Pennsylvania College of Optometry
Dean of the School of Audiology
Presented at the Scott Haug Foundation Retreat
Kerrville, Texas, October 2003
Editor's Note: I was very impressed by the information Dr. George Osborne delivered at the Scott Haug Foundation Retreat in Kerrville, Texas. I asked Dr. Osborne if we could present some of his ideas and opinions (below) on Audiology Online. I know this is a little unusual, and a little disjointed - that's my fault. Many of the issues below were adapted from Dr. Osborne's slide presentation. The presentation Dr. Osborne gave was thorough and thought provoking. Throughout this extrapolation, I have tried to present the "greatest hits version" to quickly disseminate this information to audiologists, to help them better understand where we came from, and how much further there is to go. Special thanks to Dr. Osborne.
---Dr. Douglas L. Beck, Audiologist, Editor-In-Chief.
*****************************************************
HISTORICAL NOTES:
1976: Raymond Carhart, Ph.D. - "...as long as either ASHA or clinical audiology are satisfied to accept only this definition as describing competence in clinical audiology [ccc from ASHA...and the Master's degree] the field cannot expect to be recognized as equal to professions that hold the doctorate as one of their inviolate requirements."
1976: Academy of Dispensing Audiologists (ADA) was created
Founders: Leo Doerfler, John Maher, John Balko, Norm Carmel,, Chauncey Hewitt, Mike Pollack, Roy Rowland, and Anthony Tsappis, 1st National Meeting - Cape Cod 1979, ADA represents "audiology practitioners."
The ADA gave birth to the Au.D. at its 1988 Education Conference in Chicago. ADA also created the Audiology Awareness Campaign.
"ADA is dedicated to leadership in advancing practitioner excellence, high ethical standards, professional autonomy, hearing technology, and sound business practices in the provision of quality audiological care."
1987: ASHA Panel on Future of Audiology
Participants were Drs. Lucille Beck, James Jerger, George Osborne, and Richard Talbot (moderator). The panel agreed that the profession needed change and that the future would find audiologists as:
Autonomous Profession
Doctoring Profession
Limited License Practitioners
Own Professional Organization
Enriched Curriculum
Direct Access for Patients
New Professional Structure
1988 - American Academy of Audiology (AAA) is created
Founded January 1988 - Houston, TX by Dr. James Jerger - 3 months after the ASHA Panel
30 Founders from all across the country. AAA is now (2003) 8,500 strong.
1988: ADA Chicago Conference on Education in Audiology - formed ad hoc committee that became AFA
1989: Audiology Foundation of America (AFA) is created - charged with transitioning audiology to a doctoring profession. The Au.D. is absolutely the result of the many years of hard work and unwavering focus of the AFA. AFA Founders include: David Cieliczka, David Citron, Leo Doerfler, David Goldstein, Angela Loavenbruck, George Osborne, Susan Whichard, and Tom Zachman.
Au.D. STATUS REPORT 2003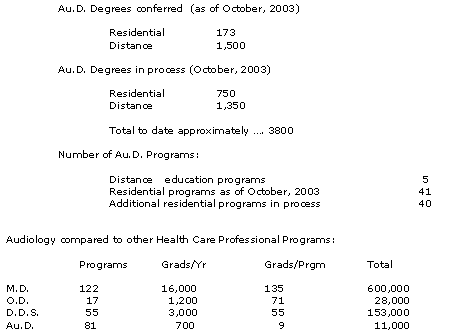
Clearly, we already have too many Au.D. programs! Although the marketplace will determine which programs survive, adding an additional 40 is going to create significant problems for our profession going forward. The smallest professional program class size I am aware of is 34. Small Au.D. programs will continue to be dependent upon their affiliation with and support by some "other" entity (SLP - allied health - etc.).
Use of Au.D. Title:
Don't embarrass your colleagues by inappropriate use of the title.
Never as a student. The title ("doctor") should be used only after you complete the degree. Au.D. (C) or Candidate is inappropriate.
Recommended uses upon completion of the degree:
George S. Osborne, Au.D.
Dr. George S. Osborne, Audiologist
Audiology's Greatest Challenge is to earn Limited Licensed Practitioner status, which will provide audiologists with limited Rights and Privileges of a Physician for those services the law recognizes they provide. Limited Licensed Practitioners are allowed Direct Access to Patients Without Physician Referral and the ability to Bill Directly for Services Using UPIN Number.
Limited Licensed Practitioners: (all are identifiable by a common designator)
Medicare reimburses five types of non-physician health care professionals classified as ''limited licensed practitioners''—optometrists (OD), dentists (DDS), oral and maxillofacial surgeons (DDS), podiatrists (DP), and chiropractors (DC)--as physicians when they furnish specific services for which the law considers them to be physicians."
Autonomous: Having the right or power of self-government, undertaken or carried on, without outside control. Existing or capable of existing, independently. Although all healthcare providers will be influenced by outside forces the intent of the ASHA panel was that decisions concerning the profession of Audiology should be made by audiologists and not by individuals from another profession.
Transitioning to the Au.D. means moving out of the Graduate School into Professional Schools. Doctoring Professionals earn a "First Professional Degree." The US Department of Education defines the following types of degrees:
Bachelor's Degree: A degree awarded by a postsecondary institution to a student who has completed at least four academic years of college-level work in an academic or occupation-specific field of study.
Master's Degree: A degree awarded by a graduate school or department to a person who has completed the full-time equivalent of at least one but not more than two years of work beyond the baccalaureate level.
Doctoral Degree: Any of numerous academic degrees awarded by universities and some colleges on completion of advanced graduate or professional studies in the humanities, the social sciences, the behavioral sciences, or the pure sciences beyond the master's level.
First Professional Degree: A degree awarded by an institution to an entry-level professional in certain occupational fields (medicine, dentistry, optometry, podiatry, etc), having a minimum of 2 years of pre-preparation and 4 years of professional training.
"Doctors" are trained in professional schools - not graduate schools. Audiology will eventually need to transition out of graduate schools, and into professional schools. Although this change will take many years, some programs have already made this move.
Changing the profession means changing graduation "Hood" colors. Doctoring professions hoods are usually a shade of green. This change has already been accomplished.
Education (Ed.D.) = Light Blue
Philosophy (Ph.D.) = Dark Blue
Medicine (M.D.) = Green
Optometry (O.D.) = Seafoam Green
Pharmacy (Pharm.D.) = Olive Green
Audiology (Au.D.) = Spruce Green
Changing the profession means changing our curriculum. This has been very difficult for some of our programs to grasp. Adding a couple of courses and renaming the CFY is not in keeping with the spirit of transition to a doctoring profession. As an example of a professional doctoring Au.D. curriculum the following information, which is specific to the PCO School of Audiology 4-year residential program, is an example of the direction in which I believe the profession needs to move. All "doctors" share a basic biomedical foundation and audiologists will need to gain access to that same information if we expect to be independent "doctors" on par with the dentist, physician, optometrist, etc.
Entrance Requirements:
Bachelors Degree or 90 Semester Hours
Audiology/Optometry Aptitude Test
Letters of Recommendation
Essay about why you want to be an Audiologist
On-Campus Interview to meet faculty, students, tour campus and clinic
Pre-Audiology Coursework
Pre-Audiology Coursework
Biology, General or Zoology (with labs)
Chemistry, General (with labs)
Chemistry, Organic (with labs)
Physics, General (with labs)
Microbiology or Bacteriology (with labs)
English Composition or Literature
Mathematics (College) or Calculus
Psychology
Statistics (Math, Biology or Psychology)
Actual Curriculum:
Module 1 - Molecular and Cellular Processes: biochemistry, molecular genetics, histology, anatomy, physiology, general pathology, immunology, and pharmacology (1st half of year 1)
Module 2 - Integrative Organ Systems and Disease: Histology, physiology, pathology, pharmacology, and clinical medicine. (2nd half of year 1)
Module 3 - Integrative Auditory Systems and Disease: Auditory Vestibular biology sequence (neurology, anatomy, histology, biochemical and physiologic conditions), auditory diseases, auditory disorders, and emergencies. (year 2 and 1st half of year 3)
Module 4 - Integrative Neuro-Auditory Sciences: head and neck anatomy, neuroscience, neuropathology, neuropharmacology, neuro-auditory disease, as well as human development. (years 1 thru 3)
Module 5 - Audiologic Principles and Management of Hearing/Balance Problems: Diagnosis, evaluation, and treatment (rehabilitation), including amplification. (years 1 thru 3)
Module 6 - Principles and Practice of Audiologic Medicine: Professional practice both on and off campus (affiliated local clinics) from observation to clinical activities. 908 hours, personal and professional career planning, intro to the Health Care System, Practice development and management. (years 1 thru 3)
Module 7 - Clinical Problem Solving: literature searching, evaluation of data, integration of basic science into clinical applications. (years 1 thru 3)
Module 8 - Clinical Externships: placements to include: private practice, hospital based site, medical practice site and other options. (~3100 hours structured experience.) (last ½ of yeaar 3 and year 4)
Module 9 - Electives and Scholarship (research w or w/o M.A. or Ph.D.) - 36 specialty areas in audiology to choose from. (years 2-4)
Curriculum Summary: 1200 hours didactic, 570 hours laboratory, 80 hours clinical problem solving, and 3200 hours of patient care
Patients need Direct Access to Audiologists: At the present time too many healthcare dollars are spent "in search of audiologic services" and audiologists do NOT receive the monies for the services they provide. A few examples of where the money goes:
Audiology's Greatest Opportunity. Congressional Action is necessary and the time is right NOW! All audiologists and their patients should write their congressional representatives to support these bills.
HR 2821 - Hearing Health Accessibility Bill
- Introduced in House of Representatives on July 22, 2003
HR 2821 will allow Medicare beneficiaries the option of going directly to a qualified audiologist for hearing and balance diagnostic tests.
SPONSORS: Rep. Jim Ryun (R-KS) and Rep. Lois Capps (D-CA). Also Reps. Cass Ballenger (R-NC), Carolyn McCarthy (D-NY), Martin Meehan (D-MA), George Miller (D-CA), Jim Ramstad (R-MN), Fred Upton (R-MI), Robert Wexler (D-FL) - more being added daily
S 1647 - Hearing Health Accessibility Bill - Senate companion to HR 2821 (exact same verbiage) was introduced September 24, 2003
SPONSORS: - Senator Ben Campbell (R-CO) and Senator Tim Johnson (D-SD) - others are signing on daily,
The Structure of our Profession needs to change: Audiology organizations have been bidding for the same members in a structure that is Horizontal. We need to think Vertically and work together to create a profession that provides for audiologists with similar interests and responsibilities to communicate with each other and the entire profession. A vertical structure may look something like the following:
Umbrella Association - AAA
State Affiliates - (underway)
Practitioner Academy - ADA, ARA, EAA, etc. (to represent different specialty areas)
Student Organization - NAFDA
Accreditation Commission for Audiology Education - ACAE (in process)
Academic Academy - CAuDP (to represent academic programs)
The Vocabulary of a Profession - it is important that audiologists recognize that doctoring professions already have very specific definitions for many terms we need to integrate into our vocabulary.
Student: this is easy - a student is a student.
Clerkship: a clinical rotation usually within the training institution
Externship: a clinical rotation traditional outside of - but related to - the training institution. Very common 3rd and 4th year placements in various practice settings. The VA - Medical Centers - Qualified Preceptors. Student, Clerkship, and Externship is where it ends for us at this time.
The following terms do not apply to audiology today and we should be careful not to use them inappropriately.
Residency: The period of training in a specific specialty. It occurs after graduation and its length may vary from 3 to 7 years, depending upon specialty.(ENT - Pediatrician - Orthodontist - etc.)
Intern: The term ''intern'' is used to identify doctors in their first year of residency.
Board-Certification: traditionally is reserved for a doctor who has successfully completed a nationally recognized specialty examination after finishing a residency program.
Fellow: The term ''fellow'' is usually reserved for doctors in subspecialty programs (versus residents in specialty programs) or in Graduate programs that are beyond the requirements for eligibility for board certification in the specialty (i.e. Ph.D. in Biochemistry).
Audiology is alive and well! However, there is still lots of work to do. - But in my opinion Audiology is the single best option to medicine or any other healthcare profession today. Our challenge is to educate the pre-healthcare advisors across the country (there are 1200 of them) about audiology so that talented young "future doctors" are aware of the opportunities that audiology offers. We must concentrate on graduating increasing numbers of highly qualified audiologists to meet the growing demand for hearing and balance services.
Current State of Audiology
October 27, 2003
Related Courses
1
https://www.audiologyonline.com/audiology-ceus/course/understanding-privilege-for-healthcare-professionals-36096
Understanding Privilege, for Healthcare Professionals
Systems of privilege have created a wide division of inequality. This course will help hearing care professionals identify their privilege and determine how to make a difference in their places of employment.
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Understanding Privilege, for Healthcare Professionals
Systems of privilege have created a wide division of inequality. This course will help hearing care professionals identify their privilege and determine how to make a difference in their places of employment.
36096
Online
PT60M
Understanding Privilege, for Healthcare Professionals
Presented by Esther Clervaud, EdS
Course: #36096Level: Intermediate1 Hour
AAA/0.1 Intermediate; ACAud inc HAASA/1.0; BAA/1.0; CAA/1.0; IACET/0.1; IHS/1.0; NZAS/1.0; SAC/1.0
Systems of privilege have created a wide division of inequality. This course will help hearing care professionals identify their privilege and determine how to make a difference in their places of employment.
2
https://www.audiologyonline.com/audiology-ceus/course/creating-leadership-in-audiology-through-37632
Creating Leadership in Audiology Through a Mentoring Circle
There are so many components to quality patient care that it is challenging to “master” them all. What if you could come together with other professionals who possess knowledge or experience that could help you or your practice? There are a number of veteran audiologists as well as rising professionals who have wisdom, qualifications, narratives, and unique journeys to share. The purpose of this talk is to rethink the traditional mentor/mentee vertical relationship and explore collaboration in the form of circle…where all professionals, regardless of age or experience, learn from each other.
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Creating Leadership in Audiology Through a Mentoring Circle
There are so many components to quality patient care that it is challenging to “master” them all. What if you could come together with other professionals who possess knowledge or experience that could help you or your practice? There are a number of veteran audiologists as well as rising professionals who have wisdom, qualifications, narratives, and unique journeys to share. The purpose of this talk is to rethink the traditional mentor/mentee vertical relationship and explore collaboration in the form of circle…where all professionals, regardless of age or experience, learn from each other.
37632
Online
PT60M
Creating Leadership in Audiology Through a Mentoring Circle
Presented by Natalie Phillips, AuD
Course: #37632Level: Introductory1 Hour
AAA/0.1 Introductory; ACAud inc HAASA/1.0; AHIP/1.0; ASHA/0.1 Introductory, Related; BAA/1.0; CAA/1.0; Calif. SLPAB/1.0; IACET/0.1; IHS/1.0; NZAS/1.0; SAC/1.0
There are so many components to quality patient care that it is challenging to “master” them all. What if you could come together with other professionals who possess knowledge or experience that could help you or your practice? There are a number of veteran audiologists as well as rising professionals who have wisdom, qualifications, narratives, and unique journeys to share. The purpose of this talk is to rethink the traditional mentor/mentee vertical relationship and explore collaboration in the form of circle…where all professionals, regardless of age or experience, learn from each other.
3
https://www.audiologyonline.com/audiology-ceus/course/unlocking-more-time-for-patients-41986
Unlocking More Time for Patients
On busy days in clinic have you ever wished for more time? Learn about Phonak products and processes across the patient journey that free up valuable clinic time for providers as well as reduce the time patients need to spend in the office for follow-up care.
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Unlocking More Time for Patients
On busy days in clinic have you ever wished for more time? Learn about Phonak products and processes across the patient journey that free up valuable clinic time for providers as well as reduce the time patients need to spend in the office for follow-up care.
41986
Online
PT60M
Unlocking More Time for Patients
Presented by Rochelle Wong, AuD
Course: #41986Level: Introductory1 Hour
AAA/0.1 Introductory; ACAud inc HAASA/1.0; AHIP/1.0; BAA/1.0; CAA/1.0; IACET/0.1; IHS/1.0; NZAS/1.0; SAC/1.0; TX TDLR, #142/1.0 Manufacturer
On busy days in clinic have you ever wished for more time? Learn about Phonak products and processes across the patient journey that free up valuable clinic time for providers as well as reduce the time patients need to spend in the office for follow-up care.
4
https://www.audiologyonline.com/audiology-ceus/course/core-topics-for-audiology-assistants-37123
Core Topics for Audiology Assistants
This course includes one hour of content on each of the following topics: 1) ethical concepts and decision-making; 2) universal safety precautions, including the Occupational Safety & Health Administration's (OSHA) bloodborne pathogens standard, and 3) patient confidentiality and the Health Insurance Portability & Accountability Act (HIPAA).
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Core Topics for Audiology Assistants
This course includes one hour of content on each of the following topics: 1) ethical concepts and decision-making; 2) universal safety precautions, including the Occupational Safety & Health Administration's (OSHA) bloodborne pathogens standard, and 3) patient confidentiality and the Health Insurance Portability & Accountability Act (HIPAA).
37123
Online
PT180M
Core Topics for Audiology Assistants
Presented by James W. Hall III, PhD, Kathleen Weissberg, OTD, OTR/L, Amit Gosalia, AuD
Course: #37123Level: Introductory3 Hours
AAA/0.3 Introductory; ACAud inc HAASA/3.0; AHIP/3.0; ASHA/0.3 Introductory, Related; BAA/3.0; CAA/3.0; Calif. SLPAB/3.0; IACET/0.3; IHS/3.0; Kansas, LTS-S0035/3.0; NZAS/3.0; SAC/3.0
This course includes one hour of content on each of the following topics: 1) ethical concepts and decision-making; 2) universal safety precautions, including the Occupational Safety & Health Administration's (OSHA) bloodborne pathogens standard, and 3) patient confidentiality and the Health Insurance Portability & Accountability Act (HIPAA).
5
https://www.audiologyonline.com/audiology-ceus/course/engaging-deaf-professionals-in-ehdi-37893
Engaging Deaf Professionals in the EHDI System
The course explores ways to draw on Deaf professionals' expertise in working with families of Deaf and hard of hearing infants and young children. A highlight of Deaf people's knowledge, experiences, expertise, and contributions in the EHDI (Early Hearing Detection and Intervention) System will be discussed.
auditory, textual, visual
129
USD
Subscription
Unlimited COURSE Access for $129/year
OnlineOnly
AudiologyOnline
www.audiologyonline.com
Engaging Deaf Professionals in the EHDI System
The course explores ways to draw on Deaf professionals' expertise in working with families of Deaf and hard of hearing infants and young children. A highlight of Deaf people's knowledge, experiences, expertise, and contributions in the EHDI (Early Hearing Detection and Intervention) System will be discussed.
37893
Online
PT60M
Engaging Deaf Professionals in the EHDI System
Presented by Sheri Farinha, MA, Julie Rems Smario, EdD
Course: #37893Level: Intermediate1 Hour
AAA/0.1 Intermediate; ACAud inc HAASA/1.0; AHIP/1.0; ASHA/0.1 Intermediate, Related; BAA/1.0; CAA/1.0; Calif. SLPAB/1.0; IACET/0.1; IHS/1.0; IL EITP/1.0; Kansas, LTS-S0035/1.0; NZAS/1.0; SAC/1.0
The course explores ways to draw on Deaf professionals' expertise in working with families of Deaf and hard of hearing infants and young children. A highlight of Deaf people's knowledge, experiences, expertise, and contributions in the EHDI (Early Hearing Detection and Intervention) System will be discussed.

