Abstract: Electroneuronography (ENoG) involves electrical stimulation of the facial nerve at or near the stylomastoid foramen and the subsequent measurement and interpretation of the motoric response, as recorded at or near the nasio-labial fold. The ENoG test is the only 'relatively objective' measure of facial nerve integrity.
ENoG compares the neurophysiologic response of the normal side to the abnormal side in order to help determine whether surgical intervention is recommended and to determine the probable prognosis with regards to the clinical presentation and case history.
Introduction:
Facial nerve paralysis is a debilitating condition (1). Patients with facial nerve disorders are often devastated due to the emotional and psychological impact of facial disfiguration and the subsequent physical limitations and difficulties associated with speaking, drinking, eating, and facial expression secondary to the disorder. Socialization and community participation is extraordinarily limited and difficult for many of these patients.
The evaluation of facial nerve viability is critically important part to management of facial nerve disorders. Depending on the outcome of the ENoG evaluation, physicians may choose to 'watch and wait', or they may elect surgical intervention. Surgical intervention is by no means trivial, and it's utility is often directly determined based on the ENoG evaluation.
Patients with facial nerve disorders have a variety of etiologies including; Bell's Palsy (BP), iatrogenic (surgically induced) injury, trauma to the temporal bone secondary to motor vehicle accidents (MVA), otitis media, herpes zoster oticus, multiple sclerosis, Melkersson-Rosenthal syndrome, mastoiditis, mumps, chicken-pox, Gilllain-Barre syndrome, central nervous system disorders (i.e., stroke), glomus jugulare, meningioma, facial nerve neuroma, and others (2).
It is important that the patient experiencing facial nerve palsy maintain adequate eye-care. As the ipsilateral eyelid may not function appropriately, it is important to have the patient use articificial tears, eye protection (such as a patch or sunglasses to keep dirt and debris out of the eye) and it is often a good idea to tape the eyelid closed while sleeping. Although these cautions are typically addressed by the physician, the audiologist might also underline the importance of these recommendations.
Electroneuronography (ENoG) is the test performed by audiologists to evaluate the integrity of the facial nerve. ENoG is within the scope of practice of audiologists, based on both AAA and ASHA Scope of Practice statements (3, 4). Audiologists have been evaluating facial nerve function for many decades.
Perhaps the earliest assessment of facial nerve function by audiologists began with measurement of the acoustic reflex during immittance test batteries.
Alternative tests of facial nerve function:
Many other tests of facial nerve function have been, and continue to be used. These include; the Hilger test, electromyography, acoustic reflex testing (5), evoked accelerometry, antidromic nerve potentials, MRI and CT radiologic evaluations, maximal nerve stimulation tests, minimal nerve stimulation tests, transcranial magnetic stimulation (6), blink reflex tests (7) and others.
House-Brackmann Facial Grading Scale:
The most commonly used facial nerve grading scale is the House-Brackmann (HB) scale (8). The HB scale is used to approximate the quantity of volitional motion the patient has based on their clinical facial presentation. Although the HB scale is based on clinical observation, and variation among observers exists, the HB scale allows us to grossly describe the characteristics and degree of facial nerve motion using a subjective analysis scale, which is easily and reliably applied.
The HB scale has six grades. Each grade is reported as a fraction (i.e., 1/6 = grade one). A grade one presentation is perfectly normal. Grade two is a slight, or mild weakness. Grade three is a moderate weakness with good (normal) eye closure. Grade four is a moderate weakness with no volitional eye closure. Grade five is a severe weakness. Grade six is a total facial paralysis.
In some respects, we can say that only grade six (6/6) presentations require EnoG testing. That is, the purpose of the test is to determine whether or not the facial nerve is neurophysiologically intact. Therefore, if the patient has any volitional motion (as would be evident with grades one through five) the facial nerve is indeed intact. Nonetheless, it is certainly useful to chart the progress of facial nerve disorders via ENoG even in cases with grades two through five presentations.
Additionally, it is sometimes rather difficult to discern if an apparent grade five presentation is indeed a grade five, of if the extremely limited motion is actually from the masseter, or from musculature motion from the contralateral (normal) side. ENoG evaluation allows a subclinical analysis which may impact medical or surgical decisions. Similarly, once a visible improvement is apparent regarding facial nerve reanimation, further ENoG testing provides little information.
Anatomy and Physiology:
There are twelve pairs of cranial nerves. The two cranial nerves which are of most interest to the audiologist are the seventh nerve (the facial nerve) and the eighth nerve (the vestibulocochlear nerve). Our discussion here will be limited to the seventh nerve.
Each facial nerve has some 10,000 fibers (9). About 2/3rds of the fibers are motor fibers, about 1/3rd are sensory. The sensory portion of the facial nerve is the nervus intermedius. It is estimated that only half of the motor fibers need to be functioning for the patient to have essentially normal facial nerve function.
As the facial nerve exits the brainstem, it traverses the cerebellopontine angle (CPA) to the medial end of the internal auditory canal (i.e. the porus acousticus). Progressing distally to the stylomastoid foramen, the facial nerve includes the labyrinthine segment, the tympanic segment, the pyramidal bend, the mastoid portion and finally the stylomastoid foramen, where the nerve exits the skull and is readily positioned within the parotid gland. Interestingly, most traumatic injuries, such as temporal bone fractures secondary to motor vehicle accidents, are reported to be within the labyrinthine segment of the facial nerve.
As the main trunk of the facial nerve enters the parotid region, it divides into two main divisions. The superior division of the nerve divides into three sections; temporal, zygomatic and buccal divisions. The inferior division of the nerve divides into the buccal, mandibular and cervical branches (10).
Bell's Palsy:
Bell's Palsy (BP) is probably the single most common etiology of facial nerve disorders. The incidence of BP in the general population is about 15 cases per 100,000 population (0.00015%). BP has a familial tendency, although it is certainly not predictable across families or generations. BP will recur in 5 to 10 percent of patients.
The time from onset of BP to total, unilateral facial paralysis is usually about 24 to 48 hours. Spontaneous recovery is common, and usually occurs for some 75 to 80 percent of all patients, in about 3 to 4 weeks. Across all BP patients, 15 to 20 percent maintain a lifelong residual weakness following resolution of the BP. About 5 percent of all patients have permanent weakness worse than HB grade 4/6.
The etiology of BP is unknown. Viral neuropathy, bacterial infections, genetics, environmental and many other causes have been suggested. It is likely that there are a number of reasonable etiologies. Various treatment options are available for the BP patient including; surgical intervention, 'wait and watch' approaches, acyclovir treatment (11) and other medical options.
Wallerian Degeneration:
When BP and other facial nerve injuries occur, it takes some 72 hours for Wallerian Degeneration (WD) to occur. WD is the process of denervation of the neural fibers and it is a relatively slow process (12). WD occurs from proximal to distal anatomy.
If we were to test a patient with an HB grade six (1/6) facial presentation, one hour after the onset of BP, it is likely we would get a normal ENoG result. That is, because the facial nerve hasn't completed WD, the fibers are physiologically intact, although non-functional volitionally. The resultant ENoG would be a false negative if the test was performed prior to complete WD. In essence, the test would quantify the physiologic viability before the complete damage has been done. Therefore, it is important to wait approximately 72 hours before performing the first ENoG to allow the nerve to undergo complete WD. Results obtained prior to that are essentially non-interpretable as they potentially measure the status of the nerve before the damage has plateaued.
Timing the ENoG Test:
As noted above, Wallerian degeneration impacts the first ENoG test session. Typically, testing is delayed until 72 hours post-onset of paralysis. However, at the other end of the timing window is the 21 day maximum. Specifically, if ENoG and subsequent surgical intervention are delayed past a 21 day post-onset window, the test and possible surgical intervention are of questionable value.
In essence, the ENoG should be performed for the first time at about 72 hours post-onset and again at 3 to 5 day intervals until a trend and confirmation can be obtained. If the trend and confirmation are determined prior to 21 days post-onset, surgical intervention may be an option. If the ENoG is not obtained prior to 21 days post-onset, it is of little clinical use. Specifically, an ENoG obtained 4 weeks after onset of facial paralysis is difficult, if not impossible, to interpret.
3 Types of Facial Nerve Injury:
Fisch has used three terms to describe the three primary types of facial nerve injury (13). These are; neuropraxia, neurotmesis and axonotmesis. It is important to note that ENoG cannot differentiate between neurotmesis and axonotmesis.
Neuropraxia. Neuropraxia is the most common finding associated with BP. In this situation, the patient experiences paralysis without peripheral nerve degeneration. The ENoG demonstrates a normal or reduced response. The nerve fibers and the sheath are anatomically intact, however, they are not responsive to volitional commands.
Neurotmesis. Neurotmesis is the worst possible outcome. The ENoG will demonstrate essentially no response (i.e. flat line). Neurotmesis represents a total anatomic separation with a very poor prognosis (14).
Axnotmesis. Axonotmesis has been described as an inner nerve fiber disruption despite an intact outer casing (epineurium). The ENoG will show no response (i.e., flat line). An analogy to help describe axonotmesis is when an insulated cable with thousands of wires inside has been manually bent back and forth. Many of the internal wires will snap and separate, despite intact, external insulation.
RECORDING TECHNIQUES, ANALYSIS STRATEGIES and TROUBLE-SHOOTING:
At first glance, ENoG would appear to be a relatively simple electrophysiologic measurement technique. The stimulus electrode is placed directly over the facial nerve across a broad anatomic region. The electrodes located in the nasolabial fold (base of the nose to the corner of the mouth) do not require precise placement. The amplitude of the response is, by auditory electrophysiology standards, gigantic, often exceeding 2000 microvolts (over 2 millivolts).
A protocol for recording ENoG is summarized in Table 1. Consistent with typical clinical protocol, the procedure is explained to the patient at the outset. Most patients undergoing ENoG readily agree to the discomfort of electrical stimulation since they are very troubled by facial nerve dysfunction and want to do whatever they can to help discover the cause and impact the effective treatment of their facial nerve disorder. Even children rarely protest when the ENoG procedure is explained and measurement begins.
Naturally, the wise clinician will take care to use terms which do not alarm patients. For example, we recommend instructions similar to 'We will present a little stimulation to the nerve that goes to your face', rather than, 'We are going to give you an electrical shock to test your facial nerve.'
Prior to beginning the ENoG procedure, as is customary with all electrophysiologic diagnostic tests, the clinician should carefully assemble necessary supplies (e.g., tape, skin abraiding material, conducting paste, electrodes), prepare the skin for stimulus and response electrode application, and check interelectrode impedance for all electrode combinations.
The fundamental principle in ENoG analysis, is a quantified comparison of the distal facial nerve response comparing ipsilateral to contralateral sides. Therefore, ENoG measurement should be conducted using the same stimulation and recording technique for each side.
Conventionally, the 'good' side is stimulated first. Bipolar electrical stimulation (in milliamperes, mA's) is delivered to the region at the base of the ear, presumably where the facial nerve trunk exits the stylomastoid foramen in the mastoid and then courses anteriorly through the parotid gland and towards the face.
Note in Figure 1 that the negative (black) stimulation electrode is located just behind the earlobe (remember 'black is back'). Avoid inching the stimulating electrodes anteriorly ahead of the ear to enhance detection of an ENoG response, as the likelihood of inadvertently stimulating a masseter muscle response (and mistaking it for a facial nerve response) is increased as the stimulator moves anterior. Typically, audiologists will sample several stimulation locations in this region to verify the largest possible response is measured. As a rule, the optimal response is recorded with the two electrodes positioned parallel to the nerve (along a horizontal line from just behind to just in front of the earlobe).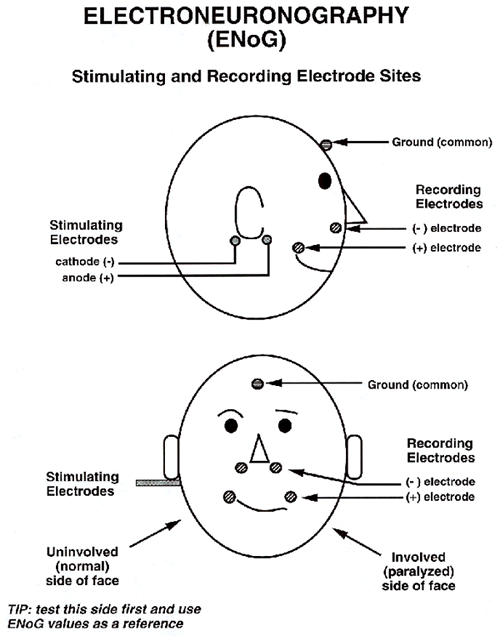
If you suspect the response is contaminated with masseter response, or may indeed be masseter response, there are two things to consider. 1- If the response is 'triphasic', it may well be the masseter, and 2- observe the patient's mandible closely. If the jaw is moving in rhythym with the stimulation, it is likely that the response includes some/all masseter response, rather than the desired, isolated, facial nerve response.
The measurement electrodes are located on the nasolabial fold (see Figure 1), ipsilateral to the side of stimulation. Be sure to check inter-electrode impedance for each side (less than 5000 ohms is desirable) and verify that the ipsilateral electrodes are plugged into the electrode box/strip prior to stimulation. Measurement electrodes may be fixed (disc electrodes taped to the base of the nose and corner of the mouth), or the electrodes (within a bar) may be placed in these locations by the audiologist and systematically moved for subsequent stimulations in an attempt to maximize the response. Two measurement electrodes may also be placed near the forehead, outside the eyebrows. Then, either a two channel or two single channel ENoG recordings can be made from two branches of the facial nerve. This approach is often taken during intraoperative monitoring of facial nerve function.
ENoG stimulation must be efficiently and effectively delivered. That is, we desire to test with the lowest possible stimulus which produces a maximal response. If accomplished, a further increase in stimulus intensity will not yield an increase in response amplitude. Although the literature does not appear to offer a maximal stimulus level, good clinical protocol suggests there is no reason to stimulate above 40 mA. The intensity level which first produces a maximum response varies from patient-to-patient, and even from side-to-side within a patient. Usually, however, the stimulus intensity must exceed 20 to 25 mA before a supramaximal level is reached. Symmetry in the amplitude level from one side to the other is not important. Rather, it is critically important to assure that the largest possible facial nerve response is obtained from each side. Because the ENoG is such a large physiologic response (often exceeding 1000 mVolts), and few (1 to 10) stimulus presentations are needed to average a response, an experienced audiologist can confidently find the supramaximal response in several minutes. Examples of normal and abnormal ENoG waveforms are illustrated in Figure 2.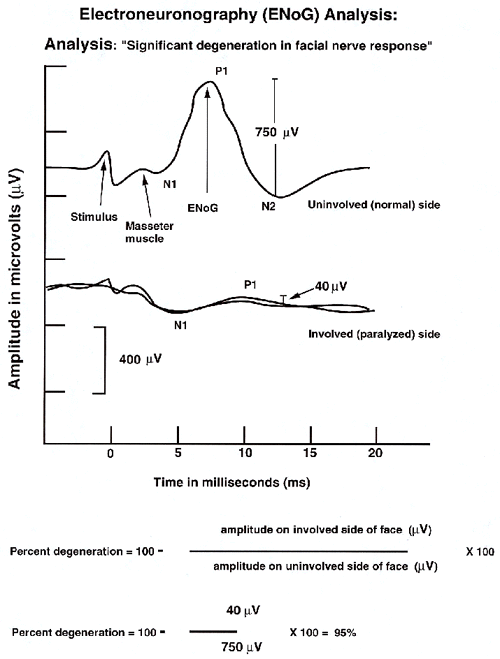
Despite the size of the ENoG response, and the appearance of simplicity in measurement as outlined above, problems can and will arise clinically with patients with suspected facial nerve dysfunction. The most common measurement problems and some helpful solutions are summarized in Table 2. Robust and reliable responses are unequivocal.
There are, clearly, many possible explanations for a suboptimal response. Some can be quickly and effectively addressed by slight modification in test protocol, but others (e.g., obesity) may be difficult to resolve in a timely fashion.
Considerable clinical experience and judgement is required to regularly record quality ENoG responses and to avoid errors in interpretation. One must bear in mind the serious consequences of errors in interpretation.
If a response is mistakenly identified on the involved side, that is artifact or perhaps masseter muscle is accepted as a facial nerve response, this 'false-positive' error can lead to a decision to withhold potentially effective surgical therapy. If, on the other hand, the audiologist incorrectly concludes there is no ENoG (perhaps due to measurement problems summarized in Table 2), then potentially irreversible and damaging therapy (e.g., surgery) may be implemented for a patient who, in fact, has a normal facial nerve response.
ANALYSIS OF ENoG DATA:
Latency is not critically important for ENoG. Typical N1 latencies are less than 6 millisconds. Of primary importance is amplitude. As mentioned earlier, the 'normal' side is evaluated first, the 'abnormal' side is tested second.
The result of the ENoG is reported as a percentage. In essence, the amplitude of the normal side is the denominator and the amplitude of the weak side is the numerator. Therefore, if the weak side amplitude is 1240 microvolts and the normal side has an amplitude of 3265 microvolts, the weak response is reported as:
1240 microvolts (weak side)
_________________________ = 0.379 = 38 percent response.
3265 microvolts (normal side)
Alternatively, some locations report the percentage in terms of 'denervation', indicating the percentage of neural fibers which are no longer responding. Therefore, the 38% response indicated above, would be considered a 62% 'denervation'. Either protocol is fine, as long as the audiologist and the physician use consistent terminology!
Any response greater than ten percent (or conversely, a 90% denervation) is consistent with spontaneous recovery and may trigger the 'watch and wait' response from the physician. A response of less than ten percent may suggest a surgical alternative.
It is a good clinical protocol to test the patient approximately every 3 to 5 days until a plateau (or direction) can be determined.
ILLUSTRATIVE CASE ONE:
MRN is a 61 year old male. He had been in the office previously for evaluation of his noise induced, SN loss. His last office visit was 18 months ago. MRN presents today with right facial paralysis.
He stated that after he woke up four days ago, he noted peculiar sensations while shaving, and he noted he couldn't drink his coffee without 'droolling all over the place'. His wife told MRN to go to the ER, as she thought he had had a stroke. He said he felt fine, he assumed he had 'slept on it funny' and went to work. That evening his wife noticed that when he was sleeping, his eyelid did not close all the way. The second morning, he went to his primary care physician's (PCP) office . The physician diagnosed 'probable Bell's Palsy' and referred MRN to the Audiology Department for additional work-up.
MRN presented to the audiologist with a grade six (6/6) H-B facial weakness. The audiology work-up included the comprehensive audiometric evaluation and complete immitance battery. The audiogram was consistent with the test obtained 18 months ago (symmetric, 55 dB SN loss, excellent word recognition scores), normal tympanograms AU and normal ipsi lateral reflexes on the left ear. Ipsilateral reflexes were absent in the right ear. With the stimulus in the right ear, the acoustic reflex was recorded from the left ear (contralateral response). With the stimulus in the left ear, there was no response obtained from the right ear. Tuning fork tests were consistent with the audiometric findings. A midline Weber response was obtained and air conduction was greater than bone conduction via the Rinne.
The above findings are classic findings consistent with Bell's Palsy. Therefore, the electroneuronography (ENoG) test was ordered and completed to obtain a 'baseline' response.
The left side response was obtained first. The maximal stimulus (40 milliamperes) was required to obtain a 'plateau' response. The response obtained from the left side was 2140 microvolts (uV). Using the same stimulation and recording paprameters on the right side, the response obtained was 965 uV. The response was obtained and recorded from each side three times. Therefore, the response of the right side was determined to be (965/2140) 45% of the normal side, also referred to as a '55% denervation'. The responses were consistent with neuropraxia and BP.
The audiologist instructed the patient to use artificial tears to keep the eye moist and lubricated and to protect the eye with glasses/sunglasses during all waking hours as the normal 'blink' response, which protects the eye from debris and insult, was not functioning. Additionally, the audiologist suggested that the eyelid be gently taped closed (with an adhesive tape) during sleep, to protect the eye. MRN was scheduled for the next ENoG four days later. A report of the audiologist's findings was sent to the PCP.
During the second office visit, MRN's facial paralysis was again determined to be a grade six. Although the audiogram was not repeated, acoustic reflexes were repeated. The left and the right ipsilateral responses were present. The contralateral responses were present. The second ENoG showed the left amplitude at 2310 uV, and the right side was determined to be 1405 uV's. The response was determined to be 61% of the normal side, or 39% denervated. A follow-up (third) visit was scheduled four days later. An audiology report was sent to the PCP.
At the third visit, the audiologist noted that the facial presentation had improved to a grade three. Volitional eye closure had returned. The audiologist told the patient to discontinue the previously recommended eye-care protocols. Acoustic reflexes were again tested and were determined to be present via ipsi an contralateral pathways. The ENoG test revealed the left side amplitude of 2275 uV. The right side had improved to 1885 uV. The response was determined to be 83% of the normal side. The patient was released from additional ENoG tests, a report was sent to the PCP and the patient was instructed to follow-up with the PCP weekly, until complete resolution of the BP had occured, some two weeks later.
ILLUSTRATIVE CASE TWO:
The ENT service requested a bedside consult on patient TRW. TRW had been involved in an MVA (motor vehicle accident) seven days prior. TRW had been ejected through the windshield at a high rate of speed. TRW suffered multiple facial lacerations, a variety of broken bones (collarbone, ribs, pelvis) and a collapsed lung.
At the time of the initial consult, TRW was conscious and was able to respond to commands. Both sides of his face appeared puffy and swollen. His right blink reflex was absent. The left blink reflex was intact.
The audiologist and the ENT resident reviewed the chart. It was determined that the patient was on muscle relaxants and significant facial edema was present. Therefore, ENoG testing was deferred until 24 hours after muscle relaxants were discontinued, and until the apparent swelling was reduced. A facial grading was deferred.
Three days later, the patient reported he could not hear out of the right ear. A bedside audiogram was obtained. The audiogram demonstrated a mild SN loss in the left ear, no responses were obtained in the right ear. Bedside screening tympanometry confirmed intact and mobile tympanic membranes AU (type A).
The right ear was diagnosed with profound SN loss.
The left side ENoG response was obtained. The left side required a stimulus of 35 milliamperes to obtain a plateau response of 2800 uV. This response confirmed the muscle relaxants were indeed not 'on board', and also demonstrated that the edema was no longer a prohibitive factor in obtaining the ENoG. The right response was not repeatable nor was it apparent (a.k.a. 'flatline'). A report was sent to the ENT service.
A second ENoG was obtained three days later (13 days post-insult) demonstrating essentially the same response pattern. A report was sent to the ENT service. A CT with contrast was ordered. The CT scan showed a longitudunal fracture across the right temporal bone.
A combined middle fossa-mastoid facial nerve decompression was scheduled for the next day. Intraoperative monitoring of the facial nerve was obtained throughout the surgery. General anesthesia without muscle relaxants was employed. The otologist/surgeon determined the fracture had severed the facial nerve at the geniculate ganglion. A microscopic re-anastamosis was obtained. Intraoperative monitoring revealed that when the distal segment of the nerve was stimulated, a reduced but repeatable response was obtained at the orbicularis oris, confirming physiologic facial nerve integrity.
The patient awoke with a grade six presentation. The facial nerve slowly regained limited function. At 8 months post-op, a grade four result was obtained. At one year post-op, a grade three result was obtained. The patient has maintained a grade three function for two years. This is not likely to improve.
CONCLUSION:
ENoG is an extremely important test within the audiologist's scope of practice. Surgical decisions are sometimes based on ENoG results, and this helps underscore the importance and the weighting given this test by our surgical colleagues.
We strongly advise those who intend to record ENoG clinically to gain experience with supervision prior to providing this important clinical service, and then to proceed cautiously and deliberately. Training for ENoG is sometimes very lengthy as individual offices may go weeks, months or years between presenting patients.
Nonetheless, clinical training in this protocol should receive the same rigorous thought, study and practice as does intraoperative monitoring.
REFERENCES:
1. Jackson, C.G., von Doersten, P.G.: The Facial Nerve. Current Trends in Diagnosis, Treatement and Rehabilitation. Med Clin North Am., 83:1, 179-195. Jan. 1999
2. Beck, D.L., Benecke, J.E., Electroneurography: Electrical Evalustion of the Facial Nerve. J. Am. Acad. Audiol, 4: 109-115 (1993).
3. American Speech,Langauge, Hearing Association. Scope of Practice in Audiology. By the Ad Hoc Committee on Scope of Practice in Audiology. See https://www.asha.org/librrary/scope_aud.htm (online Dec. 2000).
4. American Academy of Audiology. Audiology: Scope of Practice Position Statements. See https://www.audiology.org/Pages/default.aspx (online Dec. 2000).
5. de Bisschop, G., Sarabian, A., de Bisschop E., Sarabian N.: Selection of electrophysiological investigations for diagnosis in idiopathic facial palsy. Twenty years experience in an ENT department. Rev Laryngol Otol Rhinol (Bord) , 119:2, 75-85. 1998.
6. Rimpilainen, I., Eskola, H., Laippala, P., Karma, P.: Prognositication of Bell's Palsy using transcranial magnetic stimulation. Acta Otolaryngol Suppl, 529, 111-115. 1997.
7. Kimura, M. , Nakagawa, I, Miimai. H., Hamada, H, Sakai, A., and Yasuuji, M.: Evaluation with blink reflex of bilateral facial palsy. Masui, 49:2, 159-162. Feb. 2000.
8. House, J.W. Brackmann, D.E.: Facial Nerve Grading System. Otolaryngol Head Neck Surg 93:146-147. 1985.
9. Hughes, G.B., Josey, A.F., Glasscock, M.E., Jackson, C.G., and Ray, W.A. : Clinical electroneurography: Statistical analysis of controlled measurements in twenty-two normal subjects. Laryngoscope, 91, 1834-1846 . 1981.
10. Beck, D.L.: Facial nerve electrophysiology: Electroneurography and facial nerve monitoring. Seminars in Hearing. 14:2 123-133. May, 1993.
11. Peiterwsen, E.: Bell's Palsy treated with Acyclovir (comment). Ugeskr Laeger, 159:14 2105. March 1997.
12. Bendet, E., Vajtai, I., Maranta C., Fisch, U.: Rate and extent of early axonal degeneration of the human facial nerve. Ann Otol Rhinol Laryngol, 107:1, 1-5. January, 1998.
13. Fisch, U. : Maximal nerve excitability testing vs. Electroneuronography. Arch Otolaryngol 106:352-357. 1980.
14. Cai, Z., Yu, G., Ma, D., Tan, J., Yang, Z., Zhang, X.: Experimental studies on traumatic facial nerve injury. J Laryngol Otol, 112:3 243-247. March 1998.
ACKNOWLEDGEMENT:
This article was originally published in The Hearing Journal, Vol 54, No 3, March, 2001. The article has been re-edited and is presented here for educational purposes with the permission of The Hearing Journal and its publisher, Lippincott Williams & Wilkins.



