With the increased number of hospitals performing universal newborn hearing screenings, audiologists will be increasingly responsible for the early identification and diagnosis of hearing loss. Importantly, we will be increasingly called upon to fit hearing aids on a patient population under the age of 6 months. Early identification of hearing loss and accurate fitting of hearing aids has a significant benefit on language development (Eilers, 1994). Therefore, audiologists must provide the best amplification and fitting possible. The latest programmable and digital technology makes accurate fittings easier, especially for the higher frequencies (2000-6000 Hz). At Children's Healthcare of Atlanta, we have developed a protocol for tone burst evoked potential testing to ensure we have the information necessary for a thorough hearing aid fitting on these young patients.
The search for an accurate way to evaluate the hearing of young children began in the early 1940's by the Ewings of England (Northern, 1991). Ewing and Ewing observed physical reactions to sounds such as eyeblinking, involuntary squinting, jumping, and sound localization. During the same time period, Froeschels and Beebe described the cochleopalpebral reflex (Northern, 1991). Also called the auropalpebral reflex, this involuntary shutting of the eyes with acoustic stimuli occurs at approximately 24 - 25 weeks gestation age in fetuses developing normally (Kuczwara, 1984). The limitations of these observable reflexes were obvious and the search continued for a reliable objective test measure. Acoustic immittance showed promise; however, Keith (1973, 1975), found that only one third of healthy newborns exhibited a clear stapedial reflex. His findings suggested that immittance testing could not be used as a sole assessment of hearing. Keith was not the only one evaluating objective techniques to evaluate infant hearing in the 1970's. The Crib-O-Gram devices and Auditory Brainstem Response (ABR) tests were also being explored (Hall, 1992). Of all these methods, the ABR has become the most widely utilized.
When testing infants, evoked potentials are an essential portion of the audiologic evaluation. However, testing limited to traditional ABR click stimuli provides an estimation of auditory functioning in a broad frequency range between 1000-4000 Hz. A complete evoked potential evaluation must contain reliable ear specific and frequency specific information. According to Hall (1992), a brief tone stimulation is the obvious choice for frequency specific ABR.
TONE BURST PROTOCOL
Establishing a protocol, which is adequate for all clinical situations is impossible. Clinics may vary their protocol based on available equipment, time and information needed. The flow chart below outlines our typical protocol:
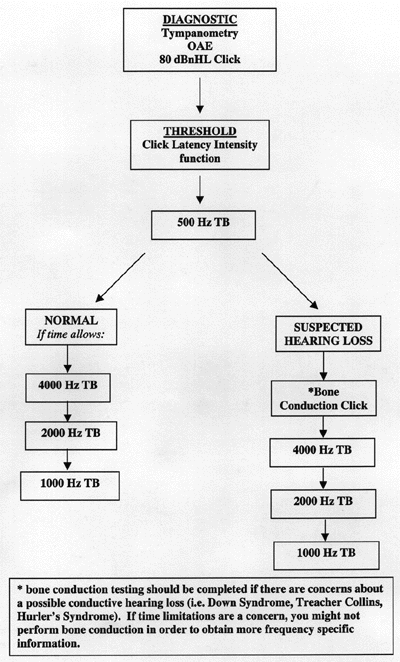
Prior to three months of age, a natural sleep state is attempted. In our clinic, children three months and older are sedated by a nurse for the evoked potential testing. With the type of sedation typically used at our facility (chloral hydrate), the majority of sedated children sleep for approximately one hour. We have found this is enough time to obtain click stimulus and 500 Hz tone burst evoked responses. If the child continues to sleep, more threshold information may be obtained. Preparedness is the key to obtaining the most information in the shortest period of time. Before the child falls asleep, skin can be prepared for electrode placement; however, some clinicians prefer to wait until after the child is asleep so as not to interfere with the sedation process. Additional preparation involves readying the electrodes and insert earphones, securing extra electrodes in case replacements are needed, ensuring the amplifier cord and earphone cords are not touching each other and completing the set-up of the patient file on the evoked potential system.
PARAMETERS:
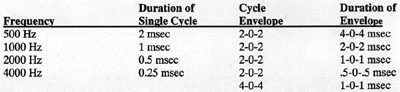
Polarity: Rarefaction or condensation may be used. However, an alternating click stimulus may be necessary to reduce electrical interference commonly observed in hospitals.
Stimulus rate: 27.7/sec or 39.1/sec. Our clinic uses 39.1/sec.
Ramping/Windowing: Blackman. Many systems use linear ramping. However, this conventional form of ramping produces non-frequency specific ABRs due to spectral splattering into areas of the cochlear with better hearing, especially with tone bursts below 1000 Hz. Therefore, frequency specific results with linear envelopes are not valid, particularly in the low frequencies (Hall, 1992). To ensure validity on frequency specific studies, Blackman ramping should be utilized.
Electrode placement: Cz-A1 and Cz-A2
Filter Settings: High Pass 30 Hz. Since tone burst ABR typically has a great deal of low frequency energy, it is essential to have the high-pass cut off set at 30 Hz.
Low Pass 1500 Hz - 3000 Hz
Intensity: Variable
IMPORTANCE OF TONE BURST CALIBRATION
The dial reading on most new ABR equipment does not come from the manufacture set up in dB nHL (dB normal hearing level). Appropriate correction factors are critical for accurate estimation of thresholds based on tone burst evoked potential responses. Using normal hearing adults is the easiest way to start gathering normative data to establish correction factors. The number of adults used to establish norms might vary but should be at least 10.
To initiate a Tone Burst calibration protocol, we recommend:
1- Test adults in the sound booth with insert earphones 500-4000 Hz and obtain behavioral auditory thresholds in dB HL.
2- Perform behavioral hearing test via the ABR equipment. Thresholds should be obtained for each tone burst stimulus in a sound treated room (Hall, 1998). Behavioral thresholds obtained on the ABR equipment are important because periodic listening checks can be performed to verify normal operation; just like verifying normal output from the clinical audiometer.
3- Record the ABR and obtain wave V thresholds and latencies. With this information, develop a correlation factor between the dial setting on the ABR equipment and auditory thresholds obtained in the booth. When completing a test, subtract the correlation factor from the ABR dial setting to obtain the corrected threshold in dB nHL.
RELIABILITY OF THE TONE BURST COMPARED TO BEHAVIORAL THRESHOLDS
A high correlation between tone burst thresholds and behavioral thresholds has been demonstrated within 20 dB by numerous authors (Hall, 1992). Stapells (1998) studied the correlation between tone burst ABR thresholds and behavioral thresholds in infants and young children. He found that 98% are within 30 dB, 80% are within 15 dB, and 66% are within 10 dB. Folsom (1996) demonstrated that thresholds for low-frequency tone burst evoked responses tend to be 10 dB poorer than behavioral thresholds. The average difference between behavioral and ABR thresholds for mid-to-high frequencies is less than 10 dB. The author cautioned that + 2 standard deviations of calculated threshold differences can create differences of up to 48 dB in the low frequencies and 30 dB in the mid-to-high frequencies. Gorga (1988) demonstrated that thresholds for tone burst evoked responses may vary slightly among subjects. His study compared the thresholds of four different subjects and found that Wave V threshold varied by up to 10 dB for 500 Hz and 2000 Hz tone burst stimuli. These authors remind us that evoked potentials are a test of auditory functioning and not an exact threshold for hearing. Behavioral testing should always be conducted when the child is developmentally appropriate.
WHAT THE TONE BURST TELLS US
We all know that evoked potentials are not a test of hearing. However, the neural responses obtained from the tone burst provide us with valuable information and should be considered a starting point of estimating behavioral thresholds. The threshold information can be used to help further educate parents regarding their child's hearing loss and its possible configuration. In addition, the estimated thresholds are beneficial for programming hearing aids and verifying the fitting using hearing aid fitting formulas such as DSL. The thorough audiologist will continue attempts to obtain ear specific and frequency specific behavioral thresholds. Once the child is able to perform Visual Response Audiometry (VRA) an ear specific audiogram should be obtained. For best results, use foam insert eartips or the child's earmolds by attaching the insert nipple into the earmold tubing.
CONCLUSION
Although conducting tone burst evoked potentials involves additional preparation and test time, the information obtained and the application of the additional information is extremely valuable. Incorporating tone burst evoked potentials into our evoked potential protocol has been an excellent and simple way to gather more information using equipment we already owned and had at our disposal. In retrospect, now we wonder how we ever fit a hearing aid without it!
REFERENCES
Eilers, R, Kimbrough, O.: Infant Vocalizations and the Early Diagnosis of Severe Hearing Impairment. J of Pediatr124:199-203.
Folsom, R: Frequency Specific ABR. Fourth International Symposium on Childhood Deafness. 1996
Gorga MP, Kaminski JR, Beauchaine KA, Jesteadt, W: Auditory Brainstem Responses to Tone Bursts in Normally Hearing Subjects. Journal of Speech and Hearing Research 31: 87-97, 1988.
Hall, J: Handbook of Auditory Evoked Responses. Boston. Allyn and Bacon, 1992.
Keith R: Impedance Audiometry with Neonates. Arch Otolaryngol 97: 465-467, 1973.
Keith, R: Middle Ear Function in Neonates. Arch Otolarngol 101:376-379, 1975..
Kuczwara LA, Birnholz JC, Klodd DA: Auditory Responsiveness in the Fetus. Natl. Student Speech Lang Hear Assoc J 14:12-20, 1984.
Northern J, Downs, M: Hearing in Children, 4th ed. Baltimore: Williams & Wilkins, 1991.
Stapells, D: Frequency Specific Evoked Potential Audiometry in Infants. Phonak: A Sound Foundation Through Early Amplification; Oct 1998

