The Buffalo Model is a conceptualization of auditory processing disorders (APD) based on the results of a three-test battery. Each test takes a different look at auditory processing and together they provide more than 30 indicators that help to identify APD and what types of problems it represents.
Audiologists have long been interested in the diagnosis of central auditory disorders; starting in the days when the focus was identifying site-of-dysfunction in patients with brain lesions (Bocca et al., 1954). In the 1970s interest turned to the evaluation of APD in those who have learning and/or communicative problems (Katz & Illmer, 1972). Over the years more and more attention has been directed toward remediation of auditory processing difficulties (Katz & Burge, 1971; Sloan, 1986; Tallal, 1996; Musiek, 1999). First, this article will discuss the Buffalo Battery of tests and relate their results to categories of APD, which in turn will point to therapies and the expected results from therapy. The therapies are geared to address the underlying APD issues, which are expected not only to show improvement on retests but, more importantly, to result in improvement in the related academic and communicative problems.
The Buffalo Model
The Buffalo Model is a coherent approach to the evaluation and remediation of APD. Our first APD test and therapy procedure was Phonemic Synthesis in 1957, followed by the Staggered Spondaic Word (SSW) test in 1961, and the third test and therapy procedure was Speech-in-Noise in 1966. However, the conceptual link between these components was not made until 1986 when the Buffalo Model was conceived. At that time the three central tests were combined into a diagnostic battery, and the various therapeutic procedures that had been used for many years fit in neatly as effective approaches to remediate the underlying auditory processing difficulties. More recently, additional therapeutic measures and evaluation techniques have been added.
Definition of APD
The Buffalo Model definition of APD is, "what we do with what we hear." It is how efficiently and effectively people process what they hear. Our notion is that APD refers to rather basic functions of the central nervous system (CNS), but we recognize that any behavioral speech test or therapeutic procedure requires some language and cognitive knowledge. There is no clear line between where auditory processing ends and where language or higher cognitive functions begin. We do believe that understanding speech in quiet as well as in noise, dichotic listening, short-term/working auditory memory, sequencing, and sound localization are among the many functions that are heavily dependent upon auditory processing skills. We feel particularly confident in this, in part, because such difficulties respond so well to basic auditory therapies.
The Buffalo Battery
Prior to evaluation with the Buffalo Battery pure-tone thresholds, tympanometry and acoustic reflexes should be carried out to determine the status of the person's peripheral hearing and middle ear functions. This is necessary because hearing loss, as well as fluid in the middle ear, can influence performance on central tests; such conditions should be compensated for (e.g., using higher presentation levels) and/or taken into account when making interpretations from the data.
The SSW Test - was devised to evaluate auditory function in patients with brain lesions (Katz, 1961), but because of its makeup and complexity it turned out to be sensitive to various components of auditory processing. For example, one can study the performance for right and left ears individually as well as when they are competing with one another (Katz, 1968; Katz & Pack, 1975). Odd-numbered items begin in the right ear and even-numbered items begin in the left ear. Thus, one can compare these two halves of the test to see if there is a significant difference. Logic would hold that the ear with which the item begins would make no difference. However, we quickly learned that some brain-lesioned patients perform significantly better in one condition (Berlin, Chase, Dill & Hagepanos, 1965) and others perform significantly better in the other. It turned out that the site of lesion differed for these two groups (one with lesions anterior to the post-central gyrus and the other involving the auditory cortex) (Katz, 1977). The SSW gains further power from test findings and behaviors called response biases and qualifiers. The SSW test was used to establish the four categories of the Buffalo APD Model based on the findings with numerous brain-lesioned patients over more than 25 years of testing and research. The SSW provides test indicators for each of the four CAP categories (Katz & Smith, 1991; Katz, 1992).
The Phonemic Synthesis (PS) Test - focuses on the discrimination of individual speech sounds, the degree to which they are remembered effectively, and how such sounds are synthesized into words (Katz & Harman, 1981). These are the same three characteristics that were noted by Luria (1966; 1970) as functions specific to the auditory cortex of the brain, where phonemic decoding takes place. In this test individual phonemes are presented one at a time (about 1 to 1.5/second) and the listener is asked to say the word that was produced (e.g., /s-u-p/ = soup). The PS test has indicators of three APD categories, but primarily indicates decoding difficulties (Katz, 1998).
The Speech in Noise Test - is used to analyze a person's understanding when foreground speech is competing with background noise in the same ear (Mueller & Bright, 1994). In this battery, modified W-22 words are presented at a +5 dB signal-to-noise ratio (SNR) for each ear. This score is subtracted from the score in quiet for the same ear. The Speech in Noise test is an important indicator of the Tolerance-Fading Memory (TFM) category of APD, as well as a practical clinical measure, as complaints of difficulty understanding speech in noise are prevalent in patients diagnosed either with APD or hearing loss (Katz, 1992).
This battery of central tests contains many indicators of APD; however, administration of all three tests generally require only 30 to 45 minutes. The brevity is most helpful when testing children who are hyperactive, distractible or have short attention spans. The Buffalo Battery is available on CD along with a comprehensive manual from Precision Acoustics (360-892-9367). Additionally, the SSW-Plus computer program is available for calculating, interpreting, and recommending habilitation from the Buffalo Battery (distributed by Gary Bricault: 585-381-3459, or [email protected]).
APD Categories
Based on the functions and test signs that are associated with various sites of lesion (Katz, 1968; 1972; Katz & Pack, 1975; Katz, Avellanosa, & Aguilar-Markulis, 1980), APD categories were developed (Katz & Smith, 1991; Katz, 1992). As in most fields, categories enable us to break down complex problems into smaller understandable units. This classification has been extremely helpful in understanding APD and in developing treatment plans to remediate it. It is heartening to note that the other major category system, developed by Bellis and Ferre (Bellis, 2002), is quite similar to the Buffalo Model. This indicates that groups of knowledgeable audiologists have found consistency in their analyses of auditory processing deficits even when using different central tests.
The impetus for developing the Buffalo Model started with a comment from a speech-language pathologist who had low regard for APD. He said, "what you guys need is a theory." The way that I could best conceptualize auditory processing was to think in terms of anatomy and physiology based on years of evaluating and researching the performance of those with CNS lesions. The Buffalo Model is made up of four major categories that are discussed below.
The Decoding Category - refers to the ability to quickly and accurately digest speech, most importantly at the phonemic level. Indeed, phonemic recognition is basic to words and sentences and is closely correlated with them (Boothroyd, 1968; Nittrouer & Boothroyd 1990). Anatomically, phonemic decoding of speech is uniquely associated with the auditory cortex of the brain. Luria (1966, 1970) points out that the middle-posterior portion of the superior temporal lobe is responsible for phonemic discrimination, phonemic memory, and phonemic synthesis-analysis. Interestingly, these are the skills required by the PS test and are the ones trained in PS therapy. Katz (1962) pointed out that those with lesions to this region of the brain demonstrated large error peaks on the SSW test in the contralateral ear, as well as significantly greater numbers of errors at the ends of the items compared to the beginnings (i.e., Order Effect low/high) (Wilson, 1979; McCarthy, 1981). This latter indicator is associated with slow processing, as seen in those with auditory decoding problems. Similar findings were noted in other types of speech analyses by Burns & Canter (1977) and Tallal (1980).
Tolerance-Fading Memory (TFM) Category - refers to two skills that are often found together. The word "tolerance" refers to understanding speech in noise and "fading memory" refers to auditory short-term or working memory. "Various" related characteristics such as attention (Tillery et al., 2000) are also combined into the TFM category. There appears to be no functional connection between these factors. However, blocking out noise, short-term/working auditory memory, attention, and other TFM signs are associated with anterior portion of the brain (Efron et al., 1983; Luria, 1966); therefore, the connection among them may be anatomical. We look for signs such as Order Effect high/low (having significantly more errors on the first parts of items than on the last) which is associated with limited short-term memory (a primacy error). In addition, we are likely to see one or more significant Speech in Noise scores for the individual.
Integration Category - is a complex and variable disorder (Katz & Ivey, 1994) that is associated with the corpus callosum. The major indicator of the Integration category of the Buffalo Model is the SSW Type-A pattern, in which the left competing condition for the left-ear-first items is significantly poorer than any of the other columns (especially in right-handed individuals). This pattern is commonly seen in those with severe reading and/or spelling problems and who are sometimes labeled Dyslexic. Integration cases tend to have more tenacious problems than others with APD. Katz, Avellanosa & Aguilar-Markulis (1980) found Type-A SSW patterns in one-third of their corpus callosum tumor cases.
Organization Category - In the earliest SSW records for brain-damaged patients we found evidence of sequencing problems and later on noted the same confusion in those with APD cases. SSW and PS sequencing errors are considered reversals. On the SSW test if there is only one error or no errors on an item that is out of sequence; it is counted as a reversal. Lucker (1981) pointed out that those who have SSW reversals tend to be disorganized and were generally unable to follow directions sequentially. Since then we have verified that keen observation over and over again. We find the same thing to be true for PS reversals, although most often those who make word reversals may not be the same individuals who make phoneme reversals. Both Luria (1970) and Efron (1963) noted auditory sequencing errors in the same fronto-temporal and fronto-temporal-parietal regions as we found on the SSW test (Katz & Pack, 1975).
Diagnosis and Verification
APD categories are not mutually exclusive; in fact, the vast majority of those seen for APD testing demonstrate problems in two or more categories. It is likely that people who have just one area of dysfunction have milder APD and are able to compensate more effectively than those who have two or more categories to contend with. Roughly 5-10% of the cases seen in my practice demonstrated all four categories of dysfunction. On the Buffalo Battery we look for confirmation from other test signs, as well as from observations "on the ground". That is, we expect independent observations of parents and teachers to coincide fairly well with our findings.
The Buffalo Model Questionnaire (BMQ) has 48 items dealing with potential problems and six types of therapy that can influence (improve) central test results. Some items from the BMQ are shown in Table 1. The case history form has additional questions dealing with APD as well as hearing disorders. At the time of the retest, the parents are given a form addressing their initial concerns and an opportunity to rate whether these issues have improved, gotten worse, or remain the same. We expect, and do find in almost all cases, that those issues dealing with our therapy are shown to improve. In the final analysis, the most important outcome for those with APD is improvement in their academic and communicative problems. When we see improvement on our therapy materials and central tests, and the parents and teachers independently report improvement at school and home, we consider this validation of both our initial diagnoses and therapeutic procedures.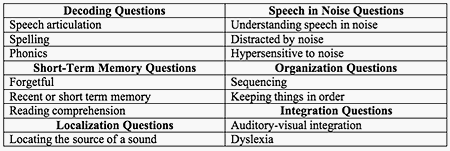
Table 1. Selected items from the Buffalo Model Questionnaire and case history
form relating to specific aspects of APD.
The Role of Attention & Temporal Processing
There have been questions with the Buffalo Model as it relates to attention, more specifically, Attention Deficit Hyperactivity Disorder (ADHD). Tillery et al. (2000) found that attention in children with ADHD is not a significant influence on the results of the Buffalo battery. Using a double-blind design, over 60 children who were diagnosed with ADHD were evaluated using the Buffalo test battery without their usual Ritalin® medication. Thirty-four of those subjects who were identified with significant APD were then reevaluated on Ritalin® or a placebo. The Ritalin® subjects were superior to those taking a placebo on an auditory attention test, but there was no significant difference between the groups on the any of the tests in the Buffalo battery. In other words, despite improved attention the scores on the Buffalo battery were not affected.
Temporal processing has also been of recent interest (Musiek, et al., 2005) as it relates to the use of non-verbal testing for APD. While temporal processing is not addressed directly in the Buffalo model, this type of processing likely relates to decoding in our model. Regardless, the Buffalo model is effective for both evaluation and therapy with speech, without specifically testing or remediating temporal processing, per se.
Therapy for Auditory Processing Disorders
A program of therapy can be set up based, in large part, on an individual's diagnostic profile. For those with decoding problems we strongly recommend phonemic training, emphasizing individual speech sounds. For those with TFM problems we recommend Speech-in-Noise (SN) desensitization and Auditory Memory Training. For auditory Organization problems we recommend therapy for what we believe is the underlying problem: sequencing. For those who have Integration problems we generally recommend dichotic listening training and some non-auditory approaches. In addition, for those who have localization of sound difficulties we recommend an approach called Localization Clock training. Our major emphasis here will be on the decoding and speech-in-noise therapies because of the author's longtime experience with them.
Phonemic Training Program (PTP) - The PTP as well as the PS program are discussed below; both address Decoding issues. Both can be administered during the same therapy session, although the PTP is more basic than the PS program. It has been used with great success with those who have cochlear implants (Katz, 1998; Katz & King, 2001), are mentally challenged, hard of hearing, and those with difficulty speaking English as a second language. We have used it with children as young as four years of age, as well as with the elderly and those who have neurological disorders.
PTP employs a deck of cards with the letters of the alphabet printed on them corresponding to the sounds that will be taught. Additional markings should be used on the cards to distinguish, for example, long and short vowels as well as voiced and voiceless Th-sounds. An acoustically transparent screen is also used to prevent visual identification of the sounds from the face and lips. A more complete discussion of PTP is provided elsewhere (Katz, 2007). The three steps in PTP are shown in Table 2.
Table 2. . PTP steps for the first three sessions and those that follow. At each
session the previous sounds are reviewed, and then four new sounds are introduced.
In the first PTP session we start with four new sounds (e.g., D, short-E, M, and H). These sounds were chosen because they tend to be quite difficult for most children with APD. However, the task is quite simple because these sounds are easily distinguished from one another. The previous sounds are reviewed in subsequent sessions; therefore, the sounds that are most challenging are heard many times during the therapy program.
PTP starts with a procedure called Introduction Without Bias. Each sound is introduced separately as follows: "I'm going to say a sound a few times, just listen carefully to it; don't repeat it: /d/.../d/......./d/. That was the /d/ sound (show the card with the D on it) that we hear in a word like 'door, day' and even the word 'food'. Do you hear the /d/ in the word 'food'?" Put the card in front of the child and say, "each time I say /d/ please point to this card". After one or two presentations, followed by appropriate pointing, explain that if you say a different sound such as /s/ the person should point to a designated place on the table to indicate that the sound was not represented on any of the cards shown.
The first card (i.e., D) is removed and the second sound (short-E) is presented in the same way using the Introduction Without Bias procedure. An occasional foil (e.g. /z/) that is nothing like the sound being taught can be presented in order to keep the individual tuned into the task.
Now the two sounds may be contrasted. Because they are so different acoustically, we can assume the task will be an easy one. Each time a sound is presented the person points to the card. The D and short-E are each presented once and, if desired, may be presented once again if there was a hesitation or an error. Both cards are removed and the third new sound /m/ is introduced without bias. Then the previous two sounds are placed in front of the child again and the three sounds are tested. Usually one round of each sound and occasionally a foil is sufficient. As before, the cards are removed and the fourth sound is presented. Then all four sounds are contrasted.
During this simple procedure the sounds are heard quite a few times individually and associated with particular letters, which makes the listening task more concrete. In the next therapy session (as shown in Table 2) we start with Introduction & Review. That is, we review the sounds from the previous session, much as it was done originally, although generally in an abbreviated form. In this way prior to introducing the new sounds, the previous sounds are given another chance to 'adhere' to the child's brain. The next step is to present the four new sounds for this session using the Introduction Without Bias procedures as in the previous session. The sounds T, short-A, L and N would be appropriate because they, too, are often difficult for those with APD, but are not likely to be confused with one another.
In the third session, and in most of the following sessions, all three steps of PTP are administered. The previous week's new sounds are given first in the Introduction & Review followed by a Review step. The Review sounds are those that were introduced two sessions before and briefly reviewed in the last session. For example, in the third session D, short-E, M, and H are placed in the Review group and remain there in subsequent sessions. On the fourth session D, short-E, M, and H and T, short-A, L, and N are all mixed together and presented in a random order 4 at a time (not one-by-one). In this way sounds that were taught individually without significant competition are now introduced randomly and often presented with more challenging comparisons (e.g. m/n, short-A/short-E). After about eight sessions there will be too many sounds to review each time, so some of the easier sounds can be omitted from the Review step.
Phonemic Synthesis (PS) Program - The PS program (available on CD from Precision Acoustics, see page 2) also addresses Decoding problems. Like the PTP, individual speech sounds are presented but in this case they must be discriminated (recognized from all possible sounds), remembered, and successfully blended together in order to respond with the correct word. Unlike the PTP, the PS program presents a wider range of speech sounds throughout the program. The sounds of the word are presented at a rate of 1 to 1.5 seconds per sound, which provides generous pauses between sounds. The sounds are associated with words, and in this way the PS program has a beneficial effect on spelling and oral reading accuracy (Kahler, 1983) as well as speech (Katz & Medol, 1972).
There are 15 programmed lessons that start off very easy and increase in difficulty with each successive lesson. The first three lessons are presented in a multiple-choice format to get the person started, and then gradually such aids are removed until the individual is able to handle easy and difficult sounds in easy and difficult combinations for shorter and longer words (see Katz, 2007).
The first controlled study using both PTP and PS programs is nearing completion and suggests positive results (Montgomery, Katz, & Walker, 2007). Clinical results by Katz (2007) are reported elsewhere.
Speech-in-Noise (SN) Desensitization Training - One aspect of TFM is difficulty understanding speech in noise. To remediate this problem we have used a desensitization approach for many years. Just as the allergist increases one's tolerance for allergens by gradually increasing doses of the allergens, speech in noise desensitization training follows the same principle using increasing levels of noise with a constant level of speech (Katz and Burge, 1971).
Speech-in-noise training uses recorded words. I believe that the best speech signals to use are monosyllabic words. Some people prefer sentences, running speech, or questions. Because the basic auditory processing task is to learn how to pull speech out of a background of noise, higher-level strategies using linguistic or other cognitive skills may, in fact, reduce the more basic learning because of compensatory strategies. Monosyllabic words are a more challenging linguistic unit because they demand that we accurately recognize most, if not all, of the component sounds.
The noise source is not as critical. I believe that cafeteria noise and multi-talker noise are excellent competition for this task. Whenever possible, a consistent noise level should be used to maintain a fairly consistent SNR for any particular noise level. It is most appropriate to have the recorded speech directed to one channel of the audiometer and the noise to the second channel. In this way the speech can be presented at a comfortably-loud level and the noise presented at varying intensities. "A series" is a group of presentations generally starting with no noise and gradually increasing to a high level of noise. One or more series can be presented during the therapy session.
Generally, we start with speech through a loudspeaker(s) (or headphones if there is too much ambient noise) at a comfortably loud level (e.g., 60 dB HL) and no noise. We present 10 words at each intensity level and record the errors on the score sheet. Initially, for young children we generally follow the no-noise presentation with a fairly mild noise level presentation. For adults, a SNR of +10 or +12 dB is a good place to begin the noise unless the person is very apprehensive or sensitive to challenging noise levels. After 10 words at each noise level the competition is raised by 2 dB. The series is terminated when the person makes quite a few errors or shows significant anxiety or tension. Initially for most individuals, using our speech list and noise, a +2 dB SNR is generally tolerable early in the therapy and for most individuals a 0 dB SNR is tolerable later on. If an individual has six or seven errors at one noise level we generally do not raise the noise to a more challenging level. However, it should be stated that on a few occasions when we have raised the levels after a very poor performance, some individuals had better scores than at the lower level. Often after a difficult listening challenge, some people are able to develop more effective approaches and thus improve their performance.
When individuals have more difficulty with noise in one ear than the other, it is appropriate to give that ear more training in order to equate the performance of the ears. This is generally carried out under headphones. Benefits from speech-in-noise therapy are generally reflected on speech in noise retests.
Short-Term Auditory Memory Training - Many people who have APD also have difficulty with short-term auditory memory. Therefore, memory training is an important therapy; however, due to my own memory problem I rarely administer this therapy because I would not know if it was my problem or the patient's. However, I have worked with some people who definitely had much poorer short-term memories than mine.
As in each of the other therapies we start with easy materials and gradually increase the difficulty level. Generally, digits are good to work with because we often have to remember them (e.g., telephone numbers and addresses) and because the discrimination task is simple as each digit is quite distinctive. It is first necessary to determine at what level the individual is functioning. A list of randomized digits is prepared prior to the session to see if the person can repeat two, three, four, or more digits. Once the person's digit threshold is determined, it is well to start the therapy one step below. That is, if the individual is not consistently able to recall four digits then therapy begins with three digits to establish positive performance and to firm up their skill at this level.
When the person is ready to move to four digits, training can begin with easier presentations. For example, 1, 2, 8, 9 is a lot easier to remember than 9, 4, 7, 2. This eases the individual into the new level, and as they develop the skills the listening task can be increased in difficulty. When the individual is able to repeat four digits on a consistent basis, then five digits can be trained in the same way. After working on digits, one might train individual words and later sentences with the intent of eventually working on commands.
Auditory Sequencing Training - Auditory sequencing training can be taught in much the same manner as short-term memory; however, in this case the person is asked to maintain the proper sequence. In the beginning, sequencing training should involve digits spans that can be readily remembered, so the individual is not working on two difficult tasks at the same time.
Dichotic Offset Training (DOT) - I am currently experimenting with Dichotic Offset Training (DOT) to teach the individual how to listen effectively with both ears to different stimuli. For DOT we use four letters of the alphabet in each item in the format of the SSW test. That is, two letters are directed to the right ear and two letters to the left ear. In the truly dichotic condition (zero millisecond offset for the competing letters) the second letter to the right ear and the first letter to the left are presented simultaneously. One group of 10 or more items begins in the right ear and another group begins in the left ear so that the person can learn to perform better in these two slightly different conditions. For most people with APD, the left-ear-first (LEF) condition is more challenging relative to the right-ear condition. The training starts with competing words separated by 500 ms; gradually the offset is reduced by 100 or 50ms for subsequent conditions.
Typically, listeners are able to improve their DOT performance for a particular condition on the retest measure (Katz, Chertoff & Sawusch, 1984). Listeners gradually learn how to process the auditory information more effectively, even as the dichotic challenge increases. When the task becomes quite difficult, other strategies may be used. For example, one strategy includes presenting the two letters to the left ear without competition in the right ear, and then repeating the item in the normal fashion. Benefit from this therapy can be seen with the therapy materials themselves as well as on dichotic listening tests.
Localization Clock Training - An additional therapy technique to improve the ability to locate sounds in space is called the Localization Clock system. Numbers from 1 to 12 are placed in a circle on the floor to represent a clock with a diameter of roughly 7 to 8 feet. In the middle of the circle we place a dot that represents the point over which a chair is centered.
For training purposes, the client is seated on the chair in the middle of the clock with eyes closed, facing the 12-o'clock card directly in front. Music or other noises are used to conceal the movement of the therapist. The therapist stands on an hour or half hour point and stops the music or background noise. The therapist then gives a brief verbal signal, for example the word, "test". The listener points to where he or she believes the speaker's mouth is. The listener is then asked to visually verify their response. If the response is incorrect, they can see how far off they were. Then the person is asked to close their eyes and face forward again and the test word is repeated. Generally, the second try is closer than the first. It is reinforcing when they see they were correct, and it is instructive when they see their misperception. Often 10 minutes for six sessions is all that is needed to make major gains in this localization skill. Pre- and post-testing on a Localization Clock task (with the 24 points around the clock presented randomly) can document initial performance and post-therapy improvement.
Summary and Suggestion
The Buffalo Model procedures have been used with great success for many years. It is an efficient and effective approach to evaluate and remediate APD. It is a logical-coherent system that begins with the anatomy and physiology of the central auditory mechanism and ends in a detailed approach to providing habilitation for auditory processing deficits.
I would like to encourage, if you already use parts of the Buffalo Model (e.g., the SSW test) successfully, to try the PS and/or Speech-in-Noise tests to acquire even greater diagnostic power. If you are not using response bias or qualifiers, do try them. I believe you will be pleased with how much insight you receive, free of charge. Because APD is a highly treatable condition, and if you don't plan to get involved in therapy, please encourage other audiologists or speech-language pathologists to help remedy this disorder. One final note, this paper has focused on the Buffalo Model and the therapy procedures that relate to it. There are other general references on APD that the reader may want to examine including Geffner & Ross-Swain (2007) and ASHA (2005) for additional information.
References
American Speech-Language-Hearing Association. (2005). (Central) Auditory Processing Disorders—The Role of the Audiologist [Position statement]. Available at www.asha.org/members/deskref-journals/deskref/default
Bellis, T. (2002). Developing deficit-specific intervention plans for individuals with auditory processing disorders. Seminars in Hearing, 23, 287-295.
Berlin, C., Chase, R., Dill, A., & Hagepanos, T. (1965). Auditory findings in patients with temporal lobectomies. Asha, 7, 360.
Bocca, E., Calearo, C., & Cassinari, V. (1954). A new method for testing hearing in temporal tumours. Acta Otolaryngologica, 44, 219-221.
Boothroyd, A. (1968). Developments in speech audiometry. British Journal of Audiology, 2, 3-10.
Burns, M., & Canter, G. (1977). Phonemic behavior of aphasic patients with posterior cerebral lesions. Brain Language, 4, 492-507.
Efron, R. (1963). Temporal Perception, Aphasia and Deja Vu. Brain, 86, 403-424.
Efron, R., Crandell, P.H., Koss, B., Divenyi, P.L., & Yund, E.W. (1983). Central auditory processing III: The 'cocktail party effect' and temporal lobectomy. Brain Language, 19(2), 254-263.
Geffner, D, Ross-Swain, D (2007) Auditory Processing Disorders: Assessment Management and Treatment. San Diego: Plural Publishing.
Kahler, L. (1983). Phonemic synthesis: A prediction of early reading success. Paper presented at American Speech-Language-Hearing convention, Cincinnati, OH.
Katz, J. (1968). The SSW Test: An Interim Report. Journal of Speech and Hearing Disorders, 33, 132-146.
Katz, J. (1977). The Staggered Spondaic Word test. In R. Keith (Ed.), Central Auditory Dysfunction (pp. 103-121). New York: Grune & Stratton.
Katz, J. (1983). Phonemic Synthesis and other auditory skills. In E. Lasky and J. Katz (Eds.), Central Auditory Processing Disorders: Problems of Speech, Language and Learning, University Park Press.
Katz, J. (1992). Classification of auditory processing disorders. In J. Katz, N. Stecker, D. Henderson (Eds.), Central Auditory Processing: A Transdisciplinary View (p. 81-92). Chicago: Mosby Yearbook.
Katz, J. (1998). Central auditory processing and cochlear implant therapy. In M.G. Masters, N. Stecker, J. Katz (Eds.), Central Auditory Processing Disorders: Mostly Management (p. 215-232). Boston: Allyn & Bacon.
Katz, J. (2007). Phonemic Training and Phonemic Synthesis programs. In D. Geffner & D. Ross-Swain (Eds.), Auditory Processing Disorders: Assessment, Management and Treatment (255-256). San Diego: Plural Publishing.
Katz, J., Avellanosa, A., & Aguilar-Markulis N. (1980). Evaluation of corpus callosum tumors using the SSW, CES, and PICA. Paper presented at American Speech-Language Hearing Association Convention, Detroit.
Katz, J., & Burge, C. (1971). Auditory perception training for children with learning disabilities. Menorah Medical Journal, 2, 18-29.
Katz, J., & Harmon, C. (1981). Phonemic Synthesis: Diagnostic and Training Program. In R. Keith (Ed.), Central Auditory and Language Disorders in Children. Houston: College Hill Press.
Katz, J., & Illmer, R. (1972) Auditory perceptual problems in children with learning disabilities. In J. Katz (Ed.), Handbook of Clinical Audiology. Baltimore: Williams & Wilkins.
Katz, J., & Ivey, R. (1994). Spondaic procedures in central testing. In J. Katz (Ed.), Handbook of Clinical Audiology, 4th Edition (pp. 249, 253). Baltimore: Williams & Wilkins.
Katz, J., & King, J. (2001). A CAP approach for people with cochlear implants. Contact, 14, 39-42.
Katz, J. & Medol, E. (1972). The use of Phonemic Synthesis in speech therapy. Menorah Medical Journal, 3, 10-13.
Katz, J., & Pack, G. (1975). New developments in differential diagnosis using the SSW test. In M. Sullivan (Ed.), Central Auditory Processing Disorders. Omaha: University of Nebraska Press.
Katz, J., Chertoff, M., & Sawusch, J. (1984). Dichotic Training. Journal of Auditory Research, 24, 231-264.
Katz, J., & Smith, P. (1991). A ten minute look at the CNS through the ears: using the SSW test. Annals New York Academy of Sciences, 620, 233-252.
Lucker, J. (1981). Interpreting SSW test results of learning disabled children. SSW Newsletter, 3, 7-9.
Luria, A.R. (1966). Higher Cortical Functions in Man. New York: Basic Books.
Luria, A.R. (1970). Traumatic Aphasias Its Syndromes: Psychology and Treatment (p. 118-119, 122, 267-268). The Hague: Mouton.
McCarthy, D.L. (1981). A Cross Validation of the SSW and CES Tests in Detecting Lesions of the Central Auditory Nervous System, M.A. Thesis, University at Buffalo.
Montgomery, N., Katz, J., Walker, M. (2007). Why Can't Mario Read? Missouri Speech-Language Hearing Association convention, Osage Beach, MO.
Mueller, H.G., & Bright, K. (1994). Monosyllabic procedures in central testing. In J. Katz (Ed.), Handbook of Clinical Audiology (pp. 222-238). Baltimore: Williams & Wilkins.
Musiek, F. (1999). Habilitation and management of auditory processing disorders: Overview of selected procedures. Journal of American Academy of Audiology, 10, 329-342.
Musiek, F., Shinn, J., Jirsa, R., Bamiou, D., Baran, J., & Zaidan, E. (2005). The GIN (Gaps in Noise) Test Performance in Subjects with and without Confirmed Central Auditory Nervous System Involvement, Ear & Hearing, 26, 608-618.
Nittrouer, S., & Boothroyd, A. (1990). Context effects in phoneme and word recognition by young children and older adults. Journal of the Acoustical Society Of America, 87, 2705-2715.
Sloan, C. (1986). Treating Auditory Processing Difficulties in Children. San Diego: College-Hill Press.
Tallal, P. (1980). Auditory processing disorders in children. In P. Levenson, and C. Sloan (Eds.), Auditory Processing and Language (pp. 81-100). New York: Grune & Stratton.
Tallal, P., Miller, S., Bedi, G., Byma, G., Wang, X., Nagarajan, S., Schreiner, C., Jenkins, W. & Merzenich, M. (1996). Language comprehension in language-learning impaired children improved by acoustically modified speech. Science, 271, 81-84.
Tillery, K., Katz, J., & Keller, W. (2000). Effects of methylphenidate (Ritalin TM) on auditory performance in children with attention and auditory processing disorders. Journal of Speech-Language and Hearing Research, 43, 893-901.
Wilson, L. (1979). A Cross Validation of the SSW and CES Tests in Detecting Lesions of the CNS. M.A. Thesis, University at Buffalo.
APD Evaluation to Therapy: The Buffalo Model
May 14, 2007
Related Courses
1
https://www.audiologyonline.com/audiology-ceus/course/cortical-auditory-evoked-potentials-in-39954
Cortical Auditory Evoked Potentials in a Pediatric Practice
This course explores how to use the Cortical Auditory Evoked Potential for verifying hearing technologies on the user, evaluating the severity of Auditory Neuropathy Spectrum Disorder, and evaluating pediatric patients with Auditory Processing Disorders. Real world Cortical tracings and how to apply normative data to them are discussed.
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Cortical Auditory Evoked Potentials in a Pediatric Practice
This course explores how to use the Cortical Auditory Evoked Potential for verifying hearing technologies on the user, evaluating the severity of Auditory Neuropathy Spectrum Disorder, and evaluating pediatric patients with Auditory Processing Disorders. Real world Cortical tracings and how to apply normative data to them are discussed.
39954
Online
PT60M
Cortical Auditory Evoked Potentials in a Pediatric Practice
Presented by Shanda Brashears, AuD
Course: #39954Level: Advanced1 Hour
AAA/0.1 Advanced; ACAud inc HAASA/1.0; ASHA/0.1 Advanced, Professional; BAA/1.0; CAA/1.0; Calif. SLPAB/1.0; IACET/0.1; IHS/1.0; Kansas, LTS-S0035/1.0; NZAS/1.0; SAC/1.0
This course explores how to use the Cortical Auditory Evoked Potential for verifying hearing technologies on the user, evaluating the severity of Auditory Neuropathy Spectrum Disorder, and evaluating pediatric patients with Auditory Processing Disorders. Real world Cortical tracings and how to apply normative data to them are discussed.
2
https://www.audiologyonline.com/audiology-ceus/course/20q-auditory-processing-disorders-there-39454
20Q: Auditory Processing Disorders - Is There a Gold Standard?
This course describes the origins and current views on the auditory processing disorder (APD) construct. This course includes a discussion of the identification of the “gold” or reference standard test (or test battery) used for the diagnosis of an APD.
textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
20Q: Auditory Processing Disorders - Is There a Gold Standard?
This course describes the origins and current views on the auditory processing disorder (APD) construct. This course includes a discussion of the identification of the “gold” or reference standard test (or test battery) used for the diagnosis of an APD.
39454
Online
PT120M
20Q: Auditory Processing Disorders - Is There a Gold Standard?
Presented by Andrew J. Vermiglio, AuD
Course: #39454Level: Intermediate2 Hours
AAA/0.2 Intermediate; ACAud inc HAASA/2.0; AHIP/2.0; ASHA/0.2 Intermediate, Professional; BAA/2.0; CAA/2.0; Calif. SLPAB/2.0; IACET/0.2; IHS/2.0; Kansas, LTS-S0035/2.0; NZAS/2.0; SAC/2.0
This course describes the origins and current views on the auditory processing disorder (APD) construct. This course includes a discussion of the identification of the “gold” or reference standard test (or test battery) used for the diagnosis of an APD.
3
https://www.audiologyonline.com/audiology-ceus/course/using-amplification-to-address-functional-37924
Using Amplification to Address Functional Hearing Loss and Auditory Processing Disorders
This presentation is designed to discuss the role of hearing aids/amplification in the treatment of functional hearing losses/auditory processing disorders.
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Using Amplification to Address Functional Hearing Loss and Auditory Processing Disorders
This presentation is designed to discuss the role of hearing aids/amplification in the treatment of functional hearing losses/auditory processing disorders.
37924
Online
PT60M
Using Amplification to Address Functional Hearing Loss and Auditory Processing Disorders
Presented by Gail Whitelaw, PhD
Course: #37924Level: Intermediate1 Hour
AAA/0.1 Intermediate; ACAud inc HAASA/1.0; AHIP/1.0; ASHA/0.1 Intermediate, Professional; BAA/1.0; CAA/1.0; Calif. SLPAB/1.0; IACET/0.1; IHS/1.0; Kansas, LTS-S0035/1.0; NZAS/1.0; SAC/1.0
This presentation is designed to discuss the role of hearing aids/amplification in the treatment of functional hearing losses/auditory processing disorders.
4
https://www.audiologyonline.com/audiology-ceus/course/auditory-processing-disorder-and-blast-31270
Auditory Processing Disorder and Blast Trauma
This course will focus on the current approach to blast trauma and the role of the audiologist in working with this population. Characteristics, assessment tools, and treatment will be discussed.
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Auditory Processing Disorder and Blast Trauma
This course will focus on the current approach to blast trauma and the role of the audiologist in working with this population. Characteristics, assessment tools, and treatment will be discussed.
31270
Online
PT60M
Auditory Processing Disorder and Blast Trauma
Presented by Gail Whitelaw, PhD
Course: #31270Level: Advanced1 Hour
AAA/0.1 Advanced; ACAud inc HAASA/1.0; BAA/1.0; CAA/1.0; Calif. SLPAB/1.0; IACET/0.1; IHS/1.0; Kansas, LTS-S0035/1.0; NZAS/1.0; SAC/1.0
This course will focus on the current approach to blast trauma and the role of the audiologist in working with this population. Characteristics, assessment tools, and treatment will be discussed.
5
https://www.audiologyonline.com/audiology-ceus/course/auditory-processing-disorder-counseling-38443
Auditory Processing Disorder: Counseling
This course provides information on interpretation of case history information and test results, and will guide DoD and VA audiologists in discussing the complexities of hearing health with patients experiencing subjective communication issues in the presence of background noise. Recommendations and additional referral considerations are discussed in detail.
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Auditory Processing Disorder: Counseling
This course provides information on interpretation of case history information and test results, and will guide DoD and VA audiologists in discussing the complexities of hearing health with patients experiencing subjective communication issues in the presence of background noise. Recommendations and additional referral considerations are discussed in detail.
38443
Online
PT60M
Auditory Processing Disorder: Counseling
Presented by Kimberly Jenkins, AuD, Indiana Gutierrez, AuD
Course: #38443Level: Intermediate1 Hour
ASHA/0.1 Intermediate, Professional; IACET/0.1
This course provides information on interpretation of case history information and test results, and will guide DoD and VA audiologists in discussing the complexities of hearing health with patients experiencing subjective communication issues in the presence of background noise. Recommendations and additional referral considerations are discussed in detail.


