Interview with Sam Marzo, M.D., Neurotologist, Department of Otolaryngology, Loyola University Medical Center
Beck: Good Morning Dr. Marzo. Thanks for sharing your time with me today.
Marzo: Hi Dr. Beck. Nice to speak with you again.
Beck: Dr. Marzo, would you please tell me a little about your professional education and experience?
Marzo: Sure. I graduated from Loyola University Medical School in 1991, and did my otolaryngology residency at Loyola and finished in 1996. I did my fellowship in otology, neurotology and skull-base surgery in Nashville, with Drs. Michael Glasscock and Gary Jackson. After my fellowship, I had a private practice and I was part-time faculty at Loyola. Then in 1999, I became full-time at Loyola and have been here ever since.
Beck: I suppose your practice at Loyola is 100 percent otology and neurotology and skull-base surgery?
Marzo: Yes, that's right...and then I have areas of interest for research and that includes hearing loss, facial nerve disorders, dizziness and related topics.
Beck: Excellent. I wonder if you can tell me a little about the direct bone conduction system, and its application to hearing loss patients?
Marzo: Sure. There have been a few other implanted bone conduction systems available over the last few years; these systems were originally designed for people with middle ear damage, such as those with severe irreparable damage from cholesteatoma or middle ear infections, or for people with birth defects in whom the middle or outer ear was not fully developed. So originally, we thought of these systems as potential solutions for people with maximal conductive hearing loss and other conductive hearing losses.
Beck: And indeed, that is still the case....but now, direct bone conduction has also been shown to be advantageous in cases of Single Sided Deafness, or SSD.
Marzo: Right. That's the more recent application, and it's opened up options for people with total and permanent hearing loss in either ear, secondary to trauma, or perhaps after the surgical removal of a skull base tumor, such as people who've lost hearing due to acoustic neuroma.
Beck: OK, let's chat a little about children with atresia (the absence of an ear canal) and in particular, children who have been radiologically shown to have normal inner ears - are they candidates?
Marzo: Assuming the child has bilateral atresia and normal inner ears, they are likely a candidate....However, one issue would be the age of the child. The FDA approval currently only goes down to age five years for implantation of the bone conduction system. Nonetheless, if
the child is very young bone conduction can be achieved using a headstrap. This brings up a few issues. Adults that tried the strap tell us that although it's pretty good, it is not as good as the implanted device. Therefore, if we offer this alternative to very young children, we allow them to have access to speech and language, which is obviously very important, but we're not doing so optimally. So if the child is physically well developed, and the surgeon decides a child aged three or four years is a good candidate, they can implant the device in appropriate candidates. We have a slide that shows how bone conduction sound bypasses the outer ear, the ear canal and the middle ear, stimulating the inner ear, the cochlea directly.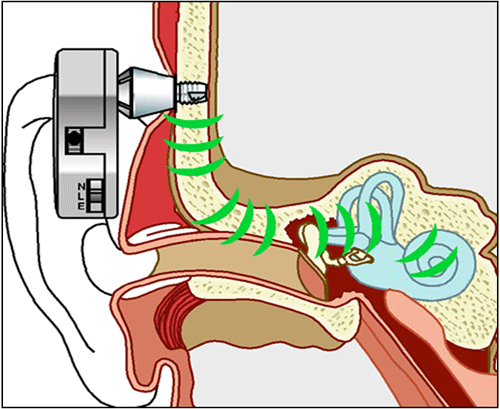
Beck: We know that for appropriate children, implanting a cochlear implant down to age 12 months is very important...and we know that the earlier a child is implanted, the better their chance of developing normal speech and language, and getting mainstreamed in school....so the same assumptions can be made here? On other words, earlier implantation is better?
Marzo: Yes, and I think this is a very reasonable assumption.
Beck: I agree. If it were my child, I would certainly argue that the sooner the child receives effective speech and language input, the better the opportunity for success. If the child was implanted at say, age three years six months, would you eventually repair the atresia?
Marzo: Yes. When the child is ready, atresia repair is still an option, one does not exclude the other. Atresia repair may be done at approximately age five, or a little older...but atresia repair and direct bone conduction are not at all mutually exclusive. Some children with atresia have stenotic ear canals and they're at greater risk for cholesteatoma...so that's another reason to do atresia repair, even for a child doing very well with the implant.
Beck: Very good. Let's talk a little about SSD patients.
Marzo: I see quite a few of these patients. They may be post-op acoustic neuroma patients, trauma patients or sudden sensorineural hearing loss patients - those that didn't respond to steroid or other medical/surgical treatments.
Beck: I'd like to mention that sudden sensorineural hearing loss is considered a medical emergency, and people experiencing this need to see an otologist or a neurotologist immediately because if it's treated immediately, some of these cases will reverse.
Marzo: That's correct. I appreciate your mentioning that. Many docs don't treat sudden sensorineural hearing loss aggressively, they just watch and wait. However, we know that a significant number can be helped with aggressive and immediate medical therapy.
Beck: Can you review how the direct bone conduction system works for patients with SSD?
Marzo: The direct bone conduction system is surgically placed on the side without hearing, just above and behind the ear. When the sound processor unit "hears" a sound on the bad side, it sends out a bone-conducted signal, which the normal cochlea hears. The system allows the patient to perceive sounds from both sides of their head, within the better ear. Some patients say they can even tell where the sound is coming from while using the system for SSD. I have a slide on this too, showing an example in which the left ear isn't working, and so the system is placed on the left side, and the sound is transmitted to the right side.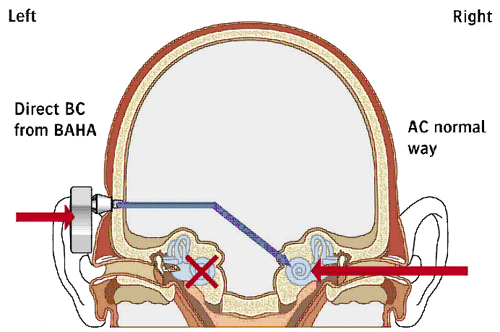
Beck: And this is an important benefit because people cannot localize very well with only one hearing ear. In other words, their ability to tell where the sound is coming from is pretty much non-existent with untreated SSD, and that can be dangerous with respect to horns honking, sirens approaching, tires screeching, finding a ringing phone, determining who is calling them or speaking, or hearing other warning sounds.
Marzo: Right. Of course, we're not sure why they can tell the direction of the sound with SSD using the direct bone conduction system...but we've heard this time and time again, and I believe many of them can.
Beck: Yes, I've had direct bone conduction patients tell me that too. I think it has to do with the quality of the sound, and perhaps a consciously imperceptible temporal lag...I wonder if the brain can tell the difference in the sound quality from the normal ear, versus the bone conducted sound, and after adaptation has occurred, perhaps a month or two or three, maybe the patient's brain automatically recognizes qualitative and quantitative differences? Perhaps the arrival time at the cochlea of the two auditory inputs, allows the brain to unconsciously fill in the missing pieces to create a localization percept?
Marzo: That makes sense. But as of this moment all we know with certainty is that patients do report localization ability.
Beck: Sounds like a wonderful premise for localization-based research!
Marzo: I agree. We've been very pleased to offer this alternative to our patients, and we've had excellent results.
Beck: Is the direct bone conduction system covered by most insurance companies?
Marzo: Well, that's always a great question. Generally it is covered, but every insurance company and every insurance policy is different. So you cannot say a simple yes or no across the board. In general, we've been successful, and that means that our office calls the insurance company to get pre-approval, and that helps all of us understand an individual's benefits and costs ahead of time. Some insurance companies pay 100 percent, other's don't...so the variation is terrific, and again, pre-approval seems to be the best way to go. For people that want to get an idea as to what the device looks like, they can view a functioning system below.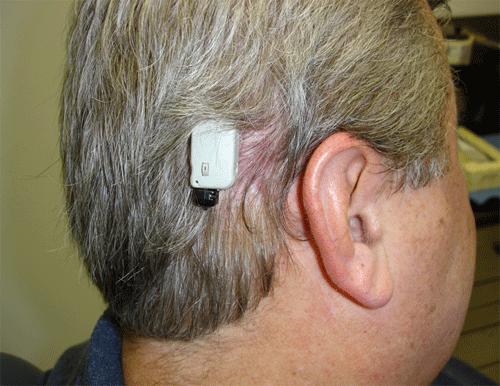
Beck: Thanks so much for your time Dr. Marzo. It's been a pleasure speaking with you.
Marzo: Thank you too, Dr. Beck.
----------------------
View more information on the direct bone conduction system.
For more information on Loyola University Medical Center, visit www.lumc.edu.

