The way in which audiology is practiced is changing. In the past, it was often adequate to base clinical decisions on intuition and data collected in laboratories rather than the real world. Today, a new paradigm based on evidence-based practice and sound clinical research is emerging. Evidence-based practice (EBP) is the process by which audiologists make patient treatment decisions based on a careful study of the clinical evidence (Cox, 2004; 2005). An evidence-based approach suggests that the audiologist carefully analyze the research and incorporate the findings into their clinical practice if the evidence is strong enough.
Recently, there has been interest in the use of evidence-based principles as they relate to the practice of hearing aid dispensing. In 2004, a special two-day workshop sponsored by the Independent Hearing Aid Fitting Forum (IHAFF) in Jackson Hole, Wyoming was held. The entire IHAFF workshop was devoted to a review of the evidence related to various aspects of the hearing aid fitting process; subsequently, several papers presented at the workshop were published in the 2005 July/August edition of the Journal of the Academy of Audiology (JAAA). The IHAFF workshop and the JAAA journal edition challenged many of the scientific bases underlying contemporary practice in the hearing care profession and revealed several of the limitations of how hearing aids are currently dispensed. While many topics were covered in this publication, there was no conclusive review of evidence either supporting or not supporting the use of speech audiometry as either a pre-fitting or post-fitting predictor of hearing aid benefit.
Speech Audiometry
Assessment of speech perception has been, and remains, a routine part of clinical audiometry. The diagnostic value of identifying and differentiating auditory disorders is well documented; furthermore, speech audiometry has been recognized as an important component of the diagnostic test battery for well over 75 years (Fletcher, 1929). Speech audiometry has been used since the 1940s as part of the hearing aid selection and fitting process (Carhart, 1946). Numerous measures of speech intelligibility, including word recognition, sentence length, and speech-in-noise tests, have all been employed as part of both the pre-fitting selection and hearing aid fitting verification protocols. Some speech audiometry procedures have enjoyed widespread use for decades and have become an accepted part of the clinical repertoire for the dispensing audiologist.
Given this history, it is not surprising that speech audiometry for the purpose of fitting hearing aids is popular among audiologists. Kirkwood (2005) reported that 92% of audiologists surveyed used some type of speech audiometry procedure. Strom (2003) reported that 42% of dispensing professionals use some type of speech-in-noise testing during the pre-fitting test battery. Aided speech audiometry has also enjoyed widespread clinical use over the years. According to two separate studies by Mueller (2003) and Lindley (2006), 30% of audiologists routinely conduct aided speech measures, with over 70% of this group using either the W-22 or NU-6 for verification purposes at the time of the fitting.
While popularity of a test procedure does not equate to efficacy, it is reasonable to assume based on surveys that most audiologists believe speech intelligibility testing is a valuable component of the hearing aid selection and fitting protocol. However, given the current trend to develop protocols that are evidence-based, it is critical that these popular clinical procedures accurately predict benefit in real-world listening situations.
Hearing aid benefit can be defined as the difference between unaided and aided performance measured either objectively or subjectively. Hearing aid benefit can be measured objectively by comparing aided and unaided measures of speech recognition ability, as one example. Hearing aid benefit can also be measured subjectively through the use of self-report measures. Because objective tests are completed using a pre-defined external standard, they are taking place almost exclusively within the laboratory. Therefore, self-report measures of outcome are a useful method of determining real-world benefits of hearing aid performance.
Another separate dimension of outcome is hearing aid satisfaction. Satisfaction differs from benefit in that satisfaction is not necessarily performance driven. For example, a patient can experience a significant degree of benefit as measured on aided and unaided tests, but be reporting dissatisfaction as measured on a satisfaction scale.
An important question to address at this time is, "why do we need self-report measures of real-world outcome?" According to Cox (2003) there are at least three reasons to use self-report measures of benefit and satisfaction. First, for largely economic reasons, health care is becoming more consumer driven. In this evolving system, the consumer decides what treatment is selected and when it is complete. The major index of quality of service is self-report outcome and satisfaction. Consumer-driven health care places an added emphasis on the patient's point of view. Therefore, it is critical to measure the real-world benefit and satisfaction of hearing aid use.
A second reason self-report measures of outcome are gaining importance is related to the fact that many of these real-world experiences simply cannot be measured effectively in laboratory conditions. The traditional hearing aid outcome measures clinicians have used in the past, such as speech recognition in quiet and in noise, do not capture the true experiences of hearing aid use in everyday listening situations. In order to quantify the true impact hearing loss and its associated treatment have on activity limitations, lifestyles, etc., self-report measures outcome can be used.
Third, even when laboratory conditions are used to simulate real-world listening situations, they do not always resemble the patient's impression of the actual real-life situation. According to Cox (2003), self-report outcome measures are increasing in use, because they give us a scientifically defensible way to validly measure the real-life success of the hearing aid fitting.
In an attempt to evaluate the predictive value of speech intelligibility scores on self-report measures of hearing aid benefit, this review will examine the evidence supporting and opposing the use of speech intelligibility tests in the hearing aid selection and fitting process. This review focused on two clinically relevant questions related to speech audiometry as a predictor of hearing aid benefit: 1) Are there real-world outcome measures from adult patients to support the use of speech audiometry as a pre-fitting selection tool?; and, 2) Are there real-world outcome measures from adult patients to support the use of speech audiometry as a post-fitting verification tool?
Evidence-Based Systematic Review and Methods
Using the five steps of EBP and six levels of evidence outlined by Cox (2005), the author reviewed evidence published in peer-reviewed journals over the past 25 years in an attempt to answer the two aforementioned clinically-based questions. In order for the evaluation of the evidence to be considered clinically effective, studies were included for review only if they met the following criteria:
- Published in a peer-reviewed journal between 1980 and 2005
- Used a research design in which only randomized, controlled studies and meta-analysis of high quality studies (Level 1 and Level 2 evidence), and non-randomized intervention studies (Level 3 evidence) (Cox, 2004; 2005).
- Used adult subjects with hearing impairments
- Completed self-report measures of real-world hearing aid outcome during the post-fitting follow-up process.
- Conducted speech intelligibility testing either as part of a pre-fitting test battery or post-fitting hearing aid verification protocol.
The decision to use these criteria was not arbitrary. Self-report measures of real-world outcome were not commonly employed in research until the 1980s. It was also determined that adults would be the focus of this review, as the data for children are considerably different than for adults.
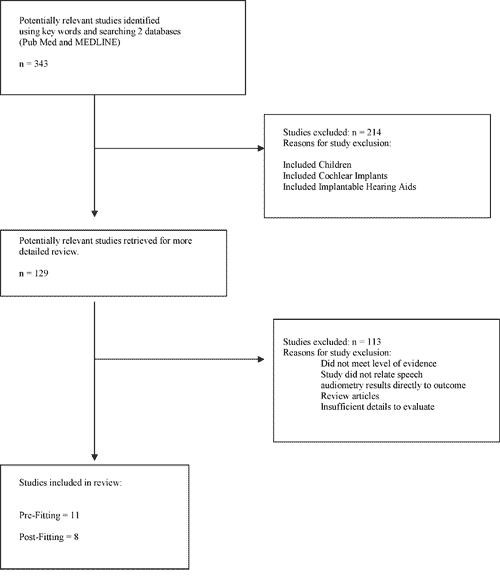
Figure 1. Summary of flow of study selection and inclusion/exclusion
(See page 5 of addendum for detail)
Results
Two separate reviews were conducted, one for the use of speech audiometry as a pre-fitting measure of intelligibility, and a separate review for speech testing used as part of an aided assessment during the fitting. The decision to conduct two separate reviews was based upon consideration of the fact that surveys show clear differences as to when speech testing is conducted by audiologists (Mueller, 2003).
Pre-Fitting Speech Audiometry
A total of 11 studies met the above criteria and were reviewed (A list of the reviewed studies including summary information for each is provided on page 1 & 2 of the PDF addendum to this article - DOWNLOAD PDF ADDENDUM). Out of the 11 studies, 10 used some type of speech-in-noise testing in their design; the other used speech testing in quiet conditions only. None of the 11 studies showed a strong predictive relationship between pre-fitting speech test scores and self-reports of hearing aid outcome. Four studies indicated a statistically significant, but weak correlation between pre-fitting test scores and hearing aid outcome. A good example of this comes from the Humes and Humes (2004) analysis of 123 adults two years post-fitting. In their regression analysis, they show a weak correlation between the amount of decline in speech-recognition performance at high intensities (PI-PB rollover) and the classification of individuals as successful or unsuccessful hearing aid users as classified by the Hearing Aid Interview. Additionally, other speech tests used in the analysis (Connected Speech Test and Nonsense Syllable Test, each completed in quiet and in noise) were not able to differentiate successful and unsuccessful hearing aid users.
The other study of note is the one conducted by Walden and Walden (2004) in which unaided QuickSIN scores were compared to scores obtained on the International Outcome Inventory for Hearing Aids (IOI-HA), Satisfaction with Amplification in Daily Life (SADL), and Hearing Aid Usefulness Scale (HAUS). In this non-randomized study of 50 adults, the unaided QuickSIN score and all measures of outcome were correlated. However, this predictive relationship is attributable to aging effects. Walden and Walden (2004) also used the NU-6 in quiet as another unaided test. There was no predictive relationship between the NU-6 and any measure of hearing aid outcome used in this study. Additionally, once the effects of aging are taken into consideration, there is no predictive relationship between unaided QuickSIN scores and hearing aid outcome.
This review indicates that there is no evidence supporting the pre-fitting use of single word speech tests in quiet. There is weak evidence at best to support the use of sentence-length speech-in-noise testing presented at multiple intensity levels during the pre-fitting assessment as predictors of hearing aid outcome as measured on a self-report scale.
Post-Fitting Speech Audiometry
A total of 8 studies in which aided speech testing was compared to hearing aid outcomes were reviewed (A list of the reviewed studies including summary information for each is provided on page 3 & 4 of the PDF addendum to this article - DOWNLOAD PDF ADDENDUM). Out of the 8 studies, 5 cited here were also reviewed in the unaided review. The predictive nature of these five studies was consistent for both unaided and aided comparisons to hearing aid outcome: If the unaided test showed no relationship to hearing aid outcome, the aided version of the test was not different. As with the unaided QuickSIN, Walden and Walden (2004) showed a predictive relationship between the aided QuickSIN results and self-report measures of hearing aid outcome. However, this predictive relationship is dependant upon age. In other words, a patient's age is just as likely to predict hearing aid outcome as his or hers QuickSIN score.The final study worth noting was a meta-analysis conducted by Gatehouse (1998) consisting of a large sample size (n
Discussion
The purpose of this review was to investigate the predictive value of speech intelligibility testing as currently practiced by most audiologists. There are two important questions in need of discussion. The first relates to the use of speech audiometry during the pre-fitting test battery. The second is related to the role aided word recognition performance contributes to capturing overall hearing aid benefit.
Unaided Speech Intelligibility as a Predictor of Hearing Aid Benefit
In an era in which self-report assessment of real-world outcomes is gaining importance, the way clinicians conduct speech audiometry for the purposes of hearing aid selection and verification needs to be reevaluated. A single pre-selected presentation condition (e.g., single words in quiet) does not reflect the range of listening conditions that the typical patient experiences on a daily basis. To that end, there is no evidence suggesting that any single combination of speech material, presentation level, or signal-to-noise ratio used during the pre-fitting assessment predicts outcome with hearing aids in everyday listening situations.
Humes et al. (2003) examined three groups of hearing aid patients: Group 1 purchased and retained their hearing aids; Group 2 returned their hearing aids for credit; and Group 3 did not purchase hearing aids. All three groups were matched for hearing loss, age, and gender. Unaided speech scores showed no significant differences for the three groups. If hearing aids returned for credit is assumed to be a measure of dissatisfaction, this provides further evidence of no relationship between unaided speech intelligibility scores and self-reports of satisfaction and benefit.
As hypothesized by Carhart and Tillman (1970) over 35 years ago, "the patient's performance in these noisy situations gives the clinician perhaps the most realistic index of the performance that the hearing aid user can expect to achieve in a good portion of his daily life." Recognizing this, several sentence length speech-in-noise tests have become commercially available over the past decades, although up to this point they have failed to gain widespread clinical use (Mueller, 2003). Even in studies using these sentence length speech-in-noise tests, there was a weak relationship between pre-fitting speech intelligibility scores and self-reports of real world hearing aid benefit.
Aided Speech Intelligibility Testing as a Predictor of Hearing Aid Outcome
There are several reasons aided tests of speech intelligibility are conducted clinically. One of the major reasons is to determine if hearing aids provide benefit. When used as a measure of benefit, aided scores are compared to unaided scores, and differences are observed. Although comparing aided speech intelligibility to unaided speech intelligibility continues to be a popular hearing aid verification test, there is virtually no evidence to support its continued use as a predictor of self-report measures of real-world hearing aid outcome.
Although the evidence does not support the use of aided speech intelligibility as a predictor of hearing aid benefit, there are some studies worthy of further discussion. Humes (2003) and Gatehouse (1998) in their meta-analyses examined the relationship between various measures of both unaided and aided word recognition performance and self-report of hearing aid outcome. Both meta-analyses used a large sample size and wide array of target stimuli, signal-to-noise ratios, and presentation levels.
Gatehouse (1998) noted that when conducting a composite Four Alternative Auditory Feature (FAAF), which samples at two different presentation levels and two separate signal-to-noise ratios, almost one-quarter of the variance in the outcome measure can be accounted for use of the composite FAAF realtive to the FAAF presented in four completely separate presentation levels. These findings suggest that a wider sampling of the patient's typical listening environments increases the overall effectiveness of the laboratory test as it relates to patient's everyday listening situations.
Humes (2003) reported a meta-analysis of three large studies, each with a large sample size. Four unaided and four aided measures of speech intelligibility were correlated with each other. Additionally, five measures of subjective benefit, two measures of satisfaction and three measures of usage, were all correlated with each other. However, no predictive relationship across these measures was found. Humes (2003) concluded that there are three separate and distinct measures of hearing aid outcome which all can be measured clinically:
- Usage;
- Subjective satisfaction and benefit; and,
- Speech intelligibility performance.
The preponderance of studies reviewed here suggest that speech intelligibility tests, conducted either unaided or aided, are not good predictors of hearing aid benefit for everyday listening situations as measured on self-report scales of hearing aid outcome. Even though speech audiometry is considered to be an essential part of the basic hearing aid evaluation protocol, as well as a standard part of the post-hearing aid fitting follow-up, there is limited evidence to support its use as a predictor of real-world hearing aid outcome. What little evidence there is to support the use of speech audiometry comes in the form of sentence-type-speech-in-noise tests. A weak, positive relationship appears to exist between speech-in-noise testing, particularly when presented at more than one level, and real-world outcome.
There are some clinical procedures using recorded speech and noise, which hold promise as pre-fitting predictors of real-world hearing aid benefit. The Acceptable Noise Level Test (ANLT), developed by Anna Nabelek (2003) and colleagues at the University of Tennessee, has been shown to be a strong predictor of hearing aid use, when unaided ANLT scores are collected during the pre-fitting appointment (Nabelek, Tampas, & Burchfeld, 2004). In a recent study, unaided ANLT scores predicted a patient's success with hearing aids with 85% accuracy (Nabelek et al., 2006).
Another speech test conducted during the pre-fitting appointment that appears to be a relatively good predictor of real-world aided benefit and satisfaction is the Performance-Perceptual Test (PPT). (Saunders & Forsline, 2006). The PPT uses a format wherein the patient subjectively rates their ability to understand speech in noise, and compares this subjective rating to the objective score on a sentence-length speech in noise test (e.g. QuickSIN). Emerging evidence suggests that the PPT might be good predictor of hearing aid satisfaction.
Based on review of the evidence, and in view of the emerging patient trends outlined by Cox (2003), the following recommendations would be supported by Level 1 to Level 3 evidence:
- During the pre-fitting evaluation, audiologists are advised not to rely on unaided speech intelligibility scores in the hearing aid selection process when making judgments or predictions on real-world outcome.
- Aided speech intelligibility tests utilizing single words in quiet have no predictive relationship to self-report measures of hearing aid outcome. Aided speech intelligibility testing using sentences in noise presented at multiple intensity levels has a minimal predictive relationship, at best. There is simply not enough evidence to support the use of aided speech intelligibility tests in determining if hearing aids are providing real-world benefit.
Acknowledgements
The author wishes to acknowledge Gus Mueller, Patti McCarthy and Mike Nerbonne for their valuable comments and suggestions on this paper. Significant portions of this paper were originally part of a Central Michigan University capstone.
References
Bentler, R., Anderson, C., Niebuhr, D., & Getta, J. (1993). Longitudinal study of hearing aid effectiveness I: Objective measure. Journal of Speech and Hearing Research, 6(4), 808-819.
Carhart, R. (1946). Selection of hearing aids. Archives of Otolaryngology. 44, 1-18.
Carhart, R. & Tillman, T. (1970). Interaction of competing speech signals with hearing loss. Archives of Otolaryngology, 91(3), 273-79.
Cord, M., Leek, M., & Walden, B. (2000). Speech recognition ability in noise and its relationship to perceived hearing aid benefit. Journal of the American Academy of Audiology, 11(8), 475-483.
Cox, R. (2003). Assessment of subjective outcome of hearing aid fitting: getting the client's point of view. International Journal of Audiology, 42, S90-S96.
Cox, R. (2004). Waiting for evidence-based practice for your hearing aid fittings? It's here. The Hearing Journal, 57(8) 10-17.
Cox, R. (2005). Evidence-based practice as a provision of amplification. Journal of the American Academy of Audiology, 16(7), 419-438.
Crowley, H., & Nabelak, A. (1996). Estimation of client-assessed hearing aid performance based upon unaided variables. Journal of Speech and Hearing Research, 39(1),19-27.
Davis, H. & Silverman, R. (1947). Hearing and Deafness. New York: Holt, Rinehart and Winston.
Etymotic Research. (1993). The SIN Test. (Compact Disc). 61 Martin Lane, Elk Grove Village, IL 60007.
Fletcher, H. (1929). Speech and Hearing. New York: Van Nostrand.
Gatehouse, S. (1994). Components and determinants of hearing aid benefit. Ear and Hearing, 15(1), 30-49.
Gatehouse, S. (1998). Speech tests as measures of outcome. Scandinavian Audiology Supplement,.27(49S), 54-60.
Humes, L., Wilson, D., and Humes, A. (2003). Examination of differences between successful and unsuccessful elderly hearing aid candidates matched for age, hearing loss, and gender. International Journal of Audiology, 42(7), 432-441.
Humes, L., & Humes, L. (2004). Factors affecting long-term hearing aid success. Seminars in Hearing, 25(1), 63-72.
Kirkwood, D. (2005). When it comes to hearing aids, "more" was the story on '04. The Hearing Journal, 58(5), 28-37.
Lindley, G. (2006). Current hearing aid fitting protocols: results from an online survey. Audiology Today, 18(3), 19-22.
Mueller, H.G. (2003). Fitting test protocols are "more honored in the breach than the observance". The Hearing Journal, 56(10), 19-26.
Mulrow, C., Tuley, M., & Aguilar, C. (1992). Correlates of successful hearing aid use in older adults. Ear and Hearing, 13, 108-113.
Nabelek, A., Burchfeld, S., & Webster, J. (2003). Relationship between acceptance of background noise and hearing aid use. Journal of the Acoustical Society of America, 11, 2289.
Nabelek, A., Freyaldenhoven, M., Tampas, J., Burchfield, S., & Muenchen, R. (2006). Acceptable Noise Level as a predictor of hearing aid use. Journal of the American Academy of Audiology, 17, 626-639.
Nabelek, A., Tampas, J., & Burchfield, S. (2004). Comparison of speech perception in background noise with acceptance of background noise in aided and unaided conditions. Journal of Speech, Language, and Hearing Research, 47, 1001-1011.
Parving, A. (1991). The value of speech audiometry in hearing-aid rehabilitation. Scandinavian Audiology, 20(3), 159-164.
Strom, K. (2003). The HR 2003 dispensing survey. The Hearing Review, 16(6), 22-38. Saunders, G. & Forsline, A. (2006). The Performance-Perceptual Test (PPT) and its relationship to aided reported handicap and hearing aid satisfaction. Ear and Hearing, 27, 3, 229-242.
Tillman, T. & Carhart, R. (1966) An expanded test for speech discrimination utilizing CNC monosyllabic words (NU-6). Tech Rep SAM-T, June, 1-12.
Walden, B., Schwartz, D., Williams, D., Holum-Hardegen, L., & Crowley, J. (1983). Test of the assumptions underlying comparative hearing aid evaluations. Journal of Speech and Hearing Disorders, 48(3), 264-273.
Walden, B., Surr, R., Cord, M., Edwards, B., & Olson, L. (2000). Comparison of benefits provided by different hearing aid technologies. Journal of the American Academy of Audiology, 11(10), 540-560.
Walden, T., & Walden, B. (2004). Predicting success with hearing aids in everyday living. Journal of the American Academy of Audiology, 15(5), 342-352.


