a more viscous or liquid form. This will actually make it more difficult to remove cerumen with instrumentation. The removal of runnier cerumen will be labor intensive and not necessarily the best use of clinical time, particularly if the situation can be avoided in the first place.
Lastly, it is not advisable for audiologists to get in the practice of using products such as stool softeners or home remedies such as olive, castor, or mineral oil as cerumenolytic agents. The scope of practice for physicians is significantly more lenient in terms of prescribing or using non-FDA approved items in clinical practice. While physicians may use home remedies, from a legal perspective, audiologists should not assume the same freedoms as physicians. The application of products whose intended use is not specified as appropriate for hearing health care (i.e. stool softener) or products falling under the category of home remedies (olive, castor, or mineral oils) leaves too much room for interpretation in the event of an adverse event resulting from cerumen removal. Particularly for home remedies, it is uncertain as to the conditions in which these non-FDA approved products have been prepared. Ethically, it is the responsibility of the audiologist to only use FDA-approved agents for safe and effective cerumen removal procedures.
Infection Control and Cerumen Management
Infection control refers to the conscious management of the environment for the purposes of minimizing or eliminating the potential spread of disease (Bankaitis & Kemp, 2003; 2004). It is a critical component to cerumen removal for several reasons. First, cerumen is considered potentially infectious when it is contaminated with blood, dried blood, mucous, or ear discharge. Since it is highly probable for cerumen to be contaminated with these bodily substances it should be treated as a bodily fluid. Second, the external auditory canal remains more prone to bacterial infection than other skin surfaces (Jahn & Hawke, 1992). Inserting contaminated instruments into a patient's ear canal provides microbes an easy portal of entry into the body, which may potentially result in disease, particularly in immunocompromised patient populations. Third, cerumen removal is associated with potential risk of ear canal laceration that poses not only a risk for blood exposure to the clinician, but poses a risk for serious, life-threatening infection to the patient. Finally, infection control in the health care setting is a federally-mandated program. Failure of compliance results in citations and significant fines.
The Occupational Safety and Health Administration (OSHA) requires health care facilities to generate and have available a written infection control plan. The specific infection control requirements are beyond the scope of this chapter; however, related resources are currently available for audiologists and dispensing professionals (Bankaitis & Kemp, 2003; 2005). To facilitate the process of implementing infection control procedures during cerumen management, the remainder of this article will provide some basic fundamentals applicable to cerumen removal procedures.
Procedures for Reusing Mechanical Instruments
Cerumen removal via mechanical procedures involves extraction through the use of both reusable and disposable instruments. Disposable instruments are considered a one-time-use, one-time-only instrument and are not intended for reuse. In contrast, metal instruments intended for reuse must be treated very specifically prior to reuse since these instruments are considered critical instruments. Critical instruments are those instruments or objects introduced directly into the bloodstream, an otherwise sterile area of the body, or non-invasive instruments that come in contact with intact mucous membranes or bodily substances (blood, saliva, mucous discharge, pus). According to this definition, any reusable item used during mechanical removal of cerumen, including curettes, loops, and forceps, must be cleaned and then sterilized.
Cleaning refers to procedures in which gross contamination is removed from surfaces or objects without killing germs (Bankaitis & Kemp, 2003, 2005). It is an important prerequisite for sterilization and must occur prior to sterilization as the effectiveness of these procedures may be compromised without it (Kemp & Bankaitis, 2000). In contrast, sterilization involves killing 100% of vegetative microorganisms, including associated endospores. When microbes are challenged, they revert to the more resistant life form called a spore (Bankaitis & Kemp, 2003; 2005). Sterilants, by definition, must neutralize and destroy spores because if the spore is not killed, it may become vegetative again and cause disease. Whereas disinfection may kill some germs, sterilization, by definition, kills all germs and associated endospores each and every time.
There are two general sterilization techniques:
- the autoclave and
- cold sterilization techniques.
The autoclave involves pressurized heat for sterilization. Most audiologists do not have access to autoclaves and must rely on cold sterilization. Cold sterilization involves soaking instruments in EPA-approved liquid chemicals for a specified number of hours. Glutaraldehyde solutions in concentrations of 2% or hydrogen peroxide (H202) in concentrations of 7.5% or higher are the only chemicals approved by the EPA for cold sterilization (Bankaitis & Kemp, 2003; 2005).
Other Infection Control Considerations
Since cerumen management exposes the audiologist to cerumen and potentially other bodily substances, appropriate protective barriers in the form of gloves, masks, and disposable gowns should be used to ensure federal infection control requirements are met. In addition, hand washing likely represents the single most effective means of minimizing the spread of disease. Audiologists must wash hands before contact with every new patient and immediately after the removal of gloves. Furthermore, hands must be washed at any other time that clinical circumstances require. Finally, it is important for audiologists to have a plan should accidents occur. In the event a patient's ear is accidentally nicked, it is critical for audiologist to have sterilized gauze or cotton tip applicators and other items readily accessible to assist in stopping bleeding with an appropriate patient follow-up plan to confirm proper healing, including a referral resource.
Conclusion
Cerumen management is an important component to the provision of audiological services. There are several different procedures to removing cerumen including mechanical removal. Mechanical removal of cerumen using hand-held instruments is a relatively straightforward procedure requiring knowledge in a wide range of areas including ear canal anatomy, instrumentation, removal technique, and infection control principles. It involves the use of curettes, loops, and/or forceps. When necessary, cerumen softening agents are integrated to facilitate removal procedures. Although relatively straightforward, it is a procedure that requires experience and skill beyond what has been covered or implied in this article.
References
Bankaitis, A.U., Kelso, S., & Kemp, R.J. (2005). Cerumen removal technique. In A.U. Bankaitis and S. Kelso (Eds.), Cerumen Management (pp. 71-84). St. Louis: Auban, Inc.
Bankaitis, A.U., & Kemp, R.J. (2003). Infection Control in the Hearing Aid Clinic. Boulder: Auban Inc.
Bankaitis, A.U., & Kemp, R.J. (2005). Infection Control in the Audiology Clinic, 2nd Edition. Boulder: Auban, Inc.
Jahn, A.F., & Hawke, M. (1992). Infections of the external ear. In C. Cummings, J.F. Fredrickson, L. Harker, C. Krause, & C. Schuller (Eds.), Otolaryngology - Head and Neck Surgery, (2nd ed.) (pp. 2787-2794). St. Louis: Mosby - Year Book.
Kemp, R.J., & Bankaitis, A.E. (2000). Infection control for audiologists. In H. Hosford-Dunn, R. Roeser, & M. Valente (Eds.), Audiology Diagnosis, Treatment, and Practice Management, (Vol. 3.) (pp. 257-279). New York: Thieme Publishing Group.
Kemp, R.J., & Bankaitis, A.U. (2005a). Cerumen removal instrumentation and equipment. In A.U. Bankaitis & S. Kelso (Eds.), Cerumen Management (pp. 57-70). St. Louis: Auban, Inc.


