What do aural rehabilitation, auditory processing and cochlear implants have in common? Anticipated coding and reimbursement changes will link the three together in significant ways. Piecing together auditory processing evaluation and treatment, aural rehabilitation, and diagnostic programming of cochlear implant speech processors into different payment puzzles, such as Medicare, Medicaid, and private health plans can be a formidable task. This article focuses on billing and obtaining reimbursement for audiology services.
Third-Party Payers
One reason for the complexity is that the plethora of third party payers--
Medicare, Medicaid, and private health plans--have different coverage criteria and reimbursement policies. Medicare is administered at the federal level by the Centers for Medicare and Medicaid Services (CMS), whereas Medicaid is administered jointly by the federal and state governments. The result in that coverage of audiology services varies significantly from state to state. Private health plans are typically offered by commercial insurance companies (e.g., Aetna and Prudential) and by non-profit health service corporations (e.g., Blue Cross and Blue Shield) and can be classified as either fee-for-service or managed care. Managed care is broken down into health maintenance organizations (HMOs) and preferred provider organizations (PPOs)— with point of service (POS) options for both. More information about managed care can be found at https://professional.asha.org/resources/reimbursement/intro_to_managed_care.cfm.
Medicare, Medicaid, and private health plans do have something in common—they use the same language (i.e., the same codes). That common language makes it easier to explain how to fit these three audiology practice areas into three different payment puzzles and offers some instruction about procedural and diagnostic coding.
I. Aural Rehabilitation
Payers. One reason for the complexity associated with reimbursement for aural rehabilitation is the mindset of payers. Payers receive considerably more claims for diagnostic audiology services than for rehabilitative audiology services. Since its inception, the Medicare program has covered audiology as a diagnostic service. Thus, payers tend to perceive audiology as a diagnostic service only. Therefore, we recommend that the audiologist or the patient's family review the patient's health plan and request clarification in writing of the coverage for audiology and rehabilitation services, before services are rendered.
Procedural Coding. All health plans, whether private or governmental, require health care providers to use the American Medical Association (AMA) Current Procedural Terminology (CPT) when submitting claims for reimbursement. Depending on its coverage criteria and reimbursement policies, the payer then determines if the service is covered and if the practitioner is permitted by the plan to be reimbursed for the service. There are very few rehabilitation or treatment codes for audiology services, while there are a myriad of diagnostic audiology codes.
The AMA's CPT manual, in the Special Otolaryngologic Services section, assigns three codes for aural rehabilitation:
92507 Treatment of speech, language, voice, communication, and/or auditory processing disorder (includes aural rehabilitation); individual
92508 group, two or more individuals
92510 Aural rehabilitation following cochlear implant (includes evaluation of aural rehabilitation status and hearing, therapeutic services) with or without speech processor programming
While the descriptors for these three codes appear straightforward, the reimbursement for each is not. For example, a payer most likely will deny a reimbursement claim for 92507 filed by an audiologist in the event that a speech-language pathologist submitted the same code on the same day for the same patient. This occurs even if the audiologist provided cochlear implant related aural rehabilitation to the patient and the speech-language pathologist provided treatment for the patient's articulation disorder.
The confusion is due in part to the code descriptor, which is not unique to aural rehabilitation. The descriptor for CPT 92507 allows it to be used for more then one type of treatment. As such, the payer cannot differentiate the two services and rejects the second claim as a duplicate. Thus, in order to get paid, an audiologist and a speech-language pathologist must not submit a claim for the same service code on the same day for the same patient.
Another idiosyncrasy associated with aural rehabilitation is the use of 92510 by a practitioner who performs only aural rehabilitation, and does not program the cochlear implant speech processor. The high reimbursement rate associated with this code is due to the time involved in the diagnostic programming of a cochlear implant speech processor and the cost of the equipment needed to program the implant. Currently, speech-language pathologists and audiologists can use either 92507 or 92510 when seeing a patient with a cochlear implant. However, ASHA anticipates 92510 will soon become the code of choice for aural rehabilitation because of its considerably higher reimbursement rate. Unfortunately, the use of 92510 for both diagnostic programming and aural rehabilitation services has resulted in reimbursement difficulties for audiologists under the Medicare program. The American Medical Association is reviewing the "with or without speech processor programming" phrase in the CPT descriptor for 92510 with the goal of ensuring that the phrase does not meaningfully change the value of the procedure.
The use of CPT codes will become truly universal in billing when the electronic data interchange regulations of the Health Insurance Portability and Accountability Act of 1996 (HIPAA) becomes effective in October 2002, unless an extension plan has been submitted. For more information on HIPAA, refer to ASHA's Web site at https://professional.asha.org/resources/legislative/hipaa.cfm.
Medicare. In 1988, the director of the Office of Coverage Policy of the Health Care Financing Administration (HCFA, the predecessor to CMS) wrote to ASHA regarding broadening the scope of Medicare coverage of aural rehabilitation,
"Speech reading is currently the only covered therapeutic aural rehabilitative service. Although auditory training may be one aspect of a speech pathologist's scope of practice, it is not an aspect covered by Medicare Part B because it does not relate to a speech or language disorder that has resulted in a communication disability."
ASHA had requested that aural rehabilitation be covered as both an audiology and speech-language pathology benefit.
The Medicare statute (Title XVIII of the Social Security Act) defines audiology as a diagnostic service. Even before the statute was amended in 1994 to include audiology2, CMS covered audiology services as diagnostic only.3 Medicare does not cover hearing aids or services related to hearing aids.4 For speech-language pathologists, Medicare limits aural rehabilitation to speech reading training. While there is no national guidance on this issue, local contractors for Medicare (fiscal intermediaries and carriers) may draft local medical review policies (LMRPs) to provide clarification.
A local medical review policy (LMRP) for speech-language pathology services available on CMS's Web site for such documents5 states:
Currently, speech reading is the only therapeutic service covered under aural rehabilitation. Speech reading may be covered where a patient exhibits a severe hearing loss, which cannot be helped with the use of a hearing aid and/or speech discrimination that cannot be helped with the use of a hearing aid. If group therapy is provided, it must be based on plans of care that are individualized for each member of the group. Services documented as performed on a mass basis, with no distinction as to the individual patient's actual condition and need for services, are not covered.
Trends. The need for aural rehabilitation services is expected to increase dramatically as the number of retirees doubles by 2030 and additional states adopt mandates supporting the early detection of hearing impairment in infants. It is ASHA's hope that these trends will result in enhanced coverage and reimbursement for aural rehabilitation services.
II: Auditory Processing Disorders: Evaluation and Treatment
For decades, individuals with auditory processing disorders (APD) were improperly diagnosed as having hearing loss, attention deficit/hyperactivity disorder, and autism.6 An accurate diagnosis of an APD is essential to avert future misdiagnoses and ensure that those with APD receive appropriate treatment. A central auditory processing (CAP) evaluation will determine if an APD exists and, if so, describe its parameters.
It is imperative that the client and/or family review the client's health plan and request clarification in writing of the coverage for audiology services. You can assist families in obtaining reimbursement by requesting prior authorization from the health plan. This involves providing the health plan with an explanation of the Current Procedural Terminology (CPT) and International Classification of Disease (ICD-9-CM) codes you intend to submit for reimbursement (see box for relevant CPT codes).
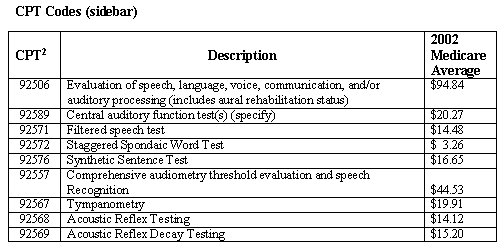
An audiologist performing a CAP evaluation could code in one of two ways depending on whether or not a speech-language pathology evaluation is also performed. Speech-language pathologists performing CAP evaluations typically use 92506 for the evaluation and ICD-9-CM 784.60 for the diagnosis. If both an audiologist and a speech-language pathologist perform portions of the CAP evaluation and both submit claims using 92506, the health plan will reimburse only one 92506 claim and deny the second as a duplicate. Obtaining prior authorization can reduce denials by helping the health plan to understand that audiologists perform the auditory processing segment of 92506 and speech-language pathologists perform the speech-language segment.
Below are two billing scenarios for consideration.

CPT 92506, a code that represents a battery of tests, has a higher work value (i.e., higher reimbursement rate) associated with it than CPT codes for individual CAP tests (e.g., Staggered Spondaic Word test).
An audiologist might also code using Scenario #2 to avoid problems with dual 92506 claims. Please note that Medicare may not allow independent audiologists to bill for CPT 92506.

The total reimbursement is higher in Scenario #2, than for Scenario #1. In addition, there is no concern about 92506 being submitted to the health plan more than once.
*The health plan may reimburse for only one instance of 92589, which would reduce the total claim to $148.42.
Diagnosis Codes
There are a variety of ICD-9-CM codes that are appropriate when performing a CAP evaluation:
388.4 Other abnormal auditory perception
389.9 Hearing loss unspecified (If CAP results are normal)
389.12 Neural hearing loss
389.14 Central hearing loss
784.60 Symbolic dysfunction (i.e., cognitive impairment, language processing problems).
This is commonly submitted by SLPs.
794.15 Abnormal auditory function study (if electrophysiological tests are performed)
III. Cochlear Implants
Medicare Policy. CMS's current interpretation of Medicare laws and regulations do not permit independently practicing audiologists to bill directly for programming cochlear implant speech processors. (See 42 CFR §440.130(a) and Section 2070.3 of the Medicare Carriers Manual.) While audiologists who are employed by physicians may bill "incident to a physician's service," Medicare requires direct personal supervision by a physician "on the premises." See Section 2050.2 of the Medicare Carriers Manual. In 1996, the AMA established CPT 92510 for "aural rehabilitation following cochlear implantation (includes evaluation of aural rehabilitation status and hearing therapeutic services) with or without speech processor programming."
CPT 92510 incorporates two separate and distinct services:
- Programming (or mapping) of the speech processor, performed only by an audiologist (and outside of the scope of practice for speech-language pathologists); and
- Aural rehabilitation (subsequent to cochlear implantation) performed by an audiologist or speech-language pathologist.
As a result of Medicare policy, ASHA learned that several providers are requiring Medicare beneficiaries to pay up-front for the diagnostic programming of the cochlear implant speech processor. As can be imagined, many beneficiaries are unable to afford this up-front payment and are often required to travel significant distances to seek providers who will program their speech processor. This represents an unfortunate impediment to enabling beneficiaries to receive all medically necessary treatment for effective use of a prosthetic device, as required by 42 CFR §410.11(f)(2).
ASHA has recommended that CMS do the following:
- Revise Section 15300(A) of the Medicare Carriers Manual and stipulate that CPT 92510 is to be billed only by qualified audiologists for programming the cochlear implant speech processor. In addition, this section should specify that aural rehabilitation following a cochlear implant be billed under CPT 92507 (by either audiologists or speech-language pathologists), as was the case before January 1, 1996. This change in stipulation would enable carrier systems to recognize programming services apart from aural rehabilitation.
- Revise Section 2070.3 of the Medicare Carriers Manual to allow speech processor programming to be included within Medicare's diagnostic testing criteria and billable directly to Medicare by independently practicing audiologists.
- Revise Section 2050.2 of the Medicare Carriers Manual to recognize that programming is a service within the scope of practice of audiologists for which the requirement of physician supervision "on the premises" is unnecessary.
- As an alternative [see points (2) and (3) above] create a separate section of the Medicare Carriers Manual that would effectively grant an exception to Sections 2070.3 and 2050.2.
- Until such time as system changes can be made to effect the revisions suggested above, issue a Program Memorandum or other directive instructing local carriers to review denials for cochlear implant speech processor programming and pay claims that fit within these amended criteria.
The codes proposed by ASHA's HCEC were revised and approved by the AMA CPT Editorial Panel earlier this year. Subsequently, they were considered by the AMA Health Care Professional Advisory Committee (HCPAC) and the AMA Relative Value Update Committee (RUC) in April 2002. The HCPAC reviews all non-physician procedures and assigns a value (i.e., the factor that converts into an outpatient reimbursement rate) based upon direct practice expense information (e.g., clinical labor, supplies, and equipment) for each proposed code. The RUC then reviews the HCPAC's recommendations. If the RUC agrees with the HCPAC recommendations, the information is forwarded to CMS for their consideration in the Medicare physician fee schedule. Approximately 80%-90% of RUC recommendations do not undergo further revision after being reviewed by CMS.
ASHA developed four procedures for diagnostic programming of the cochlear implant speech processor. Two of the procedures are for the initial diagnostic analysis of the cochlear implant, and two are for subsequent programming. They will be available for use in 2003.
Reimbursement Rates. An ASHA-led coalition submitted comments to CMS requesting the agency increase the reimbursement rate for outpatient cochlear implant surgery and associated procedures. The coalition consists of professional associations, consumer organizations, and cochlear implant manufacturers.
The coalition's comments on the proposed Medicare outpatient cochlear implant payment facilitated a 23% increase in the fee (to $19,280). This amount is for all costs associated with the procedure, with the exception of the physician professional fee and post-operative rehabilitative services, both of which are excluded from the Prospective Payment System (PPS). The increase became effective April 2002. While the reimbursement rates for cochlear implants and procedures have been increased under the proposed rule, they remain substantially below cost and are likely to continue to inhibit access to these devices by Medicare beneficiaries.
ASHA remains determined to ensure that Medicare payment levels do not create further barriers to access for cochlear implant services. As part of those efforts, ASHA continues to pursue modifications to CPT code 92510 for cochlear implant programming and aural rehabilitation to enable any audiologist to bill and receive payment directly from Medicare without physician supervision.
Conclusion
Three aspects of an audiologist's practice are riddled with confusion because of third-party payers' misunderstanding of the profession. The audiologists serving on the Health Care Economics Committee are committed to improving the status of the profession. ASHA will continue to advocate for procedure codes that best reflect the practice of audiology and reimbursement rates that reflect the true values of the procedures. Moreover, we will increase communication among the profession, payers, and employers so that audiology procedures are appropriately covered.
For More Information on ASHA (American-Speech-Language-Hearing Association), click here.
For More Information on COCHLEAR IMPLANTS, please visit the following three websites:
Advanced Bionics, MED EL
Cochlear
-----------------------------------
1CPT codes and descriptions are copyright 2001 American Medical Association.
2Section 1861 (ll)(ii)(1), Title XVIII of the Social Security Act
3Section 2070.3 of the Medicare Carriers Manual
4Section 1862 (a)(7), Title XVIII of the Social Security Act
5www.lmrp.net
6Bellis, T.J. (2002). When the brain can't hear: Unraveling the mystery of auditory processing disorders. New York: Pocket Books.

